- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 42(4); 2018 > Article
-
ResponseResponse: Serum Levels of PCSK9 Are Associated with Coronary Angiographic Severity in Patients with Acute Coronary Syndrome (
Diabetes Metab J 2018;42:207-14) -
Sung Woo Kim1, Keun-Gyu Park2

-
Diabetes & Metabolism Journal 2018;42(4):350-352.
DOI: https://doi.org/10.4093/dmj.2018.0138
Published online: August 21, 2018
1Department of Internal Medicine, Daegu Catholic University Medical Center, Catholic University of Daegu School of Medicine, Daegu, Korea.
2Department of Internal Medicine, School of Medicine, Kyungpook National University, Daegu, Korea.
- Corresponding author: Keun-Gyu Park. Department of Internal Medicine, School of Medicine, Kyungpook National University, 680 Gukchaebosang-ro, Jung-gu, Daegu 41944, Korea. kpark@knu.ac.kr
Copyright © 2018 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
-
CONFLICTS OF INTEREST: No potential conflict of interest relevant to this article was reported.
NOTES
- 1. Bae KH, Kim SW, Choi YK, Seo JB, Kim N, Kim CY, Lee WK, Lee S, Kim JG, Lee IK, Lee JH, Park KG. Serum levels of PCSK9 are associated with coronary angiographic severity in patients with acute coronary syndrome. Diabetes Metab J 2018;42:207-214. ArticlePubMedPMCPDF
- 2. Seidah NG, Awan Z, Chretien M, Mbikay M. PCSK9: a key modulator of cardiovascular health. Circ Res 2014;114:1022-1036. ArticlePubMed
- 3. Nanchen D, Gencer B, Auer R, Raber L, Stefanini GG, Klingenberg R, Schmied CM, Cornuz J, Muller O, Vogt P, Juni P, Matter CM, Windecker S, Luscher TF, Mach F, Rodondi N. Prevalence and management of familial hypercholesterolaemia in patients with acute coronary syndromes. Eur Heart J 2015;36:2438-2445. ArticlePubMed
- 4. Gencer B, Rodondi N, Auer R, Raber L, Klingenberg R, Nanchen D, Carballo D, Vogt P, Carballo S, Meyer P, Matter CM, Windecker S, Luscher TF, Mach F. Reasons for discontinuation of recommended therapies according to the patients after acute coronary syndromes. Eur J Intern Med 2015;26:56-62. ArticlePubMed
- 5. Mayne J, Dewpura T, Raymond A, Cousins M, Chaplin A, Lahey KA, Lahaye SA, Mbikay M, Ooi TC, Chretien M. Plasma PCSK9 levels are significantly modified by statins and fibrates in humans. Lipids Health Dis 2008;7:22ArticlePubMedPMC
- 6. Gencer B, Montecucco F, Nanchen D, Carbone F, Klingenberg R, Vuilleumier N, Aghlmandi S, Heg D, Raber L, Auer R, Juni P, Windecker S, Luscher TF, Matter CM, Rodondi N, Mach F. Prognostic value of PCSK9 levels in patients with acute coronary syndromes. Eur Heart J 2016;37:546-553. ArticlePubMed
- 7. Werner C, Hoffmann MM, Winkler K, Bohm M, Laufs U. Risk prediction with proprotein convertase subtilisin/kexin type 9 (PCSK9) in patients with stable coronary disease on statin treatment. Vascul Pharmacol 2014;62:94-102. ArticlePubMed
- 8. Glerup S, Schulz R, Laufs U, Schluter KD. Physiological and therapeutic regulation of PCSK9 activity in cardiovascular disease. Basic Res Cardiol 2017;112:32ArticlePubMedPMCPDF
- 9. Pirillo A, Norata GD, Catapano AL. LOX-1, OxLDL, and atherosclerosis. Mediators Inflamm 2013;2013:152786. ArticlePubMedPMCPDF
- 10. Giunzioni I, Tavori H, Covarrubias R, Major AS, Ding L, Zhang Y, DeVay RM, Hong L, Fan D, Predazzi IM, Rashid S, Linton MF, Fazio S. Local effects of human PCSK9 on the atherosclerotic lesion. J Pathol 2016;238:52-62. ArticlePubMedPDF
- 11. Zhao X, Zhang HW, Li S, Zhang Y, Xu RX, Zhu CG, Wu NQ, Guo YL, Qing P, Li XL, Liu G, Dong Q, Sun J, Li JJ. Association between plasma proprotein convertase subtisilin/kexin type 9 concentration and coronary artery calcification. Ann Clin Biochem 2018;55:158-164. ArticlePubMedPDF
- 12. Chandrakala AN, Sukul D, Selvarajan K, Sai-Sudhakar C, Sun B, Parthasarathy S. Induction of brain natriuretic peptide and monocyte chemotactic protein-1 gene expression by oxidized low-density lipoprotein: relevance to ischemic heart failure. Am J Physiol Cell Physiol 2012;302:C165-C177. ArticlePubMed
- 13. Bayes-Genis A, Nunez J, Zannad F, Ferreira JP, Anker SD, Cleland JG, Dickstein K, Filippatos G, Lang CC, Ng LL, Ponikowski P, Samani NJ, van Veldhuisen DJ, Zwinderman AH, Metra M, Lupon J, Voors AA. The PCSK9-LDL receptor axis and outcomes in heart failure: BIOSTAT-CHF subanalysis. J Am Coll Cardiol 2017;70:2128-2136. PubMed
- 14. Lakoski SG, Lagace TA, Cohen JC, Horton JD, Hobbs HH. Genetic and metabolic determinants of plasma PCSK9 levels. J Clin Endocrinol Metab 2009;94:2537-2543. ArticlePubMedPMC
- 15. Cui Q, Ju X, Yang T, Zhang M, Tang W, Chen Q, Hu Y, Haas JV, Troutt JS, Pickard RT, Darling R, Konrad RJ, Zhou H, Cao G. Serum PCSK9 is associated with multiple metabolic factors in a large Han Chinese population. Atherosclerosis 2010;213:632-636. ArticlePubMed
REFERENCES
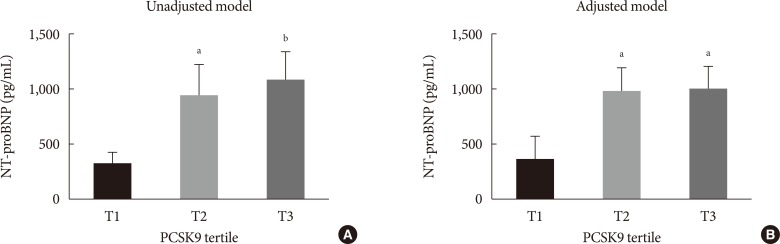
Fig. 1
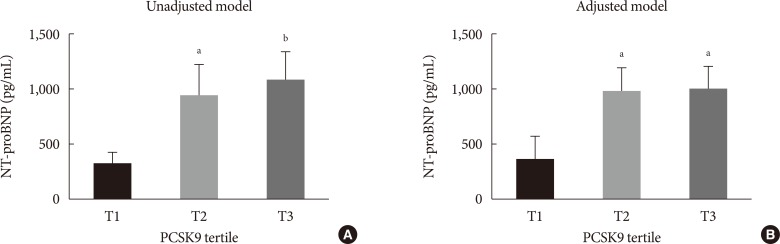
Levels of N-terminal pro-brain natriuretic peptide (NT-proBNP) according to serum proprotein convertase subtilisin/kexin type 9 (PCSK9) tertiles. Unadjusted model (A) and adjusted model (B). Model is adjusted for age, body mass index, past history of hypertension and diabetes mellitus, familial history of ischemic heart disease, and smoking. aP<0.05, bP<0.01.

Figure & Data
References
Citations
Citations to this article as recorded by 

- Plasma Levels of Proprotein Convertase Subtilisin/Kexin Type 9 Are Inversely Associated with N-Terminal Pro B-Type Natriuretic Peptide in Older Men and Women
Francesco Spannella, Federico Giulietti, Roberta Galeazzi, Anna Passarelli, Serena Re, Chiara Di Pentima, Massimiliano Allevi, Paolo Magni, Riccardo Sarzani
Biomedicines.2022; 10(8): 1961. CrossRef - PCSK9: Associated with cardiac diseases and their risk factors?
Yanan Guo, Binjie Yan, Shi Tai, Shenghua Zhou, Xi-Long Zheng
Archives of Biochemistry and Biophysics.2021; 704: 108717. CrossRef - Gut Lactobacillus Level Is a Predictive Marker for Coronary Atherosclerotic Lesions Progress and Prognosis in Patients With Acute Coronary Syndrome
Jing Gao, Jie Wang, Li-Li Zhao, Ting-Ting Yao, Yang Chen, Jing Ma, Xu Zhang, Jing-Xian Wang, Yuan Wang, Zhuang Cui, Yin Liu
Frontiers in Cellular and Infection Microbiology.2021;[Epub] CrossRef - Butein Synergizes with Statin to Upregulate Low-Density Lipoprotein Receptor ThroughHNF1α-Mediated PCSK9 Inhibition in HepG2 Cells
Jin-Taek Hwang, Hyo Jin Kim, Hyo-Kyoung Choi, Jae-Ho Park, Sangwon Chung, Min-Yu Chung
Journal of Medicinal Food.2020; 23(10): 1102. CrossRef
- Figure
- Related articles
-
- Advanced Liver Fibrosis Is Associated with Chronic Kidney Disease in Patients with Type 2 Diabetes Mellitus and Nonalcoholic Fatty Liver Disease (Diabetes Metab J 2022;46:630-9)
- Advanced Liver Fibrosis Is Associated with Chronic Kidney Disease in Patients with Type 2 Diabetes Mellitus and Nonalcoholic Fatty Liver Disease (Diabetes Metab J 2022;46:630-9)

 KDA
KDA PubReader
PubReader Cite
Cite