
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Search
- Page Path
- HOME > Search
- Basic Research
- N6-Methyladenosine Methyltransferase METTL3 Alleviates Diabetes-Induced Testicular Damage through Modulating TUG1/Clusterin Axis
- Yuan Tian, Yue-Hai Xiao, Chao Sun, Bei Liu, Fa Sun
- Diabetes Metab J. 2023;47(2):287-300. Published online January 19, 2023
- DOI: https://doi.org/10.4093/dmj.2021.0306
- 2,236 View
- 153 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
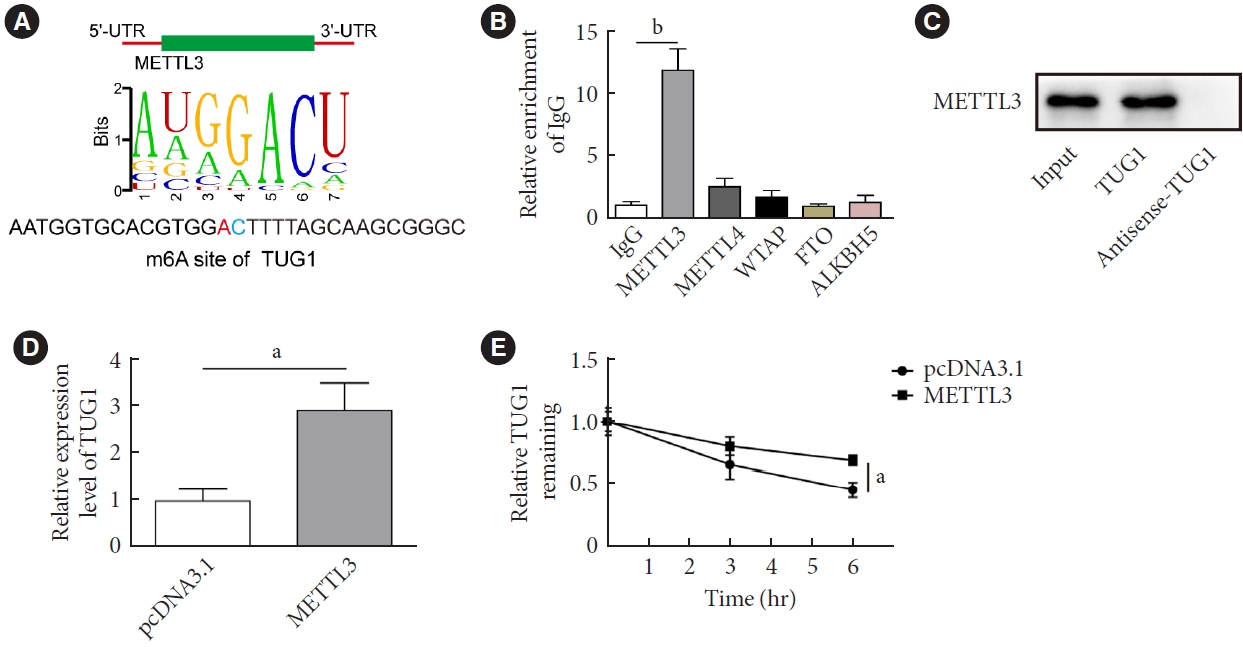
The present study investigated the regulatory effects of N6-methyladenosine (m6A) methyltransferase like-3 (METTL3) in diabetes-induced testicular damage.
Methods
In vivo diabetic mice and high glucose (HG) treated GC-1 spg cells were established. The mRNA and protein expressions were determined by real-time quantitative polymerase chain reaction, Western blot, immunofluorescence and immunohistochemistry staining. Levels of testosterone, blood glucose, cell viability, and apoptosis were detected by enzyme-linked immunosorbent assay, MTT, and flow cytometry, respectively. Molecular interactions were verified by RNA immunoprecipitation and RNA pull-down assay. Histopathological staining was performed to evaluate testicular injury.
Results
METTL3 and long non-coding RNA taurine up-regulated 1 (lncRNA TUG1) were downregulated in testicular tissues of diabetic mice and HG-treated GC-1 spg cells. METTL3 overexpression could reduce the blood glucose level, oxidative stress and testicular damage but enhance testosterone secretion in diabetic mouse model and HG-stimulated GC-1 spg cells. Mechanically, METTL3-mediated m6A methylation enhanced the stability of TUG1, then stabilizing the clusterin mRNA via recruiting serine and arginine rich splicing factor 1. Moreover, inhibition of TUG1/clusterin signaling markedly reversed the protective impacts of METTL3 overexpression on HG-stimulated GC-1 spg cells.
Conclusion
This study demonstrated that METTL3 ameliorated diabetes-induced testicular damage by upregulating the TUG1/clusterin signaling. These data further elucidate the potential regulatory mechanisms of m6A modification on diabetes-induced testicular injury. -
Citations
Citations to this article as recorded by- Negative Regulation of LINC01013 by METTL3 and YTHDF2 Enhances the Osteogenic Differentiation of Senescent Pre‐Osteoblast Cells Induced by Hydrogen Peroxide
Jiaxin Song, Yuejun Wang, Zhao Zhu, Wanqing Wang, Haoqing Yang, Zhaochen Shan
Advanced Biology.2024;[Epub] CrossRef - Diabetes and diabetic associative diseases: An overview of epigenetic regulations of TUG1
Mohammed Ageeli Hakami
Saudi Journal of Biological Sciences.2024; 31(5): 103976. CrossRef
- Negative Regulation of LINC01013 by METTL3 and YTHDF2 Enhances the Osteogenic Differentiation of Senescent Pre‐Osteoblast Cells Induced by Hydrogen Peroxide
- Complications
- Pathophysiologic Mechanisms and Potential Biomarkers in Diabetic Kidney Disease
- Chan-Young Jung, Tae-Hyun Yoo
- Diabetes Metab J. 2022;46(2):181-197. Published online March 24, 2022
- DOI: https://doi.org/10.4093/dmj.2021.0329
- 12,181 View
- 796 Download
- 41 Web of Science
- 46 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Although diabetic kidney disease (DKD) remains the leading cause of end-stage kidney disease eventually requiring chronic kidney replacement therapy, the prevalence of DKD has failed to decline over the past 30 years. In order to reduce disease prevalence, extensive research has been ongoing to improve prediction of DKD onset and progression. Although the most commonly used markers of DKD are albuminuria and estimated glomerular filtration rate, their limitations have encouraged researchers to search for novel biomarkers that could improve risk stratification. Considering that DKD is a complex disease process that involves several pathophysiologic mechanisms such as hyperglycemia induced inflammation, oxidative stress, tubular damage, eventually leading to kidney damage and fibrosis, many novel biomarkers that capture one specific mechanism of the disease have been developed. Moreover, the increasing use of high-throughput omic approaches to analyze biological samples that include proteomics, metabolomics, and transcriptomics has emerged as a strong tool in biomarker discovery. This review will first describe recent advances in the understanding of the pathophysiology of DKD, and second, describe the current clinical biomarkers for DKD, as well as the current status of multiple potential novel biomarkers with respect to protein biomarkers, proteomics, metabolomics, and transcriptomics.
-
Citations
Citations to this article as recorded by- Role of polyphenols in the management of diabetic complications
Jeevika Raina, Atika Firdous, Gurvinder Singh, Rajesh Kumar, Charanjit Kaur
Phytomedicine.2024; 122: 155155. CrossRef - Role of MCP-1 as an inflammatory biomarker in nephropathy
Yanlong Liu, Ke Xu, Yuhua Xiang, Boyan Ma, Hailong Li, Yuan Li, Yue Shi, Shuju Li, Yan Bai
Frontiers in Immunology.2024;[Epub] CrossRef - Urinary podocyte stress marker as a prognostic indicator for diabetic kidney disease
Lingfeng Zeng, Jack Kit-Chung Ng, Winston Wing-Shing Fung, Gordon Chun-Kau Chan, Kai-Ming Chow, Cheuk-Chun Szeto
BMC Nephrology.2024;[Epub] CrossRef - Identification and validation of immune and cuproptosis - related genes for diabetic nephropathy by WGCNA and machine learning
Yubing Chen, Lijuan Liao, Baoju Wang, Zhan Wu
Frontiers in Immunology.2024;[Epub] CrossRef - Specific Alternation of Gut Microbiota and the Role of Ruminococcus gnavus in the Development of Diabetic Nephropathy
Jinni Hong, Tingting Fu, Weizhen Liu, Yu Du, Junmin Bu, Guojian Wei, Miao Yu, Yanshan Lin, Cunyun Min, Datao Lin
Journal of Microbiology and Biotechnology.2024; 34(3): 547. CrossRef - The triglyceride-glucose index is superior to homeostasis model assessment of insulin resistance in predicting metabolic syndrome in an adult population in the United States
Beverley Adams-Huet, Rafael Zubirán, Alan T. Remaley, Ishwarlal Jialal
Journal of Clinical Lipidology.2024;[Epub] CrossRef - A Narrative Review of New Treatment Options for Diabetic Nephropathy
Aadhira Pillai, Darshna Fulmali
Cureus.2023;[Epub] CrossRef - Bamboo leaf: A review of traditional medicinal property, phytochemistry, pharmacology, and purification technology
Yaqian Cheng, Siqi Wan, Linna Yao, Ding Lin, Tong Wu, Yongjian Chen, Ailian Zhang, Chenfei Lu
Journal of Ethnopharmacology.2023; 306: 116166. CrossRef - Molecular Pathways of Diabetic Kidney Disease Inferred from Proteomics
Lan Wei, Yuanyuan Han, Chao Tu
Diabetes, Metabolic Syndrome and Obesity.2023; Volume 16: 117. CrossRef - Omics and Artificial Intelligence in Kidney Diseases
Nadja Grobe, Josef Scheiber, Hanjie Zhang, Christian Garbe, Xiaoling Wang
Advances in Kidney Disease and Health.2023; 30(1): 47. CrossRef - Intestinal microbiome diversity of diabetic and non-diabetic kidney disease: Current status and future perspective
Soumik Das, Ramanathan Gnanasambandan
Life Sciences.2023; 316: 121414. CrossRef - Pediatric Diabetic Nephropathy: Novel Insights from microRNAs
Francesca Lanzaro, Annalisa Barlabà, Angelica De Nigris, Federica Di Domenico, Valentina Verde, Emanuele Miraglia del Giudice, Anna Di Sessa
Journal of Clinical Medicine.2023; 12(4): 1447. CrossRef - Novel Biomarkers of Diabetic Kidney Disease
Jorge Rico-Fontalvo, Gustavo Aroca-Martínez, Rodrigo Daza-Arnedo, José Cabrales, Tomás Rodríguez-Yanez, María Cardona-Blanco, Juan Montejo-Hernández, Dairo Rodelo Barrios, Jhonny Patiño-Patiño, Elber Osorio Rodríguez
Biomolecules.2023; 13(4): 633. CrossRef - Diabetic vascular diseases: molecular mechanisms and therapeutic strategies
Yiwen Li, Yanfei Liu, Shiwei Liu, Mengqi Gao, Wenting Wang, Keji Chen, Luqi Huang, Yue Liu
Signal Transduction and Targeted Therapy.2023;[Epub] CrossRef - Metabolic phenotypes and risk of end-stage kidney disease in patients with type 2 diabetes
Lijun Zhao, Yutong Zou, Yucheng Wu, Linli Cai, Yuancheng Zhao, Yiting Wang, Xiang Xiao, Qing Yang, Jia Yang, Honghong Ren, Nanwei Tong, Fang Liu
Frontiers in Endocrinology.2023;[Epub] CrossRef - Identification of a New RNA and Protein Integrated Biomarker Panel Associated with Kidney Function Impairment in DKD: Translational Implications
Alessandra Scamporrino, Stefania Di Mauro, Agnese Filippello, Grazia Di Marco, Antonino Di Pino, Roberto Scicali, Maurizio Di Marco, Emanuele Martorana, Roberta Malaguarnera, Francesco Purrello, Salvatore Piro
International Journal of Molecular Sciences.2023; 24(11): 9412. CrossRef - Increased serum PCSK9 levels are associated with renal function impairment in patients with type 2 diabetes mellitus
Zhicai Feng, Xiangyu Liao, Hao Zhang, Juan Peng, Zhijun Huang, Bin Yi
Renal Failure.2023;[Epub] CrossRef - Analysis of Serum Pyrodeath Re-lated Proteins and Renal Injury in Patients with Type 2 DKD
茹洁 马
Asian Case Reports in Emergency Medicine.2023; 11(02): 53. CrossRef - Loganin reduces diabetic kidney injury by inhibiting the activation of NLRP3 inflammasome-mediated pyroptosis
Xiangri Kong, Yunyun Zhao, Xingye Wang, Yongjiang Yu, Ying Meng, Guanchi Yan, Miao Yu, Lihong Jiang, Wu Song, Bingmei Wang, Xiuge Wang
Chemico-Biological Interactions.2023; 382: 110640. CrossRef - Machine-learning algorithm-based prediction of a diagnostic model based on oxidative stress-related genes involved in immune infiltration in diabetic nephropathy patients
Heng-Mei Zhu, Na Liu, Dong-Xuan Sun, Liang Luo
Frontiers in Immunology.2023;[Epub] CrossRef - The roles of gut microbiota and its metabolites in diabetic nephropathy
Hui Zhao, Cheng-E Yang, Tian Liu, Ming-Xia Zhang, Yan Niu, Ming Wang, Jun Yu
Frontiers in Microbiology.2023;[Epub] CrossRef - High triglyceride levels increase the risk of diabetic microvascular complications: a cross-sectional study
Jiahang Li, Lei Shi, Guohong Zhao, Fei Sun, Zhenxing Nie, Zhongli Ge, Bin Gao, Yan Yang
Lipids in Health and Disease.2023;[Epub] CrossRef - Correlation of Kidney Injury Molecule-1 and Nephrin Levels in Iraqi Patients with Diabetic Nephropathy
Raghda Hisham Aljorani, Eman Saadi Saleh , Khalaf Gata Hussein Al Mohammadawi
Al-Rafidain Journal of Medical Sciences ( ISSN 2789-3219 ).2023; 5: 99. CrossRef - Diabetic Nephropathy: Significance of Determining Oxidative Stress and Opportunities for Antioxidant Therapies
Marina Darenskaya, Sergey Kolesnikov, Natalya Semenova, Lyubov Kolesnikova
International Journal of Molecular Sciences.2023; 24(15): 12378. CrossRef - Evaluation of Neutrophil/Lymphocyte Ratio, Low-Density Lipoprotein/Albumin Ratio, and Red Cell Distribution Width/Albumin Ratio in the Estimation of Proteinuria in Uncontrolled Diabetic Patients
Duygu Tutan, Murat Doğan
Cureus.2023;[Epub] CrossRef - Hedysarum polybotrys polysaccharide attenuates renal inflammatory infiltration and fibrosis in diabetic mice by inhibiting the HMGB1/RAGE/TLR4 pathway
Changqing Xu, Yanxu Cheng, Zongmei Liu, Xiaoyan Fu
Experimental and Therapeutic Medicine.2023;[Epub] CrossRef - Abdominal adipose tissue and type 2 diabetic kidney disease: adipose radiology assessment, impact, and mechanisms
Fei Lu, Jinlei Fan, Fangxuan Li, Lijing Liu, Zhiyu Chen, Ziyu Tian, Liping Zuo, Dexin Yu
Abdominal Radiology.2023; 49(2): 560. CrossRef - Inhibition of MD2 by natural product-drived JM-9 attenuates renal inflammation and diabetic nephropathy in mice
Minxiu Wang, Qianhui Zhang, Shuaijie Lou, Leiming Jin, Gaojun Wu, Wenqi Wu, Qidong Tang, Yi Wang, Xiaohong Long, Ping Huang, Wu Luo, Guang Liang
Biomedicine & Pharmacotherapy.2023; 168: 115660. CrossRef - Multifaceted relationship between diabetes and kidney diseases: Beyond diabetes
Pasquale Esposito, Daniela Picciotto, Francesca Cappadona, Francesca Costigliolo, Elisa Russo, Lucia Macciò, Francesca Viazzi
World Journal of Diabetes.2023; 14(10): 1450. CrossRef - Mitochondrial antiviral signaling protein: a potential therapeutic target in renal disease
Meng Wu, Zhiyin Pei, Guangfeng Long, Hongbing Chen, Zhanjun Jia, Weiwei Xia
Frontiers in Immunology.2023;[Epub] CrossRef - Research progress on multiple cell death pathways of podocytes in diabetic kidney disease
Can Yang, Zhen Zhang, Jieting Liu, Peijian Chen, Jialing Li, Haiying Shu, Yanhui Chu, Luxin Li
Molecular Medicine.2023;[Epub] CrossRef - Quantitative profiling of carboxylic compounds by gas chromatography-mass spectrometry for revealing biomarkers of diabetic kidney disease
Rongrong Zhu, Yan Yuan, Rourou Qi, Jianying Liang, Yan Shi, Hongbo Weng
Journal of Chromatography B.2023; 1231: 123930. CrossRef - Jiangtang Decoction Ameliorates Diabetic Kidney Disease Through the Modulation of the Gut Microbiota
Jinni Hong, Tingting Fu, Weizhen Liu, Yu Du, Junmin Bu, Guojian Wei, Miao Yu, Yanshan Lin, Cunyun Min, Datao Lin
Diabetes, Metabolic Syndrome and Obesity.2023; Volume 16: 3707. CrossRef - GLP-1RA Combined with SGLT2 Inhibitors for the Treatment of Diabetic Kidney Disease: A Meta Analysis
莹 郭
Advances in Clinical Medicine.2023; 13(11): 18117. CrossRef - Potential application of Klotho as a prognostic biomarker for patients with diabetic kidney disease: a meta-analysis of clinical studies
Li Xia Yu, Min Yue Sha, Yue Chen, Fang Tan, Xi Liu, Shasha Li, Qi-Feng Liu
Therapeutic Advances in Chronic Disease.2023;[Epub] CrossRef - Single-Cell RNA Sequencing Reveals RAC1 Involvement in Macrophages Efferocytosis in Diabetic Kidney Disease
Yi Song, Yifan Liu, Feng Guo, Lin Zhao, Guijun Qin
Inflammation.2023;[Epub] CrossRef - Research progress of natural active compounds on improving podocyte function to reduce proteinuria in diabetic kidney disease
Le Gong, Rui Wang, Xinyu Wang, Jing Liu, Zhaodi Han, Qian Li, Yi Jin, Hui Liao
Renal Failure.2023;[Epub] CrossRef - Identification of potential crosstalk genes and mechanisms between periodontitis and diabetic nephropathy through bioinformatic analysis
Huijuan Lu, Jia Sun, Jieqiong Sun
Medicine.2023; 102(52): e36802. CrossRef - Mitochondrial RNAs as Potential Biomarkers of Functional Impairment in Diabetic Kidney Disease
Stefania Di Mauro, Alessandra Scamporrino, Agnese Filippello, Maurizio Di Marco, Maria Teresa Di Martino, Francesca Scionti, Antonino Di Pino, Roberto Scicali, Roberta Malaguarnera, Francesco Purrello, Salvatore Piro
International Journal of Molecular Sciences.2022; 23(15): 8198. CrossRef - Renoprotective Mechanism of Sodium-Glucose Cotransporter 2 Inhibitors: Focusing on Renal Hemodynamics
Nam Hoon Kim, Nan Hee Kim
Diabetes & Metabolism Journal.2022; 46(4): 543. CrossRef - Partial Synthetic PPARƳ Derivative Ameliorates Aorta Injury in Experimental Diabetic Rats Mediated by Activation of miR-126-5p Pi3k/AKT/PDK 1/mTOR Expression
Yasmin M. Ahmed, Raha Orfali, Nada S. Abdelwahab, Hossam M. Hassan, Mostafa E. Rateb, Asmaa M. AboulMagd
Pharmaceuticals.2022; 15(10): 1175. CrossRef - Polydatin attenuates tubulointerstitial fibrosis in diabetic kidney disease by inhibiting YAP expression and nuclear translocation
Manlin He, Lan Feng, Yang Chen, Bin Gao, Yiwei Du, Lu Zhou, Fei Li, Hongbao Liu
Frontiers in Physiology.2022;[Epub] CrossRef - Prevalence of diabetic nephropathy in the diabetes mellitus population: A protocol for systematic review and meta-analysis
Sicheng Li, Huidi Xie, Yang Shi, Hongfang Liu
Medicine.2022; 101(42): e31232. CrossRef - Stratification of diabetic kidney diseases via data-independent acquisition proteomics–based analysis of human kidney tissue specimens
Qinghua Huang, Xianming Fei, Zhaoxian Zhong, Jieru Zhou, Jianguang Gong, Yuan Chen, Yiwen Li, Xiaohong Wu
Frontiers in Endocrinology.2022;[Epub] CrossRef - Novel biomarkers and therapeutic approaches for diabetic retinopathy and nephropathy: Recent progress and future perspectives
Ziyan Xie, Xinhua Xiao
Frontiers in Endocrinology.2022;[Epub] CrossRef - Diabetic Kidney Disease
Susanne B. Nicholas, Amy K. Mottl
Nephrology Self-Assessment Program.2022; 21(5): 394. CrossRef
- Role of polyphenols in the management of diabetic complications
- Basic Research
- Hypoxia Increases β-Cell Death by Activating Pancreatic Stellate Cells within the Islet
- Jong Jin Kim, Esder Lee, Gyeong Ryul Ryu, Seung-Hyun Ko, Yu-Bae Ahn, Ki-Ho Song
- Diabetes Metab J. 2020;44(6):919-927. Published online May 11, 2020
- DOI: https://doi.org/10.4093/dmj.2019.0181
- 5,973 View
- 146 Download
- 15 Web of Science
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub Background Hypoxia can occur in pancreatic islets in type 2 diabetes mellitus. Pancreatic stellate cells (PSCs) are activated during hypoxia. Here we aimed to investigate whether PSCs within the islet are also activated in hypoxia, causing β-cell injury.
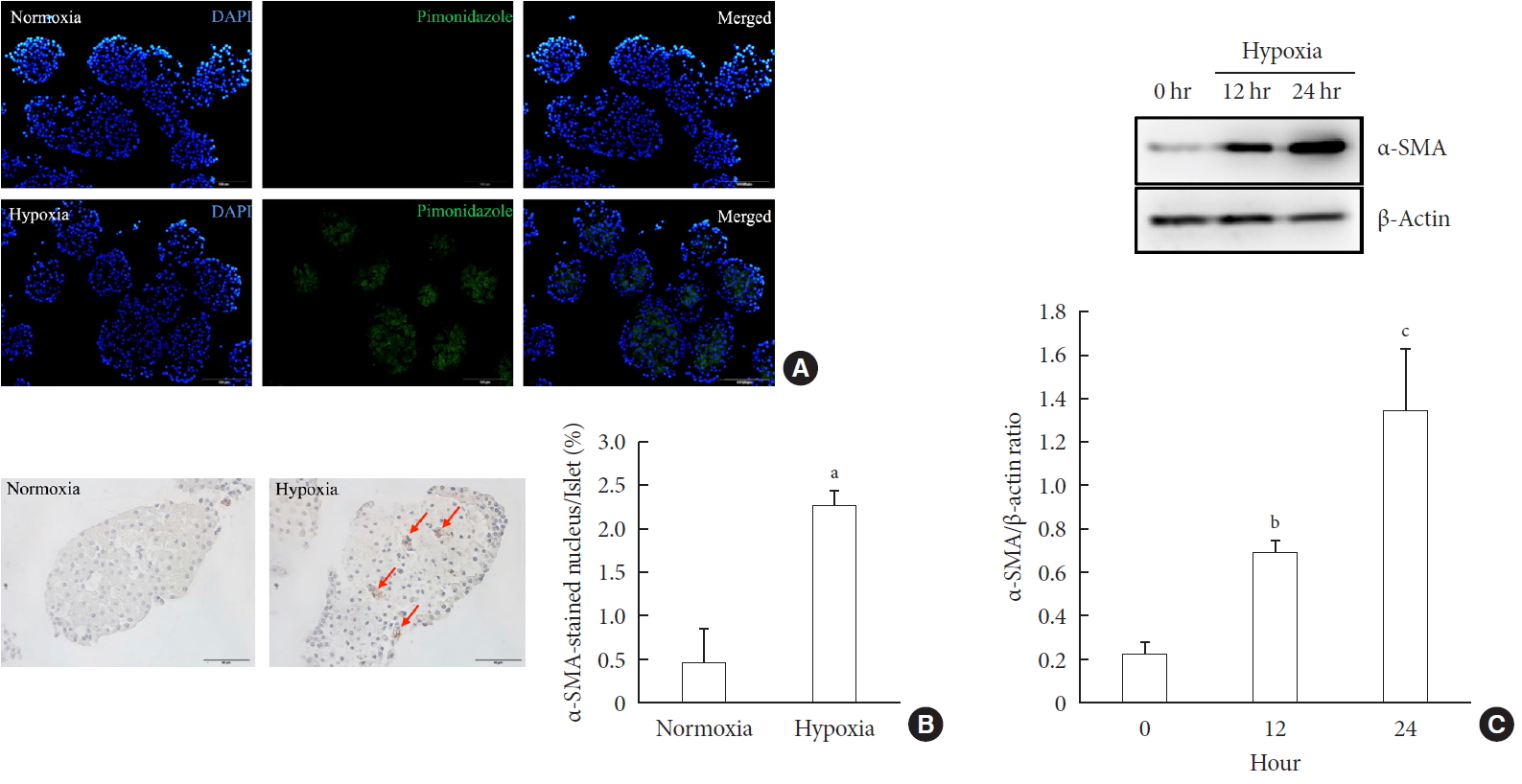
Methods Islet and primary PSCs were isolated from Sprague Dawley rats, and cultured in normoxia (21% O2) or hypoxia (1% O2). The expression of α-smooth muscle actin (α-SMA), as measured by immunostaining and Western blotting, was used as a marker of PSC activation. Conditioned media (hypoxia-CM) were obtained from PSCs cultured in hypoxia.
Results Islets and PSCs cultured in hypoxia exhibited higher expressions of α-SMA than did those cultured in normoxia. Hypoxia increased the production of reactive oxygen species. The addition of N-acetyl-L-cysteine, an antioxidant, attenuated the hypoxia-induced PSC activation in islets and PSCs. Islets cultured in hypoxia-CM showed a decrease in cell viability and an increase in apoptosis.
Conclusion PSCs within the islet are activated in hypoxia through oxidative stress and promote islet cell death, suggesting that hypoxia-induced PSC activation may contribute to β-cell loss in type 2 diabetes mellitus.
-
Citations
Citations to this article as recorded by- Effects of hypoxia in the diabetic corneal stroma microenvironment
Purnima Sharma, Jian-Xing Ma, Dimitrios Karamichos
Experimental Eye Research.2024; 240: 109790. CrossRef - Visualizing hypoxic modulation of beta cell secretions via a sensor augmented oxygen gradient
Kai Duan, Mengyang Zhou, Yong Wang, Jose Oberholzer, Joe F. Lo
Microsystems & Nanoengineering.2023;[Epub] CrossRef - Pancreatic stellate cells promote pancreatic β-cell death through exosomal microRNA transfer in hypoxia
Esder Lee, Gyeong Ryul Ryu, Seung-Hyun Ko, Yu-Bae Ahn, Ki-Ho Song
Molecular and Cellular Endocrinology.2023; 572: 111947. CrossRef - Pancreatic stellate cells in pancreatic cancer: as potential targets for future therapy
Zhengfeng Wang, Ru He, Shi Dong, Wence Zhou
Frontiers in Oncology.2023;[Epub] CrossRef - Recent advances in the development of bioartificial pancreas using 3D bioprinting for the treatment of type 1 diabetes: a review
Anushikha Ghosh, Arka Sanyal, Abhik Mallick
Exploration of Medicine.2023; : 886. CrossRef - Pancreas and islet morphology in cystic fibrosis: clues to the etiology of cystic fibrosis-related diabetes
Sarah S. Malik, Diksha Padmanabhan, Rebecca L. Hull-Meichle
Frontiers in Endocrinology.2023;[Epub] CrossRef - Diabetic mellitus, vascular calcification and hypoxia: A complex and neglected tripartite relationship
Xue-Jiao Sun, Nai-Feng Liu
Cellular Signalling.2022; 91: 110219. CrossRef - HIF-1 and NRF2; Key Molecules for Malignant Phenotypes of Pancreatic Cancer
Shin Hamada, Ryotaro Matsumoto, Atsushi Masamune
Cancers.2022; 14(2): 411. CrossRef - Pancreatic Stellate Cells and Metabolic Alteration: Physiology and Pathophysiology
Shin Hamada, Ryotaro Matsumoto, Atsushi Masamune
Frontiers in Physiology.2022;[Epub] CrossRef - Exosomal miR-140–3p and miR-143–3p from TGF-β1-treated pancreatic stellate cells target BCL2 mRNA to increase β-cell apoptosis
Xiangyun Zhu, Dechen Liu, Guoqing Li, Mengmeng Zhi, Ji Sun, Liang Qi, Jingbo Li, Stephen J. Pandol, Ling Li
Molecular and Cellular Endocrinology.2022; 551: 111653. CrossRef - Mitochondria oxidative stress mediated nicotine-promoted activation of pancreatic stellate cells by regulating mitochondrial dynamics
Yue Yuan, Zhiren Li, Miaomiao Li, Tong Jin, Xiaoyun Zhang, Xinjuan Liu, Jianyu Hao
Toxicology in Vitro.2022; 84: 105436. CrossRef - Antioxidant Mitoquinone Alleviates Chronic Pancreatitis via Anti-Fibrotic and Antioxidant Effects
Miaomiao Li, Yue Yuan, Xue Han, Xinjuan Liu, Weizhen Zhang, Jianyu Hao
Journal of Inflammation Research.2022; Volume 15: 4409. CrossRef - Diabetic Ferroptosis and Pancreatic Cancer: Foe or Friend?
Le Li, Xing-jia Yu, Lei Gao, Long Cheng, Bei Sun, Gang Wang
Antioxidants & Redox Signaling.2022; 37(16-18): 1206. CrossRef - Melatonin Induces Apoptosis and Modulates Cyclin Expression and MAPK Phosphorylation in Pancreatic Stellate Cells Subjected to Hypoxia
Matias Estaras, Manuel R. Gonzalez-Portillo, Miguel Fernandez-Bermejo, Jose M. Mateos, Daniel Vara, Gerardo Blanco-Fernandez, Diego Lopez-Guerra, Vicente Roncero, Gines M. Salido, Antonio González
International Journal of Molecular Sciences.2021; 22(11): 5555. CrossRef - Integrated pancreatic microcirculatory profiles of streptozotocin‐induced and insulin‐administrated type 1 diabetes mellitus
Yuan Li, Bingwei Li, Bing Wang, Mingming Liu, Xiaoyan Zhang, Ailing Li, Jian Zhang, Honggang Zhang, Ruijuan Xiu
Microcirculation.2021;[Epub] CrossRef - Pancreatic stellate cells - rising stars in pancreatic pathologies
P Hrabák, M Kalousová, T Krechler, T Zima
Physiological Research.2021; (S4): S597. CrossRef
- Effects of hypoxia in the diabetic corneal stroma microenvironment
- Basic Research
- The Role of CD36 in Type 2 Diabetes Mellitus: β-Cell Dysfunction and Beyond
- Jun Sung Moon, Udayakumar Karunakaran, Elumalai Suma, Seung Min Chung, Kyu Chang Won
- Diabetes Metab J. 2020;44(2):222-233. Published online April 23, 2020
- DOI: https://doi.org/10.4093/dmj.2020.0053
- 7,546 View
- 170 Download
- 17 Web of Science
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Impaired β-cell function is the key pathophysiology of type 2 diabetes mellitus, and chronic exposure of nutrient excess could lead to this tragedy. For preserving β-cell function, it is essential to understand the cause and mechanisms about the progression of β-cells failure. Glucotoxicity, lipotoxicity, and glucolipotoxicity have been suggested to be a major cause of β-cell dysfunction for decades, but not yet fully understood. Fatty acid translocase cluster determinant 36 (CD36), which is part of the free fatty acid (FFA) transporter system, has been identified in several tissues such as muscle, liver, and insulin-producing cells. Several studies have reported that induction of CD36 increases uptake of FFA in several cells, suggesting the functional interplay between glucose and FFA in terms of insulin secretion and oxidative metabolism. However, we do not currently know the regulating mechanism and physiological role of CD36 on glucolipotoxicity in pancreatic β-cells. Also, the downstream and upstream targets of CD36 related signaling have not been defined. In the present review, we will focus on the expression and function of CD36 related signaling in the pancreatic β-cells in response to hyperglycemia and hyperlipidemia (ceramide) along with the clinical studies on the association between CD36 and metabolic disorders.
-
Citations
Citations to this article as recorded by- Nrf2 inhibition regulates intracellular lipid accumulation in mouse insulinoma cells and improves insulin secretory function
Alpana Mukhuty, Samanwita Mandal, Chandrani Fouzder, Snehasis Das, Dipanjan Chattopadhyay, Tanmay Majumdar, Rakesh Kundu
Molecular and Cellular Endocrinology.2024; 581: 112112. CrossRef - CD36 gene variant rs1761667(G/A) as a biomarker in obese type 2 diabetes mellitus cases
Ashwin Kumar Shukla, Amreen Shamsad, Atar Singh Kushwah, Shalini Singh, Kauser Usman, Monisha Banerjee
Egyptian Journal of Medical Human Genetics.2024;[Epub] CrossRef - CD36 regulates macrophage and endothelial cell activation and multinucleate giant cell formation in anti neutrophil cytoplasm antibody vasculitis
Xiang Zhang, Catherine King, Alexander Dowell, Paul Moss, Lorraine Harper, Dimitrios Chanouzas, Xiong-zhong Ruan, Alan David Salama
Clinical Immunology.2024; 260: 109914. CrossRef - The association of soluble cluster of differentiation 36 with metabolic diseases: A potential biomarker and therapeutic target
Yun Li, Yaxi Chen, Xiong Z. Ruan
Pediatric Discovery.2023;[Epub] CrossRef - The role of candidate transport proteins in β‐cell long‐chain fatty acid uptake: Where are we now?
Christina Clavelo‐Farrow, Patricia Thomas
Diabetic Medicine.2023;[Epub] CrossRef - SARS-CoV-2 in the pancreas and the impaired islet function in COVID-19 patients
Ningfei Ji, Mingshun Zhang, Liang Ren, Yunyun Wang, Bicheng Hu, Jie Xiang, Yingyun Gong, Chaojie Wu, Guoqiang Qu, Wenqiu Ding, Zhiqiang Yin, Shan Li, Zhengxia Wang, Lianzheng Zhou, Xueqin Chen, Yuan Ma, Jinhai Tang, Yun Liu, Liang Liu, Mao Huang
Emerging Microbes & Infections.2022; 11(1): 1115. CrossRef - Is imaging-based muscle quantity associated with risk of diabetes? A meta-analysis of cohort studies
Shanhu Qiu, Xue Cai, Yang Yuan, Bo Xie, Zilin Sun, Tongzhi Wu
Diabetes Research and Clinical Practice.2022; 189: 109939. CrossRef - Lipotoxicity in a Vicious Cycle of Pancreatic Beta Cell Exhaustion
Vladimir Grubelnik, Jan Zmazek, Matej Završnik, Marko Marhl
Biomedicines.2022; 10(7): 1627. CrossRef - Association of cluster determinant 36, scavenger receptor class B type 1, and major facilitator superfamily domain containing the 2a genetic polymorphism with serum lipid profile in aging population with type 2 diabetes mellitus
Xixiang Wang, Xiaojun Ma, Jingjing Xu, Yujie Guo, Shaobo Zhou, Huiyan Yu, Linhong Yuan
Frontiers in Nutrition.2022;[Epub] CrossRef - CD36-Fatty Acid-Mediated Metastasis via the Bidirectional Interactions of Cancer Cells and Macrophages
Noorzaileen Eileena Zaidi, Nur Aima Hafiza Shazali, Thean-Chor Leow, Mohd Azuraidi Osman, Kamariah Ibrahim, Wan-Hee Cheng, Kok-Song Lai, Nik Mohd Afizan Nik Abd Rahman
Cells.2022; 11(22): 3556. CrossRef - The Past and Present Lives of the Intraocular Transmembrane Protein CD36
Rucui Yang, Qingping Liu, Mingzhi Zhang
Cells.2022; 12(1): 171. CrossRef - Implicating the effect of ketogenic diet as a preventive measure to obesity and diabetes mellitus
Sachin Kumar, Tapan Behl, Monika Sachdeva, Aayush Sehgal, Shilpa Kumari, Arun Kumar, Gagandeep Kaur, Harlokesh Narayan Yadav, Simona Bungau
Life Sciences.2021; 264: 118661. CrossRef - Contribution of rs3211938 polymorphism at CD36 to glucose levels, oxidized low-density lipoproteins, insulin resistance, and body mass index in Mexican mestizos with type-2 diabetes from western Mexico
Beatriz Teresita Martín-Márquez, Flavio Sandoval-Garcia, Mónica Vazquez-Del Mercado, Erika-Aurora Martínez-García, Fernanda-Isadora Corona-Meraz, Ana-Lilia Fletes-Rayas, Soraya-Amalí Zavaleta-Muñiz
Nutrición Hospitalaria.2021;[Epub] CrossRef - Investigating the association of CD36 gene polymorphisms (rs1761667 and rs1527483) with T2DM and dyslipidemia: Statistical analysis, machine learning based prediction, and meta-analysis
Ma’mon M. Hatmal, Walhan Alshaer, Ismail S. Mahmoud, Mohammad A. I. Al-Hatamleh, Hamzeh J. Al-Ameer, Omar Abuyaman, Malek Zihlif, Rohimah Mohamud, Mais Darras, Mohammad Al Shhab, Rand Abu-Raideh, Hilweh Ismail, Ali Al-Hamadi, Ali Abdelhay, Kanhaiya Singh
PLOS ONE.2021; 16(10): e0257857. CrossRef - Misregulation of Wnt Signaling Pathways at the Plasma Membrane in Brain and Metabolic Diseases
Mustafa Karabicici, Yagmur Azbazdar, Evin Iscan, Gunes Ozhan
Membranes.2021; 11(11): 844. CrossRef
- Nrf2 inhibition regulates intracellular lipid accumulation in mouse insulinoma cells and improves insulin secretory function
- Clinical Diabetes & Therapeutics
- Three Months Monitored Metabolic Fitness Modulates Cardiovascular Risk Factors in Diabetic Patients
- Ilenia Cirilli, Sonia Silvestri, Fabio Marcheggiani, Fabiola Olivieri, Roberta Galeazzi, Roberto Antonicelli, Rina Recchioni, Fiorella Marcheselli, Tiziana Bacchetti, Luca Tiano, Patrick Orlando
- Diabetes Metab J. 2019;43(6):893-897. Published online June 27, 2019
- DOI: https://doi.org/10.4093/dmj.2018.0254
- 3,931 View
- 46 Download
- 7 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Cardiovascular diseases represent the leading cause of death and moderate physical exercise is associated with a reduction in cardiovascular risk. The aim of the study was to evaluate the correlation between the amount of exercise recorded daily by a wearable gravitometer for 3 months and selected biochemical and clinical parameters. Nineteen sedentary type 2 diabetics were recruited and distributed into three homogenous groups, low, medium, and high exercise, according to the level of physical exercise monitored and expressed as MOVEs. Data showed an inverse correlation between MOVEs and oxidative stress indexes and a significant improvement in paraoxonase-1 activities and endothelial functionality. Decrease of visceral/total adipose tissue ratio, systolic blood pressure and a down-regulation of the inflammatory microRNA-146a in high exercise group were observed. Finally, a decrease of glycosylated hemoglobin and an up-regulation of the angiogenic microRNA-130a in medium exercise one was obtained. In this study, precise daily monitoring permitted to underline the importance of the amount of physical activity to counteract some cardiovascular risk factors persisting in diabetes. Finally, it identifies new microRNA biomarkers for future investigation on the same topic.
-
Citations
Citations to this article as recorded by- Emerging roles of microRNAs as diagnostics and potential therapeutic interest in type 2 diabetes mellitus
Dharmsheel Shrivastav, Desh Deepak Singh
World Journal of Clinical Cases.2024; 12(3): 525. CrossRef - Effects of Seven Weeks of Combined Physical Training on High-Density Lipoprotein Functionality in Overweight/Obese Subjects
Tiziana Bacchetti, Camilla Morresi, Gianna Ferretti, Anders Larsson, Torbjörn Åkerfeldt, Michael Svensson
Metabolites.2023; 13(10): 1068. CrossRef - Physical Exercise Protects Against Endothelial Dysfunction in Cardiovascular and Metabolic Diseases
Juan Gao, Xue Pan, Guoping Li, Emeli Chatterjee, Junjie Xiao
Journal of Cardiovascular Translational Research.2022; 15(3): 604. CrossRef - Effects of Exercise Training on the Paracrine Function of Circulating Angiogenic Cells
William S. Evans, Ryan M. Sapp, Katherine I. Kim, James M. Heilman, James Hagberg, Steven J. Prior
International Journal of Sports Medicine.2021; 42(12): 1047. CrossRef - Chronic and Transient Hyperglycemia Induces Changes in the Expression Patterns of IL6 and ADIPOQ Genes and Their Associated Epigenetic Modifications in Differentiating Human Visceral Adipocytes
Adam Wróblewski, Justyna Strycharz, Ewa Świderska, Aneta Balcerczyk, Janusz Szemraj, Józef Drzewoski, Agnieszka Śliwińska
International Journal of Molecular Sciences.2021; 22(13): 6964. CrossRef - The Potential Role of MicroRNA in Diabetic Cardiomyopathy
Jin Hwa Kim
Diabetes & Metabolism Journal.2020; 44(1): 54. CrossRef
- Emerging roles of microRNAs as diagnostics and potential therapeutic interest in type 2 diabetes mellitus
- Pathophysiology
- Metformin Ameliorates Lipotoxic β-Cell Dysfunction through a Concentration-Dependent Dual Mechanism of Action
- Hong Il Kim, Ji Seon Lee, Byung Kook Kwak, Won Min Hwang, Min Joo Kim, Young-Bum Kim, Sung Soo Chung, Kyong Soo Park
- Diabetes Metab J. 2019;43(6):854-866. Published online June 27, 2019
- DOI: https://doi.org/10.4093/dmj.2018.0179
- 6,673 View
- 115 Download
- 14 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Chronic exposure to elevated levels of free fatty acids contributes to pancreatic β-cell dysfunction. Although it is well known that metformin induces cellular energy depletion and a concomitant activation of AMP-activated protein kinase (AMPK) through inhibition of the respiratory chain, previous studies have shown inconsistent results with regard to the action of metformin on pancreatic β-cells. We therefore examined the effects of metformin on pancreatic β-cells under lipotoxic stress.
Methods NIT-1 cells and mouse islets were exposed to palmitate and treated with 0.05 and 0.5 mM metformin. Cell viability, glucose-stimulated insulin secretion, cellular adenosine triphosphate, reactive oxygen species (ROS) levels and Rho kinase (ROCK) activities were measured. The phosphorylation of AMPK was evaluated by Western blot analysis and mRNA levels of endoplasmic reticulum (ER) stress markers and NADPH oxidase (NOX) were measured by real-time quantitative polymerase chain reaction analysis.
Results We found that metformin has protective effects on palmitate-induced β-cell dysfunction. Metformin at a concentration of 0.05 mM inhibits NOX and suppresses the palmitate-induced elevation of ER stress markers and ROS levels in a AMPK-independent manner, whereas 0.5 mM metformin inhibits ROCK activity and activates AMPK.
Conclusion This study suggests that the action of metformin on β-cell lipotoxicity was implemented by different molecular pathways depending on its concentration. Metformin at a usual therapeutic dose is supposed to alleviate lipotoxic β-cell dysfunction through inhibition of oxidative stress and ER stress.
-
Citations
Citations to this article as recorded by- Metformin enhances METTL14-Mediated m6A methylation to alleviate NIT-1 cells apoptosis induced by hydrogen peroxide
Si-min Zhou, Xin-ming Yao, Yi Cheng, Yu-jie Xing, Yue Sun, Qiang Hua, Shu-jun Wan, Xiang-jian Meng
Heliyon.2024; 10(2): e24432. CrossRef - Reduced Expression Level of Protein PhosphatasePPM1EServes to Maintain Insulin Secretion in Type 2 Diabetes
Sevda Gheibi, Luis Rodrigo Cataldo, Alexander Hamilton, Mi Huang, Sebastian Kalamajski, Malin Fex, Hindrik Mulder
Diabetes.2023; 72(4): 455. CrossRef - Metformin restores prohormone processing enzymes and normalizes aberrations in secretion of proinsulin and insulin in palmitate‐exposed human islets
Quan Wen, Azazul Islam Chowdhury, Banu Aydin, Mudhir Shekha, Rasmus Stenlid, Anders Forslund, Peter Bergsten
Diabetes, Obesity and Metabolism.2023; 25(12): 3757. CrossRef - Treatment of type 2 diabetes mellitus with stem cells and antidiabetic drugs: a dualistic and future-focused approach
Priyamvada Amol Arte, Kanchanlata Tungare, Mustansir Bhori, Renitta Jobby, Jyotirmoi Aich
Human Cell.2023; 37(1): 54. CrossRef - Metformin disrupts insulin secretion, causes proapoptotic and oxidative effects in rat pancreatic beta‐cells in vitro
Maíra M.R. Valle, Eloisa Aparecida Vilas‐Boas, Camila F. Lucena, Simone A. Teixeira, Marcelo N. Muscara, Angelo R. Carpinelli
Journal of Biochemical and Molecular Toxicology.2022;[Epub] CrossRef - Protection by metformin against severe Covid-19: An in-depth mechanistic analysis
Nicolas Wiernsperger, Abdallah Al-Salameh, Bertrand Cariou, Jean-Daniel Lalau
Diabetes & Metabolism.2022; 48(4): 101359. CrossRef - Insight Into Rho Kinase Isoforms in Obesity and Energy Homeostasis
Lei Wei, Jianjian Shi
Frontiers in Endocrinology.2022;[Epub] CrossRef - Overexpression of miR-297b-5p Promotes Metformin-Mediated Protection Against Stearic Acid-Induced Senescence by Targeting Igf1r
Qingrui Zhao, Shenghan Su, Yuqing Lin, Xuebei Li, Lingfeng Dan, Yunjin Zhang, Chunxiao Yang, Xiaohan Li, Yimeng Dong, Chenchen Geng, Changhao Sun, Xia Chu, Huimin Lu
SSRN Electronic Journal .2022;[Epub] CrossRef - Metformin Dysregulates the Unfolded Protein Response and the WNT/β-Catenin Pathway in Endometrial Cancer Cells through an AMPK-Independent Mechanism
Domenico Conza, Paola Mirra, Gaetano Calì, Luigi Insabato, Francesca Fiory, Francesco Beguinot, Luca Ulianich
Cells.2021; 10(5): 1067. CrossRef - NADPH Oxidase (NOX) Targeting in Diabetes: A Special Emphasis on Pancreatic β-Cell Dysfunction
Suma Elumalai, Udayakumar Karunakaran, Jun-Sung Moon, Kyu-Chang Won
Cells.2021; 10(7): 1573. CrossRef - Metformin use and cardiovascular outcomes in patients with diabetes and chronic kidney disease: a nationwide cohort study
Min Ho Kim, Hyung Jung Oh, Soon Hyo Kwon, Jin Seok Jeon, Hyunjin Noh, Dong Cheol Han, Hyoungnae Kim, Dong-Ryeol Ryu
Kidney Research and Clinical Practice.2021; 40(4): 660. CrossRef - Different Effects of Metformin and A769662 on Sodium Iodate-Induced Cytotoxicity in Retinal Pigment Epithelial Cells: Distinct Actions on Mitochondrial Fission and Respiration
Chi-Ming Chan, Ponarulselvam Sekar, Duen-Yi Huang, Shu-Hao Hsu, Wan-Wan Lin
Antioxidants.2020; 9(11): 1057. CrossRef - Metformin Reduces Lipotoxicity-Induced Meta-Inflammation in β-Cells through the Activation of GPR40-PLC-IP3 Pathway
Ximei Shen, Beibei Fan, Xin Hu, Liufen Luo, Yuanli Yan, Liyong Yang
Journal of Diabetes Research.2019; 2019: 1. CrossRef
- Metformin enhances METTL14-Mediated m6A methylation to alleviate NIT-1 cells apoptosis induced by hydrogen peroxide
- Serum Ceruloplasmin Level as a Predictor for the Progression of Diabetic Nephropathy in Korean Men with Type 2 Diabetes Mellitus
- Min Jung Lee, Chang Hee Jung, Yu Mi Kang, Jung Eun Jang, Jaechan Leem, Joong-Yeol Park, Woo Je Lee
- Diabetes Metab J. 2015;39(3):230-239. Published online April 22, 2015
- DOI: https://doi.org/10.4093/dmj.2015.39.3.230
- 4,441 View
- 47 Download
- 22 Web of Science
- 22 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Oxidative stress is known to be associated with progression of diabetic kidney disease. Ceruloplasmin acts as a pro-oxidant under conditions of severe oxidative stress. Thus, we conducted a longitudinal observational study to evaluate whether the serum ceruloplasmin level is a predictive biomarker for progression of diabetic nephropathy.
Methods A total of 643 Korean men with type 2 diabetes mellitus were enrolled. Serum ceruloplasmin was measured using a nephelometric method. Progression of diabetic nephropathy was defined as transition in albuminuria class (i.e., normoalbuminuria to microalbuminuria, microalbuminuria to macroalbuminuria, or normoalbuminuria to macroalbuminuria) and/or a greater than 2-fold increase of serum creatinine at follow-up compared with the baseline value.
Results During the follow-up period (median, 2.7 years; range, 0.3 to 4.4 years), 49 of 643 patients (7.6%) showed the progression of diabetic nephropathy and three patients (0.5%) developed end-stage renal disease. Baseline ceruloplasmin levels were higher in the progressors than in the nonprogressors (262.6±40.9 mg/L vs. 233.3±37.8 mg/L,
P <0.001). Kaplan-Meier analysis showed a significantly higher incidence of nephropathy progression according to ceruloplasmin tertile (log-rank test,P <0.001). The hazard ratio (HR) for progression of diabetic nephropathy was significantly higher in the highest ceruloplasmin tertile category compared with the lowest ceruloplasmin tertile category, even after adjusting for confounding variables (HR, 3.32; 95% confidence interval, 1.28 to 8.61;P =0.003).Conclusion Baseline serum ceruloplasmin is an independent predictive factor for the progression of diabetic nephropathy in patients with type 2 diabetes mellitus.
-
Citations
Citations to this article as recorded by- In-depth urinary and exosome proteome profiling analysis identifies novel biomarkers for diabetic kidney disease
Shichun Du, Linhui Zhai, Shu Ye, Le Wang, Muyin Liu, Minjia Tan
Science China Life Sciences.2023; 66(11): 2587. CrossRef - Serum Level of Ceruloplasmin, Angiotensin-Converting Enzyme and Transferrin as Markers of Severity in SARS-CoV-2 Infection in Patients with Type 2 Diabetes
Patricia-Andrada Reștea, Ștefan Țigan, Laura Grațiela Vicaș, Luminița Fritea, Eleonora Marian, Tunde Jurca, Annamaria Pallag, Iulius Liviu Mureșan, Corina Moisa, Otilia Micle, Mariana Eugenia Mureșan
Microbiology Research.2023; 14(4): 1670. CrossRef - The nephropathy of sickle cell trait and sickle cell disease
Kenneth I. Ataga, Santosh L. Saraf, Vimal K. Derebail
Nature Reviews Nephrology.2022; 18(6): 361. CrossRef - Integrated Analysis of Single-Cell RNA-seq and Bulk RNA-seq in the Identification of a Novel ceRNA Network and Key Biomarkers in Diabetic Kidney Disease
Yuejun Wang, Mingming Zhao, Yu Zhang
International Journal of General Medicine.2022; Volume 15: 1985. CrossRef - Molecular Functions of Ceruloplasmin in Metabolic Disease Pathology
Zhidong Liu, Miao Wang, Chunbo Zhang, Shigao Zhou, Guang Ji
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2022; Volume 15: 695. CrossRef - A correlative study of copper, ceruloplasmin, iron, total iron binding capacity and total antioxidant capacity in diabetic nephropathy
Ramlingareddy, Shivashankara A Ramachandrayya, Jeena Jacob, Malathi Mala
Biomedicine.2022; 42(3): 469. CrossRef - Novel biomarkers for prognosticating diabetic kidney disease progression
Shilna Muttickal Swaminathan, Indu Ramachandra Rao, Srinivas Vinayak Shenoy, Attur Ravindra Prabhu, Pooja Basthi Mohan, Dharshan Rangaswamy, Mohan V Bhojaraja, Shivashankara Kaniyoor Nagri, Shankar Prasad Nagaraju
International Urology and Nephrology.2022; 55(4): 913. CrossRef - Evaluation of Serum Ceruloplasmin Levels as a Biomarker for Oxidative Stress in Patients With Diabetic Retinopathy
Gurunadh Satyanarayana, Narendra Keisham, Hitender S Batra, Subrahmanya Murti V, Mansur Khan, Sandeep Gupta, Vikram Mahindra
Cureus.2021;[Epub] CrossRef - Prospection of plasma proteins as biomarkers for diabetes mellitus monitoring
Liliane de Paula Silva, Fabiane Gomes de Moraes Rego, Geraldo Picheth, Marcelo Müller-Santos, Dayane Alberton
Journal of Diabetes & Metabolic Disorders.2021; 20(1): 611. CrossRef - Risk assessment for foot ulcers among Tunisian subjects with diabetes: a cross sectional outpatient study
B. Zantour, S. Bouchareb, Z. El Ati, F. Boubaker, W. Alaya, W. Kossomtini, M. H. Sfar
BMC Endocrine Disorders.2020;[Epub] CrossRef - Metalloproteins and apolipoprotein C: candidate plasma biomarkers of T2DM screened by comparative proteomics and lipidomics in ZDF rats
Shuai Wang, Zhiyuan Lu, Yuxin Wang, Tianran Zhang, Xiaodong He
Nutrition & Metabolism.2020;[Epub] CrossRef - Emerging vistas on electrochemical detection of diabetic retinopathy biomarkers
K.S. Shalini Devi, Madhurantakam Sasya, Uma Maheswari Krishnan
TrAC Trends in Analytical Chemistry.2020; 125: 115838. CrossRef - Oxidative stress in peritoneal dialysis patients: Association with the dialysis adequacy and technique survival
Natalia Stepanova, Lesya Korol, Olena Burdeyna
Indian Journal of Nephrology.2019; 29(5): 309. CrossRef - Recent advancements in biopolymer and metal nanoparticle-based materials in diabetic wound healing management
Veena Vijayakumar, Sushanta K. Samal, Smita Mohanty, Sanjay K. Nayak
International Journal of Biological Macromolecules.2019; 122: 137. CrossRef - Rat Böbrek Dokusunda Kurşunun Neden Olduğu Oksidatif Strese Karşı Kitosanın Koruyucu etkisi
Ugur ÖZDEK, Hasan TOZ, Ahmet Ufuk KÖMÜROĞLU, Leyla MİS, Zübeyir HUYUT, Yeter DEĞER
Van Veterinary Journal.2019; 30(3): 187. CrossRef - Changes in Trace Elements During Early Stages of Chronic Kidney Disease in Type 2 Diabetic Patients
Ching-Chiang Lin, Ching-Tang Shih, Chien-Hung Lee, Yeou-Lih Huang
Biological Trace Element Research.2018; 186(2): 330. CrossRef - The Divalent Elements Changes in Early Stages of Chronic Kidney Disease
Wan-Ju Kung, Ching-Tang Shih, Chien-Hung Lee, Ching-Chiang Lin
Biological Trace Element Research.2018; 185(1): 30. CrossRef - Long-term expression of glomerular genes in diabetic nephropathy
Dominik Chittka, Bernhard Banas, Laura Lennartz, Franz Josef Putz, Kathrin Eidenschink, Sebastian Beck, Thomas Stempfl, Christoph Moehle, Simone Reichelt-Wurm, Miriam C Banas
Nephrology Dialysis Transplantation.2018;[Epub] CrossRef - Incidence of chronic kidney disease among people with diabetes: a systematic review of observational studies
D. N. Koye, J. E. Shaw, C. M. Reid, R. C. Atkins, A. T. Reutens, D. J. Magliano
Diabetic Medicine.2017; 34(7): 887. CrossRef - Global epidemiology of diabetic foot ulceration: a systematic review and meta-analysis
Pengzi Zhang, Jing Lu, Yali Jing, Sunyinyan Tang, Dalong Zhu, Yan Bi
Annals of Medicine.2017; 49(2): 106. CrossRef - Biomarkers of diabetic nephropathy: A 2017 update
Nektaria Papadopoulou-Marketou, Christina Kanaka-Gantenbein, Nikolaos Marketos, George P. Chrousos, Ioannis Papassotiriou
Critical Reviews in Clinical Laboratory Sciences.2017; 54(5): 326. CrossRef - Serum Vascular Adhesion Protein-1 Predicts End-Stage Renal Disease in Patients with Type 2 Diabetes
Hung-Yuan Li, Hung-An Lin, Feng-Jung Nien, Vin-Cent Wu, Yi-Der Jiang, Tien-Jyun Chang, Hsien-Li Kao, Mao-Shin Lin, Jung-Nan Wei, Cheng-Hsin Lin, Shyang-Rong Shih, Chi-Sheng Hung, Lee-Ming Chuang, Emmanuel A Burdmann
PLOS ONE.2016; 11(2): e0147981. CrossRef
- In-depth urinary and exosome proteome profiling analysis identifies novel biomarkers for diabetic kidney disease
- Diabetic Cardiomyopathy and Its Prevention by Nrf2: Current Status
- Jing Chen, Zhiguo Zhang, Lu Cai
- Diabetes Metab J. 2014;38(5):337-345. Published online October 17, 2014
- DOI: https://doi.org/10.4093/dmj.2014.38.5.337
- 5,113 View
- 55 Download
- 76 Web of Science
- 75 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Diabetic cardiomyopathy (DCM), as one of the major cardiac complications in diabetic patients, is known to related with oxidative stress that is due to a severe imbalance between reactive oxygen species (ROS) and/or reactive nitrogen species (RNS) generation and their clearance by antioxidant defense systems. Transcription factor nuclear factor NF-E2-related factor 2 (Nrf2) plays an important role in maintaining the oxidative homeostasis by regulating multiple downstream antioxidants. Diabetes may up-regulate several antioxidants in the heart as a compensative mechanism at early stage, but at late stage, diabetes not only generates extra ROS and/or RNS but also impairs antioxidant capacity in the heart, including Nrf2. In an early study, we have established that Nrf2 protect the cardiac cells and heart from high level of glucose
in vitro and hyperglycemiain vivo , and in the following study demonstrated the significant down-regulation of cardiac Nrf2 expression in diabetic animals and patients. Using Nrf2-KO mice or Nrf2 inducers, blooming evidence has indicated the important protection by Nrf2 from cardiac pathogenesis in the diabetes. Therefore, this brief review summarizes the status of studies on Nrf2's role in preventing DCM and even other complications, the need for new and safe Nrf2 inducer screening and the precaution for the undesirable side of Nrf2 under certain conditions.-
Citations
Citations to this article as recorded by- Natural Products and Health
Joanna Bartkowiak-Wieczorek, Edyta Mądry
Nutrients.2024; 16(3): 415. CrossRef - Nrf2 prevents diabetic cardiomyopathy via antioxidant effect and normalization of glucose and lipid metabolism in the heart
Ge Yang, Qihe Zhang, Chao Dong, Guowen Hou, Jinjie Li, Xin Jiang, Ying Xin
Journal of Cellular Physiology.2024;[Epub] CrossRef - 3,4′,5-Trimethoxy-trans-stilbene ameliorates hepatic insulin resistance and oxidative stress in diabetic obese mice through insulin and Nrf2 signaling pathways
Yi Tan, Chunxiu Zhou, Lingchao Miao, Xutao Zhang, Haroon Khan, Baojun Xu, Wai San Cheang
Food & Function.2024; 15(6): 2996. CrossRef - Natural compounds protect against the pathogenesis of osteoarthritis by mediating the NRF2/ARE signaling
Zhenyu Wu, Zhouxin Yang, Luying Liu, Yong Xiao
Frontiers in Pharmacology.2023;[Epub] CrossRef - High fat diet exacerbates long-term metabolic, neuropathological, and behavioral derangements in an experimental mouse model of traumatic brain injury
Stanley Ibeh, Nour-Mounira Z. Bakkar, Fatima Ahmad, Judith Nwaiwu, Chloe Barsa, Sarine Mekhjian, Mohammad Amine Reslan, Ali H. Eid, Hayat Harati, Sanaa Nabha, Yehia Mechref, Ahmed F. El-Yazbi, Firas Kobeissy
Life Sciences.2023; 314: 121316. CrossRef - The Protective Effect of 11-Keto-β-Boswellic Acid against Diabetic Cardiomyopathy in Rats Entails Activation of AMPK
Jozaa Z. AlTamimi, Nora A. AlFaris, Ghedeir M. Alshammari, Reham I. Alagal, Dalal H. Aljabryn, Mohammed Abdo Yahya
Nutrients.2023; 15(7): 1660. CrossRef - Caffeic Acid Phenethyl Ester and Caffeamide Derivatives Suppress Oral Squamous Cell Carcinoma Cells
Yin-Hwa Shih, Chieh-Chieh Chen, Yueh-Hsiung Kuo, Lih-Jyh Fuh, Wan-Chen Lan, Tong-Hong Wang, Kuo-Chou Chiu, Thanh-Hien Vu Nguyen, Shih-Min Hsia, Tzong-Ming Shieh
International Journal of Molecular Sciences.2023; 24(12): 9819. CrossRef - The Role of Asiatic Acid in Preventing Dental Pulp Inflammation: An in-vivo Study
Arlina Nurhapsari, Risya Cilmiaty, Adi Prayitno, Bambang Purwanto, Soetrisno Soetrisno
Clinical, Cosmetic and Investigational Dentistry.2023; Volume 15: 109. CrossRef - Dexmedetomidine ameliorates diabetic cardiomyopathy by inhibiting ferroptosis through the Nrf2/GPX4 pathway
Fan Li, Zhenfei Hu, Yidan Huang, Haiting Zhan
Journal of Cardiothoracic Surgery.2023;[Epub] CrossRef - Metformin-mediated epigenetic modifications in diabetes and associated conditions: Biological and clinical relevance
Roberta Giordo, Anna Maria Posadino, Arduino Aleksander Mangoni, Gianfranco Pintus
Biochemical Pharmacology.2023; 215: 115732. CrossRef - Transient receptor potential vanilloid type 1: cardioprotective effects in diabetic models
Jiaqi Bao, Zhicheng Gao, Yilan Hu, Lifang Ye, Lihong Wang
Channels.2023;[Epub] CrossRef - Beyond Hepatoprotection—The Cardioprotective Effects of Bicyclol in Diabetes
Arun Samidurai, Rakesh C. Kukreja
Cardiovascular Drugs and Therapy.2023;[Epub] CrossRef - Sinapic acid ameliorates cardiac dysfunction and cardiomyopathy by modulating NF-κB and Nrf2/HO-1 signaling pathways in streptozocin induced diabetic rats
Mohammad Raish, Ajaz Ahmad, Yousef A. Bin Jardan, Mudassar Shahid, Khalid M. Alkharfy, Abdul Ahad, Mushtaq Ahmad Ansari, Ibrahim Abdelsalam Abdelrahman, Fahad I. Al-Jenoobi
Biomedicine & Pharmacotherapy.2022; 145: 112412. CrossRef - Recent Advances in KEAP1/NRF2-Targeting Strategies by Phytochemical Antioxidants, Nanoparticles, and Biocompatible Scaffolds for the Treatment of Diabetic Cardiovascular Complications
Andrea Rampin, Michele Carrabba, Martina Mutoli, Charlotte L. Eman, Gianluca Testa, Paolo Madeddu, Gaia Spinetti
Antioxidants & Redox Signaling.2022; 36(10-12): 707. CrossRef - Exercise and Urtica Dioica extract ameliorate mitochondrial function and the expression of cardiac muscle Nuclear Respiratory Factor 2 and Peroxisome proliferator-activated receptor Gamma Coactivator 1-alpha in STZ-induced diabetic rats
Seyyedeh Masoumeh Seyydi, Asghar Tofighi, Masoud Rahmati, Javad Tolouei Azar
Gene.2022; 822: 146351. CrossRef - 3,3′,4,5′-Tetramethoxy-trans-stilbene Improves Insulin Resistance by Activating the IRS/PI3K/Akt Pathway and Inhibiting Oxidative Stress
Yi Tan, Lingchao Miao, Jianbo Xiao, Wai San Cheang
Current Issues in Molecular Biology.2022; 44(5): 2175. CrossRef - The Beneficial Effects of Chinese Herbal Monomers on Ameliorating Diabetic Cardiomyopathy via Nrf2 Signaling
Yiwei Gao, Wu Liu, Xin Su, Xinyi Li, Fangning Yu, Ning Zhang, Yuli Huang
Oxidative Medicine and Cellular Longevity.2022; 2022: 1. CrossRef - Cardioprotective Effects and in-silico Antioxidant Mechanism of L-Ergothioneine in Experimental Type-2 Diabetic Rats
Ayobami Dare, Ahmed A Elrashedy, Mahendra L. Channa, Anand Nadar
Cardiovascular & Hematological Agents in Medicinal Chemistry.2022; 20(2): 133. CrossRef - Molecular Mechanisms of Ferroptosis and Relevance to Cardiovascular Disease
Lai-Hua Xie, Nadezhda Fefelova, Sri Harika Pamarthi, Judith K. Gwathmey
Cells.2022; 11(17): 2726. CrossRef - Cardiac adaptation and cardioprotection against arrhythmias and ischemia-reperfusion injury in mammalian hibernators
Lai-Hua Xie, Judith K. Gwathmey, Zhenghang Zhao
Pflügers Archiv - European Journal of Physiology.2021; 473(3): 407. CrossRef - Cardioprotective Effect of Glycyrrhizin on Myocardial Remodeling in Diabetic Rats
Vikram Thakur, Narah Alcoreza, Monica Delgado, Binata Joddar, Munmun Chattopadhyay
Biomolecules.2021; 11(4): 569. CrossRef - Therapeutic potential of targeting oxidative stress in diabetic cardiomyopathy
Nikole J. Byrne, Namakkal S. Rajasekaran, E Dale Abel, Heiko Bugger
Free Radical Biology and Medicine.2021; 169: 317. CrossRef - Punicalagin Protects Against Diabetic Cardiomyopathy by Promoting Opa1-Mediated Mitochondrial Fusion via Regulating PTP1B-Stat3 Pathway
Feng Fu, Chaoyang Liu, Rui Shi, Man Li, Min Zhang, Yanyan Du, Qiaojuan Wang, Jun Li, Guoen Wang, Jianming Pei, Mingge Ding
Antioxidants & Redox Signaling.2021; 35(8): 618. CrossRef - Elevated type I interferon responses potentiate metabolic dysfunction, inflammation, and accelerated aging in mtDNA mutator mice
Yuanjiu Lei, Camila Guerra Martinez, Sylvia Torres-Odio, Samantha L. Bell, Christine E. Birdwell, Joshua D. Bryant, Carl W. Tong, Robert O. Watson, Laura Ciaccia West, A. Phillip West
Science Advances.2021;[Epub] CrossRef - The potential role of Keap1-Nrf2 pathway in the pathogenesis of Alzheimer’s disease, type 2 diabetes, and type 2 diabetes-related Alzheimer’s disease
Ling He, Yi Sun
Metabolic Brain Disease.2021; 36(7): 1469. CrossRef - The impact of mitochondria on cancer treatment resistance
Michelle van der Merwe, Gustav van Niekerk, Carla Fourie, Manisha du Plessis, Anna-Mart Engelbrecht
Cellular Oncology.2021; 44(5): 983. CrossRef - Therapeutic Approaches Targeting Proteostasis in Kidney Disease and Fibrosis
Jia-Huang Chen, Chia-Hsien Wu, Chih-Kang Chiang
International Journal of Molecular Sciences.2021; 22(16): 8674. CrossRef - Coronary Large Conductance Ca2+-Activated K+ Channel Dysfunction in Diabetes Mellitus
Tong Lu, Hon-Chi Lee
Frontiers in Physiology.2021;[Epub] CrossRef - Ferroptosis: New Dawn for Overcoming the Cardio-Cerebrovascular Diseases
Meng-Yi Luo, Jian-Hui Su, Shao-Xin Gong, Na Liang, Wen-Qian Huang, Wei Chen, Ai-Ping Wang, Ying Tian
Frontiers in Cell and Developmental Biology.2021;[Epub] CrossRef - Recombinant Human Growth Hormone Inhibits Lipotoxicity, Oxidative Stress, and Apoptosis in a Mouse Model of Diabetic Cardiomyopathy
Zuowei Pei, Xiang Wang, Chenguang Yang, Min Dong, Fang Wang, Juan Gambini
Oxidative Medicine and Cellular Longevity.2021; 2021: 1. CrossRef - Hydrogen sulfide mitigates myocardial inflammation by inhibiting nucleotide-binding oligomerization domain-like receptor protein 3 inflammasome activation in diabetic rats
Qiang Jia, Shomaila Mehmood, Xiaofen Liu, Shanfeng Ma, Rui Yang
Experimental Biology and Medicine.2020; 245(3): 221. CrossRef - Heme oxygenase-1 in protozoan infections: A tale of resistance and disease tolerance
Rafael C. M. C. Silva, Leonardo H. Travassos, Claudia N. Paiva, Marcelo T. Bozza, Marc-Jan Gubbels
PLOS Pathogens.2020; 16(7): e1008599. CrossRef - Distinct Approaches of Raloxifene: Its Far-Reaching Beneficial Effects Implicating the HO-System
Denise Börzsei, Renáta Szabó, Alexandra Hoffmann, Médea Veszelka, Imre Pávó, Zsolt Turcsán, Csaba Viczián, Krisztina Kupai, Csaba Varga, Anikó Pósa
Biomolecules.2020; 10(3): 375. CrossRef - The Mitochondria: A Target of Polyphenols in the Treatment of Diabetic Cardiomyopathy
Humna Bhagani, Suzanne A. Nasser, Ali Dakroub, Ahmed F. El-Yazbi, Assaad A. Eid, Firas Kobeissy, Gianfranco Pintus, Ali H. Eid
International Journal of Molecular Sciences.2020; 21(14): 4962. CrossRef - The Effects of Dietary Supplements that Overactivate the Nrf2/ARE System
Robert E. Smith
Current Medicinal Chemistry.2020; 27(13): 2077. CrossRef - Allopurinol reduces oxidative stress and activates Nrf2/p62 to attenuate diabetic cardiomyopathy in rats
Jierong Luo, Dan Yan, Sisi Li, Shiming Liu, Fei Zeng, Chi Wai Cheung, Hong Liu, Michael G. Irwin, Huansen Huang, Zhengyuan Xia
Journal of Cellular and Molecular Medicine.2020; 24(2): 1760. CrossRef - Rg1 protects H9C2 cells from high glucose‐/palmitate‐induced injury via activation of AKT/GSK‐3β/Nrf2 pathway
Haitao Yu, Juan Zhen, Yang Yang, Jian Du, Jiyan Leng, Qian Tong
Journal of Cellular and Molecular Medicine.2020; 24(14): 8194. CrossRef - Ranolazine protects against diabetic cardiomyopathy by activating the NOTCH1/NRG1 pathway
Xi Chen, Long Ren, Xing Liu, Xi Sun, Chaorun Dong, Yanan Jiang, Ying Qin, Huan Qu, Jinfeng Jiao, Shuo Wang, Yunlong Bai, Baofeng Yang
Life Sciences.2020; 261: 118306. CrossRef - Low Concentration of Withaferin a Inhibits Oxidative Stress-Mediated Migration and Invasion in Oral Cancer Cells
Tzu-Jung Yu, Jen-Yang Tang, Fu Ou-Yang, Yen-Yun Wang, Shyng-Shiou F. Yuan, Kevin Tseng, Li-Ching Lin, Hsueh-Wei Chang
Biomolecules.2020; 10(5): 777. CrossRef - Protective Effect of Simplicillium sp. Ethyl Acetate Extract against High Glucose-Induced Oxidative Stress in HUVECs
Ting-Ting Tian, Qi-Rui Li, Shi-Quan Gan, Chu-Rui Chang, Xiang-Chun Shen
Evidence-Based Complementary and Alternative Medicine.2020; 2020: 1. CrossRef - Deneysel Diyabet Oluşturulan Sıçanlarda Kalp ve İskelet Kası Nrf2 Yapımı ve Oksidatif Stres Üzerine Melatoninin Etkisinin İncelenmesi
Salim ÖZENOĞLU, İnci TURAN, Hale SAYAN ÖZAÇMAK, Veysel Haktan ÖZAÇMAK
Turkish Journal of Diabetes and Obesity.2020; 4(1): 46. CrossRef - Nicorandil alleviates apoptosis in diabetic cardiomyopathy through PI3K/Akt pathway
Xuyang Wang, Jinyu Pan, Dian Liu, Mingjun Zhang, Xiaowei Li, Jingjing Tian, Ming Liu, Tao Jin, Fengshuang An
Journal of Cellular and Molecular Medicine.2019; 23(8): 5349. CrossRef - Bailcalin Protects against Diabetic Cardiomyopathy through Keap1/Nrf2/AMPK-Mediated Antioxidative and Lipid-Lowering Effects
Ran Li, Yuan Liu, Ying-guang Shan, Lu Gao, Fang Wang, Chun-guang Qiu
Oxidative Medicine and Cellular Longevity.2019; 2019: 1. CrossRef - Omega 3 rich diet modulates energy metabolism via GPR120-Nrf2 crosstalk in a novel antioxidant mouse model
Deborah Amos, Carla Cook, Nalini Santanam
Biochimica et Biophysica Acta (BBA) - Molecular and Cell Biology of Lipids.2019; 1864(4): 466. CrossRef - Increased placental expressions of nuclear factor erythroid 2–related factor 2 and antioxidant enzymes in gestational diabetes: Protective mechanisms against the placental oxidative stress?
Balachandiran Manoharan, Zachariah Bobby, Gowri Dorairajan, Sajini Elizabeth Jacob, Victorraj Gladwin, Vickneshwaran Vinayagam, Rajaa Muthu Packirisamy
European Journal of Obstetrics & Gynecology and Reproductive Biology.2019; 238: 78. CrossRef - Another look at phenolic compounds in cancer therapy the effect of polyphenols on ubiquitin-proteasome system
Aleksandra Golonko, Tomasz Pienkowski, Renata Swislocka, Ryszard Lazny, Marek Roszko, Wlodzimierz Lewandowski
European Journal of Medicinal Chemistry.2019; 167: 291. CrossRef - Hydrogen sulfide-mediated regulation of cell death signaling ameliorates adverse cardiac remodeling and diabetic cardiomyopathy
Sumit Kar, Tyler N. Kambis, Paras K. Mishra
American Journal of Physiology-Heart and Circulatory Physiology.2019; 316(6): H1237. CrossRef - Genomic and Genetic Approaches to Deciphering Acute Respiratory Distress Syndrome Risk and Mortality
Heather Lynn, Xiaoguang Sun, Nancy Casanova, Manuel Gonzales-Garay, Christian Bime, Joe G.N. Garcia
Antioxidants & Redox Signaling.2019; 31(14): 1027. CrossRef - Enhanced Keap1-Nrf2 signaling protects the myocardium from isoproterenol-induced pathological remodeling in mice
Gobinath Shanmugam, Anil Kumar Challa, Silvio H. Litovsky, Asokan Devarajan, Ding Wang, Dean P. Jones, Victor M. Darley-Usmar, Namakkal Soorappan Rajasekaran
Redox Biology.2019; 27: 101212. CrossRef - Effects of PP2A/Nrf2 on experimental diabetes mellitus-related cardiomyopathy by regulation of autophagy and apoptosis through ROS dependent pathway
Yanhui Guan, Lichun Zhou, Yu Zhang, Huiqin Tian, Anqi Li, Xiuzhen Han
Cellular Signalling.2019; 62: 109339. CrossRef - An Aza resveratrol–chalcone derivative 6b protects mice against diabetic cardiomyopathy by alleviating inflammation and oxidative stress
Shengban You, Jianchang Qian, Chuchu Sun, Hailing Zhang, Shiju Ye, Taiwei Chen, Zheng Xu, Jingying Wang, Weijian Huang, Guang Liang
Journal of Cellular and Molecular Medicine.2018; 22(3): 1931. CrossRef - Oxidative Stress in Mesenchymal Stem Cell Senescence: Regulation by Coding and Noncoding RNAs
Rosa Vono, Eva Jover Garcia, Gaia Spinetti, Paolo Madeddu
Antioxidants & Redox Signaling.2018; 29(9): 864. CrossRef - An overview of the emerging interface between cardiac metabolism, redox biology and the circadian clock
Rodrigo A. Peliciari-Garcia, Victor Darley-Usmar, Martin E. Young
Free Radical Biology and Medicine.2018; 119: 75. CrossRef - Klotho protects the heart from hyperglycemia-induced injury by inactivating ROS and NF-κB-mediated inflammation both in vitro and in vivo
Yue Guo, Xiaodong Zhuang, Zena Huang, Jing Zou, Daya Yang, Xun Hu, Zhimin Du, Lichun Wang, Xinxue Liao
Biochimica et Biophysica Acta (BBA) - Molecular Basis of Disease.2018; 1864(1): 238. CrossRef - Paradoxical cardiotoxicity of intraperitoneally-injected epigallocatechin gallate preparation in diabetic mice
Nora O. Abdel Rasheed, Lamiaa A. Ahmed, Dalaal M. Abdallah, Bahia M. El-Sayeh
Scientific Reports.2018;[Epub] CrossRef - Oxidative stress-induced miR-27a targets the redox gene nuclear factor erythroid 2-related factor 2 in diabetic embryopathy
Yang Zhao, Daoyin Dong, E. Albert Reece, Ashley R. Wang, Peixin Yang
American Journal of Obstetrics and Gynecology.2018; 218(1): 136.e1. CrossRef - Regulation on SIRT1-PGC-1α/Nrf2 pathway together with selective inhibition of aldose reductase makes compound hr5F a potential agent for the treatment of diabetic complications
Zhihua Wang, Sheng Yuan, Yanbing Li, Zhe Zhang, Wei Xiao, Dan Tang, Kaihe Ye, Zhijun Liu, Congcong Wang, Yixiong Zheng, Hong Nie, Heru Chen
Biochemical Pharmacology.2018; 150: 54. CrossRef - Fibroblast growth factor-21 prevents diabetic cardiomyopathy via AMPK-mediated antioxidation and lipid-lowering effects in the heart
Hong Yang, Anyun Feng, Sundong Lin, Lechu Yu, Xiufei Lin, Xiaoqing Yan, Xuemian Lu, Chi Zhang
Cell Death & Disease.2018;[Epub] CrossRef - Salusin-β contributes to oxidative stress and inflammation in diabetic cardiomyopathy
Ming-Xia Zhao, Bing Zhou, Li Ling, Xiao-Qing Xiong, Feng Zhang, Qi Chen, Yue-Hua Li, Yu-Ming Kang, Guo-Qing Zhu
Cell Death & Disease.2017; 8(3): e2690. CrossRef - Role of Nrf2 Signaling in the Regulation of Vascular BK Channel β1 Subunit Expression and BK Channel Function in High-Fat Diet–Induced Diabetic Mice
Tong Lu, Xiaojing Sun, Yong Li, Qiang Chai, Xiao-Li Wang, Hon-Chi Lee
Diabetes.2017; 66(10): 2681. CrossRef - Regulation of vascular large-conductance calcium-activated potassium channels by Nrf2 signalling
Yong Li, Xiao-Li Wang, Xiaojing Sun, Qiang Chai, Jingchao Li, Benjamin Thompson, Win-Kuang Shen, Tong Lu, Hon-Chi Lee
Diabetes and Vascular Disease Research.2017; 14(4): 353. CrossRef - Metallothionein Is Downstream of Nrf2 and Partially Mediates Sulforaphane Prevention of Diabetic Cardiomyopathy
Junlian Gu, Yanli Cheng, Hao Wu, Lili Kong, Shudong Wang, Zheng Xu, Zhiguo Zhang, Yi Tan, Bradley B. Keller, Honglan Zhou, Yuehui Wang, Zhonggao Xu, Lu Cai
Diabetes.2017; 66(2): 529. CrossRef - Kimchi methanol extracts attenuate hepatic steatosis induced by high cholesterol diet in low-density lipoprotein receptor knockout mice through inhibition of endoplasmic reticulum stress
Minji Woo, Mijeong Kim, Jeong Sook Noh, Yeong Ok Song
Journal of Functional Foods.2017; 32: 218. CrossRef - Aspalathin Protects the Heart against Hyperglycemia-Induced Oxidative Damage by Up-Regulating Nrf2 Expression
Phiwayinkosi Dludla, Christo Muller, Elizabeth Joubert, Johan Louw, M. Essop, Kwazi Gabuza, Samira Ghoor, Barbara Huisamen, Rabia Johnson
Molecules.2017; 22(1): 129. CrossRef - Intermittent hypoxia-induced cardiomyopathy and its prevention by Nrf2 and metallothionein
Shanshan Zhou, Xia Yin, Jingpeng Jin, Yi Tan, Daniel J. Conklin, Ying Xin, Zhiguo Zhang, Weixia Sun, Taixing Cui, Jun Cai, Yang Zheng, Lu Cai
Free Radical Biology and Medicine.2017; 112: 224. CrossRef - Inhibitory effects of rosmarinic acid on pterygium epithelial cells through redox imbalance and induction of extrinsic and intrinsic apoptosis
Ya-Yu Chen, Chia-Fang Tsai, Ming-Chu Tsai, Yu-Wen Hsu, Fung-Jou Lu
Experimental Eye Research.2017; 160: 96. CrossRef - Ischemia reperfusion injury, ischemic conditioning and diabetes mellitus
Anne Lejay, Fei Fang, Rohan John, Julie A.D. Van, Meredith Barr, Fabien Thaveau, Nabil Chakfe, Bernard Geny, James W. Scholey
Journal of Molecular and Cellular Cardiology.2016; 91: 11. CrossRef - The Role of the Nrf2/ARE Antioxidant System in Preventing Cardiovascular Diseases
Robert Smith, Kevin Tran, Cynthia Smith, Miranda McDonald, Pushkar Shejwalkar, Kenji Hara
Diseases.2016; 4(4): 34. CrossRef - Prohibitin overexpression improves myocardial function in diabetic cardiomyopathy
Wen-qian Dong, Min Chao, Qing-hua Lu, Wei-li Chai, Wei Zhang, Xue-ying Chen, Er-shun Liang, Ling-bo Wang, Hong-liang Tian, Yu-guo Chen, Ming-xiang Zhang
Oncotarget.2016; 7(1): 66. CrossRef - Restoration of Nrf2 Signaling Normalizes the Regenerative Niche
Marc A. Soares, Oriana D. Cohen, Yee Cheng Low, Rita A. Sartor, Trevor Ellison, Utkarsh Anil, Lavinia Anzai, Jessica B. Chang, Pierre B. Saadeh, Piul S. Rabbani, Daniel J. Ceradini
Diabetes.2016; 65(3): 633. CrossRef - Myocardial transcription factors in diastolic dysfunction: clues for model systems and disease
Alexander T. Mikhailov, Mario Torrado
Heart Failure Reviews.2016; 21(6): 783. CrossRef - Antioxidant Properties of Whole Body Periodic Acceleration (pGz)
Arkady Uryash, Jorge Bassuk, Paul Kurlansky, Francisco Altamirano, Jose R. Lopez, Jose A. Adams, Guillermo López Lluch
PLOS ONE.2015; 10(7): e0131392. CrossRef - Mulberry leaves (Morus alba L.) ameliorate obesity-induced hepatic lipogenesis, fibrosis, and oxidative stress in high-fat diet-fed mice
Ji-Young Ann, Hyeyoon Eo, Yunsook Lim
Genes & Nutrition.2015;[Epub] CrossRef - Oxidative Stress and Human Hypertension: Vascular Mechanisms, Biomarkers, and Novel Therapies
Augusto C. Montezano, Maria Dulak-Lis, Sofia Tsiropoulou, Adam Harvey, Ana M. Briones, Rhian M. Touyz
Canadian Journal of Cardiology.2015; 31(5): 631. CrossRef - Haeme oxygenase signalling pathway: implications for cardiovascular disease
Laura E. Fredenburgh, Allison A. Merz, Susan Cheng
European Heart Journal.2015; 36(24): 1512. CrossRef
- Natural Products and Health
- The Role of Oxidative Stress in the Pathogenesis of Diabetic Vascular Complications
- Shuji Sasaki, Toyoshi Inoguchi
- Diabetes Metab J. 2012;36(4):255-261. Published online August 20, 2012
- DOI: https://doi.org/10.4093/dmj.2012.36.4.255
- 3,811 View
- 62 Download
- 60 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Oxidative stress has been paid increasing attention to as an important causative factor for diabetic vascular complications. Among possible various sources, accumulating evidence has indicated that NAD(P)H oxidase may be the most important source for reactive oxygen species production in diabetic vascular tissues. The mechanisms underlying activation and up-regulation of NAD(P)H oxidase has been supposed to be mediated by high glucose-induced protein kinase C (PKC) activation. In this review article, activation of local renin-angiotensin II system induced by chymase activation is also shown to amplify such a PKC-dependent activation of NAD(P)H oxidase. Additionally, human evidence showing the beneficial effect of antioxidants on diabetic vascular complications. Bilirubin has been recognized as a strong endogenous antioxidant. Here markedly lower prevalence of vascular complications is shown in diabetic patients with Gilbert syndrome, a congenital hyperbilirubinemia, as well as reduced markers of oxidative stress and inflammation. Lastly, statin, angiotensin II receptor blocker, chymase inhibitor, bilirubin and biliverdin, PKC β isoform inhibitor, and glucagon-like peptide-1 analog, are shown to serve as antioxidants and have some beneficial effect on diabetic vascular complications, via inhibiting PKC-NAD(P)H oxidase activation, supporting the notion that this mechanism may be an effective therapeutic target for preventing diabetic vascular complications.
-
Citations
Citations to this article as recorded by- The effects of whey protein on anthropometric parameters, resting energy expenditure, oxidative stress, and appetite in overweight/obese women with type 2 diabetes mellitus: A randomized placebo controlled clinical trial
Maryam Nouri, Bahram Pourghassem Gargari, Zahra Ghasempour, Vahideh Sadra, Mohammad Asghari Jafarabadi, Arvin Babaei, Pedram Tajfar, Ali Tarighat-Esfanjani
International Journal of Diabetes in Developing Countries.2024; 44(1): 155. CrossRef - Rhodanine-benzamides as potential hits for α-amylase enzyme inhibitors and radical (DPPH and ABTS) scavengers
Samuel Attah Egu, Irfan Ali, Khalid Mohammed Khan, Sridevi Chigurupati, Urooj Qureshi, Uzma Salar, Zaheer Ul-Haq, Suliman A. Almahmoud, Shatha Ghazi Felemban, Mohsin Ali, Muhammad Taha
Molecular Diversity.2024;[Epub] CrossRef - Research Progress of FGF-21 and CVAI in Type 2 Diabetic Kidney Disease
央宗 才巴
Advances in Clinical Medicine.2023; 13(07): 12056. CrossRef - Is Subcutaneous Rifamycin Application Superior to Saline Application in Hip Hemiarthroplasty?
Malik Çelik, Nezih Ziroğlu, Alkan Bayrak
Bakirkoy Tip Dergisi / Medical Journal of Bakirkoy.2023; 19(2): 186. CrossRef - In pursuit of incorporation of markers of oxidative stress in traditional biochemical panels in clinical Chemistry: A risk assessment step in diagnosis and biotherapy
John Ibhagbemien Anetor, Chukwuemelie Zedech Uche, Gloria Oiyahumen Anetor
American Journal of Biopharmacy and Pharmaceutical Sciences.2022; 2: 1. CrossRef - Pathophysiologic Mechanisms and Potential Biomarkers in Diabetic Kidney Disease
Chan-Young Jung, Tae-Hyun Yoo
Diabetes & Metabolism Journal.2022; 46(2): 181. CrossRef - p38 MAPK Inhibitor (SB203580) and Metformin Reduces Aortic Protein Carbonyl and Inflammation in Non-obese Type 2 Diabetic Rats
Nuttikarn Nokkaew, Podsawee Mongkolpathumrat, Ruttanapong Junsiri, Supawit Jindaluang, Nichagron Tualamun, Niya Manphatthanakan, Nareumon Saleesee, Marisa Intasang, Jantira Sanit, Punyanuch Adulyaritthikul, Kantapich Kongpol, Sarawut Kumphune, Nitirut Ner
Indian Journal of Clinical Biochemistry.2021; 36(2): 228. CrossRef - Resveratrol-Elicited PKC Inhibition Counteracts NOX-Mediated Endothelial to Mesenchymal Transition in Human Retinal Endothelial Cells Exposed to High Glucose
Roberta Giordo, Gheyath K. Nasrallah, Anna Maria Posadino, Francesco Galimi, Giampiero Capobianco, Ali Hussein Eid, Gianfranco Pintus
Antioxidants.2021; 10(2): 224. CrossRef - BIOLOGICAL ACTIVE COMPONENTS OF SILENE TOMENTELLA AND THEIR PHARMACOLOGICAL PROPERTIES
Ugiloy Yusufovna Yusupova, Nurmurod Sheralievich Ramazonov, Khairulla Mamadievich Bobakulov, Feruza Rustamovna Egamova, Vladimir Nikolaevich Syrov, Durbek Abdikhoshimovich Usmanov
chemistry of plant raw material.2021; (1): 197. CrossRef - Chronically Elevated Exogenous Glucose Elicits Antipodal Effects on the Proteome Signature of Differentiating Human iPSC-Derived Pancreatic Progenitors
Luiza Ghila, Thomas Aga Legøy, Andreas Frøslev Mathisen, Shadab Abadpour, Joao A. Paulo, Hanne Scholz, Helge Ræder, Simona Chera
International Journal of Molecular Sciences.2021; 22(7): 3698. CrossRef - Effect of Type-2 Diabetes Mellitus in Retinopathy Patients on MDA, SOD Activity and its Correlation with HbA1c
Yali Hou, Mei Lin, Xuan Qiu, Mingjuan He, Yu Zhang, Feifei Guo
Brazilian Archives of Biology and Technology.2021;[Epub] CrossRef - Ameliorative effects of Hydrolea zeylanica in streptozotocin-induced oxidative stress and metabolic changes in diabetic rats
Sandeep Kumar Swain, Umesh Chandra Dash, Satish Kanhar, Atish Kumar Sahoo
Journal of Ethnopharmacology.2020; 247: 112257. CrossRef - Imbalance in the antioxidant defence system and pro-genotoxic status induced by high glucose concentrations: In vitro testing in human liver cells
Mattia Acito, Desirée Bartolini, Maria Rachele Ceccarini, Carla Russo, Samuele Vannini, Luca Dominici, Michela Codini, Milena Villarini, Francesco Galli, Tommaso Beccari, Massimo Moretti
Toxicology in Vitro.2020; 69: 105001. CrossRef - Synthesis of sulpha drug based hydroxytriazene derivatives: Anti-diabetic, antioxidant, anti-inflammatory activity and their molecular docking studies
Poonam Sharma, Varsha Dayma, Aparna Dwivedi, Prabhat K. Baroliya, I.P. Tripathi, Murugesan Vanangamudi, R.S. Chauhan, A.K. Goswami
Bioorganic Chemistry.2020; 96: 103642. CrossRef - Analysis of long non-coding RNA expression profiles in high-glucose treated vascular endothelial cells
Erqin Xu, Xiaolei Hu, Xiaoli Li, Guoxi Jin, Langen Zhuang, Qiong Wang, Xiaoyan Pei
BMC Endocrine Disorders.2020;[Epub] CrossRef - Potent α-amylase inhibitors and radical (DPPH and ABTS) scavengers based on benzofuran-2-yl(phenyl)methanone derivatives: Syntheses, in vitro, kinetics, and in silico studies
Irfan Ali, Rafaila Rafique, Khalid Mohammed Khan, Sridevi Chigurupati, Xingyue Ji, Abdul Wadood, Ashfaq Ur Rehman, Uzma Salar, Muhammad Shahid Iqbal, Muhammad Taha, Shahnaz Perveen, Basharat Ali
Bioorganic Chemistry.2020; 104: 104238. CrossRef - A review of fibroblast growth factor 21 in diabetic cardiomyopathy
Xiang Zhang, Luo Yang, Xiongfeng Xu, Fengjuan Tang, Peng Yi, Bo Qiu, Yarong Hao
Heart Failure Reviews.2019; 24(6): 1005. CrossRef - Recent advances in the pathogenesis of microvascular complications in diabetes
Sungmi Park, Hyeon-Ji Kang, Jae-Han Jeon, Min-Ji Kim, In-Kyu Lee
Archives of Pharmacal Research.2019; 42(3): 252. CrossRef - Metabolic syndrome status over 2 years predicts incident chronic kidney disease in mid-life adults: a 10-year prospective cohort study
So Jin Lee, Hun Ju Lee, Hyun jeong Oh, Taehwa Go, Dae Ryong Kang, Jang Young Kim, Ji Hye Huh
Scientific Reports.2018;[Epub] CrossRef - Role of peroxisome proliferator–activated receptor-gamma activation on visfatin, advanced glycation end products, and renal oxidative stress in obesity-induced type 2 diabetes mellitus
A Tabassum, T Mahboob
Human & Experimental Toxicology.2018; 37(11): 1187. CrossRef - Coffee consumption and reduced risk of developing type 2 diabetes: a systematic review with meta-analysis
Mattias Carlström, Susanna C Larsson
Nutrition Reviews.2018; 76(6): 395. CrossRef - Liraglutide ameliorates early renal injury by the activation of renal FoxO1 in a type 2 diabetic kidney disease rat model
Pin Chen, Xiaozhi Shi, Xiangjin Xu, Yiyang Lin, Zhulin Shao, Rongdan Wu, Lihong Huang
Diabetes Research and Clinical Practice.2018; 137: 173. CrossRef - Antioxidant effects of vitamins in type 2 diabetes: a meta-analysis of randomized controlled trials
Maria E. Balbi, Fernanda S. Tonin, Antonio M. Mendes, Helena H. Borba, Astrid Wiens, Fernando Fernandez-Llimos, Roberto Pontarolo
Diabetology & Metabolic Syndrome.2018;[Epub] CrossRef - Gilbert syndrome in patients with type 1 diabetes-Prevalence, glycemic control, and microalbuminuria
Sigal Singer, Nurit Pilpel, Orit Pinhas-Hamiel
Pediatric Diabetes.2017; 18(8): 803. CrossRef - Low serum bilirubin level predicts the development of chronic kidney disease in patients with type 2 diabetes mellitus
Kang Hee Ahn, Sang Soo Kim, Won Jin Kim, Jong Ho Kim, Yun Jeong Nam, Su Bin Park, Yun Kyung Jeon, Bo Hyun Kim, In Joo Kim, Yong Ki Kim
The Korean Journal of Internal Medicine.2017; 32(5): 875. CrossRef - Tiron ameliorates high glucose‐induced cardiac myocyte apoptosis by PKCδ‐dependent inhibition of osteopontin
Ping Jiang, Deling Zhang, Hong Qiu, Xianqi Yi, Yemin Zhang, Yingkang Cao, Bo Zhao, Zhongyuan Xia, Changhua Wang
Clinical and Experimental Pharmacology and Physiology.2017; 44(7): 760. CrossRef - Protective effects of 6-Gingerol on vascular endothelial cell injury induced by high glucose via activation of PI3K-AKT-eNOS pathway in human umbilical vein endothelial cells
Dan Liu, Mengqing Wu, Yi Lu, Tao Xian, Yupeng Wang, Bowei Huang, Guohua Zeng, Qiren Huang
Biomedicine & Pharmacotherapy.2017; 93: 788. CrossRef - Adenosine signaling in diabetes mellitus and associated cardiovascular and renal complications
Maria Peleli, Mattias Carlstrom
Molecular Aspects of Medicine.2017; 55: 62. CrossRef - Diabetes and increased lipid peroxidation are associated with systemic inflammation even in well-controlled patients
Alliny de Souza Bastos, Dana T. Graves, Ana Paula de Melo Loureiro, Carlos Rossa Júnior, Sâmia Cruz Tfaile Corbi, Fausto Frizzera, Raquel Mantuaneli Scarel-Caminaga, Niels Olsen Câmara, Oelisoa M. Andriankaja, Meire I. Hiyane, Silvana Regina Perez Orrico
Journal of Diabetes and its Complications.2016; 30(8): 1593. CrossRef - Agkistrodon acutus-purified protein C activator protects human umbilical vein endothelial cells against H2O2-induced apoptosis
Shu Li, Yun Hong, Xin Jin, Xianwei Li, Entao Sun, Genbao Zhang, Linming Lu, Liuwang Nie
Pharmaceutical Biology.2016; 54(12): 3285. CrossRef - The impact of mast cells on cardiovascular diseases
Eva Kritikou, Johan Kuiper, Petri T. Kovanen, Ilze Bot
European Journal of Pharmacology.2016; 778: 103. CrossRef - Comparison of acarbose and metformin therapy in newly diagnosed type 2 diabetic patients with overweight and/or obesity
Weiping Sun, Chunping Zeng, Lizhen Liao, Juan Chen, Ying Wang
Current Medical Research and Opinion.2016; 32(8): 1389. CrossRef - Mechanisms for the cardiovascular effects of glucagon-like peptide-1
H. Poudyal
Acta Physiologica.2016; 216(3): 277. CrossRef - Integrated scientific data bases review on asulacrine and associated toxicity
Attia Afzal, Muhammad Sarfraz, Zimei Wu, Guangji Wang, Jianguo Sun
Critical Reviews in Oncology/Hematology.2016; 104: 78. CrossRef - Impact of Diabetes and Defective Thyroid Ontogenesis on Audition
Luciene da Cruz Fernandes
Journal of Diabetes, Metabolic Disorders & Control.2016;[Epub] CrossRef - Serum Total Bilirubin Levels Provide Additive Risk Information over the Framingham Risk Score for Identifying Asymptomatic Diabetic Patients at Higher Risk for Coronary Artery Stenosis
Jaechan Leem, Eun Hee Koh, Jung Eun Jang, Chang-Yun Woo, Jin Sun Oh, Min Jung Lee, Joon-Won Kang, Tae-Hwan Lim, Chang Hee Jung, Woo Je Lee, Joong-Yeol Park, Ki-Up Lee
Diabetes & Metabolism Journal.2015; 39(5): 414. CrossRef - Clinical implications of carotid artery intima media thickness assessment on cardiovascular risk stratification in hyperlipidemic Korean adults with diabetes: the ALTO study
Eun-Gyoung Hong, Jung Hun Ohn, Seong Jin Lee, Hyuk Sang Kwon, Sin Gon Kim, Dong Jun Kim, Dong Sun Kim
BMC Cardiovascular Disorders.2015;[Epub] CrossRef - Undiagnosed diabetes is prevalent in younger adults and associated with a higher risk cardiometabolic profile compared to diagnosed diabetes
Yong-ho Lee, Ehrin J. Armstrong, Gyuri Kim, Jaewon Oh, Seok-Min Kang, Byung-Wan Lee, Chul Woo Ahn, Bong Soo Cha, Hyun Chul Lee, Christos S. Mantzoros, Eun Seok Kang
American Heart Journal.2015; 170(4): 760. CrossRef - Common polymorphisms in antioxidant genes are associated with diabetic nephropathy in Type 2 diabetes patients
Jasna Klen, Katja Goričar, Andrej Janež, Vita Dolžan
Personalized Medicine.2015; 12(3): 187. CrossRef - Increased endogenous serotonin level in diabetic conditions may lead to cardiac valvulopathy via reactive oxygen species regulation
Tahir Ali, Hina Waheed, Farhat Shaheen, Madiha Mahmud, Qamar Javed, Iram Murtaza
Biologia.2015; 70(2): 273. CrossRef - Antioxidant Effects of Statins in the Management of Cardiometabolic Disorders
Soo Lim, Philip Barter
Journal of Atherosclerosis and Thrombosis.2014; 21(10): 997. CrossRef - Evidence-Based Practice Use of Incretin-Based Therapy in the Natural History of Diabetes
Stanley Schwartz
Postgraduate Medicine.2014; 126(3): 66. CrossRef - Low serum bilirubin concentration is a novel risk factor for the development of albuminuria in patients with type 2 diabetes
Hiroshi Okada, Michiaki Fukui, Muhei Tanaka, Shinobu Matsumoto, Kanae Kobayashi, Hiroya Iwase, Kiichiro Tomiyasu, Koji Nakano, Goji Hasegawa, Naoto Nakamura
Metabolism.2014; 63(3): 409. CrossRef - Serum total bilirubin levels and prevalence of diabetic retinopathy in a Chinese population (中国人群血清总胆红素水平与糖尿病视网膜病变相关性的研究)
Syeda Sadia Najam, Jichao Sun, Jie Zhang, Min Xu, Jieli Lu, Kan Sun, Mian Li, Tiange Wang, Yufang Bi, Guang Ning
Journal of Diabetes.2014; 6(3): 221. CrossRef - Roles of oxidative stress, adiponectin, and nuclear hormone receptors in obesity-associated insulin resistance and cardiovascular risk
Morihiro Matsuda, Iichiro Shimomura
Hormone Molecular Biology and Clinical Investigation.2014;[Epub] CrossRef - Unilateral injection of Aβ25–35 in the hippocampus reduces the number of dendritic spines in hyperglycemic rats
Zayda Lazcano, Oscar Solis, María Elena Bringas, Daniel Limón, Alfonso Diaz, Blanca Espinosa, Isabel García‐Peláez, Gonzalo Flores, Jorge Guevara
Synapse.2014; 68(12): 585. CrossRef - Role of angiotensin-converting enzyme 2 (ACE2) in diabetic cardiovascular complications
Vaibhav B. Patel, Nirmal Parajuli, Gavin Y. Oudit
Clinical Science.2014; 126(7): 471. CrossRef - Pathogenesis of Chronic Hyperglycemia: From Reductive Stress to Oxidative Stress
Liang-Jun Yan
Journal of Diabetes Research.2014; 2014: 1. CrossRef - Daily intake of vitamin D‐ or calcium‐vitamin D‐fortified Persian yogurt drink (doogh) attenuates diabetes‐induced oxidative stress: evidence for antioxidative properties of vitamin D
B. Nikooyeh, T. R. Neyestani, N. Tayebinejad, H. Alavi‐Majd, N. Shariatzadeh, A. Kalayi, M. Zahedirad, S. Heravifard, S. Salekzamani
Journal of Human Nutrition and Dietetics.2014; 27(s2): 276. CrossRef - Roles of adiponectin and oxidative stress in obesity-associated metabolic and cardiovascular diseases
Morihiro Matsuda, Iichiro Shimomura
Reviews in Endocrine and Metabolic Disorders.2014; 15(1): 1. CrossRef - PKCδ-dependent Activation of the Ubiquitin Proteasome System is Responsible for High Glucose-induced Human Breast Cancer MCF-7 Cell Proliferation, Migration and Invasion
Shan Zhu, Feng Yao, Wen-Huan Li, Jin-Nan Wan, Yi-Min Zhang, Zhao Tang, Shahzad Khan, Chang-Hua Wang, Sheng-Rong Sun
Asian Pacific Journal of Cancer Prevention.2013; 14(10): 5687. CrossRef - Increased oxidative stress in obesity: Implications for metabolic syndrome, diabetes, hypertension, dyslipidemia, atherosclerosis, and cancer
Morihiro Matsuda, Iichiro Shimomura
Obesity Research & Clinical Practice.2013; 7(5): e330. CrossRef - Hydrogen Sulfide Suppresses High Glucose–Induced Expression of Intercellular Adhesion Molecule-1 in Endothelial Cells
Qingbo Guan, Xiaolei Wang, Ling Gao, Jicui Chen, Yuantao Liu, Chunxiao Yu, Nan Zhang, Xu Zhang, Jiajun Zhao
Journal of Cardiovascular Pharmacology.2013; 62(3): 278. CrossRef - Clinical Marker of Platelet Hyperreactivity in Diabetes Mellitus
Jin Hwa Kim, Hak Yeon Bae, Sang Yong Kim
Diabetes & Metabolism Journal.2013; 37(6): 423. CrossRef - Glucose initially inhibits and later stimulates blood ROS generation
Thomas Stief
Journal of Diabetes Mellitus.2013; 03(01): 15. CrossRef - Oxidative Stress in Cardiovascular Diseases and Obesity: Role of p66Shc and Protein Kinase C
Elena De Marchi, Federica Baldassari, Angela Bononi, Mariusz R. Wieckowski, Paolo Pinton
Oxidative Medicine and Cellular Longevity.2013; 2013: 1. CrossRef - Toxicological and pharmacological concerns on oxidative stress and related diseases
Soodabeh Saeidnia, Mohammad Abdollahi
Toxicology and Applied Pharmacology.2013; 273(3): 442. CrossRef - Comparison of antioxidant, α-glucosidase inhibition and anti-inflammatory activities of the leaf and root extracts ofSmilax chinaL.
Kyoung Kon Kim, Yun Hwan Kang, Dae Jung Kim, Tae Woo Kim, Myeon Choe
Journal of Nutrition and Health.2013; 46(4): 315. CrossRef - Correlation between blood glucose fluctuations and activation of oxidative stress in type 1 diabetic children during the acute metabolic disturbance period
Di WU, Chun-xiu GONG, Xi MENG, Qiu-lan YANG
Chinese Medical Journal.2013; 126(21): 4019. CrossRef - Oxidative stress and its complications in human health
Guniz M. Koksal
Advances in Bioscience and Biotechnology.2012; 03(08): 1113. CrossRef
- The effects of whey protein on anthropometric parameters, resting energy expenditure, oxidative stress, and appetite in overweight/obese women with type 2 diabetes mellitus: A randomized placebo controlled clinical trial
- Decreased Expression and Induced Nucleocytoplasmic Translocation of Pancreatic and Duodenal Homeobox 1 in INS-1 Cells Exposed to High Glucose and Palmitate
- Gyeong Ryul Ryu, Jun Mo Yoo, Esder Lee, Seung-Hyun Ko, Yu-Bae Ahn, Ki-Ho Song
- Diabetes Metab J. 2011;35(1):65-71. Published online February 28, 2011
- DOI: https://doi.org/10.4093/dmj.2011.35.1.65
- 3,034 View
- 37 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Type 2 diabetes mellitus (T2DM) is often accompanied by increased levels of circulating fatty acid. Elevations in fatty acids and glucose for prolonged periods of time have been suggested to cause progressive dysfunction or apoptosis of pancreatic beta cells in T2DM. However, the precise mechanism of this adverse effect is not well understood.
Methods INS-1 rat-derived insulin-secreting cells were exposed to 30 mM glucose and 0.25 mM palmitate for 48 hours.
Results The production of reactive oxygen species increased significantly. Pancreatic and duodenal homeobox 1 (Pdx1) expression was down-regulated, as assessed by reverse transcription-polymerase chain reaction and Western blot analyses. The promoter activities of insulin and Pdx1 were also diminished. Of note, there was nucleocytoplasmic translocation of Pdx1, which was partially prevented by treatment with an antioxidant, N-acetyl-L-cysteine.
Conclusion Our data suggest that prolonged exposure of beta cells to elevated levels of glucose and palmitate negatively affects Pdx1 expression via oxidative stress.
-
Citations
Citations to this article as recorded by- Nrf2 Activation Protects Mouse Beta Cells from Glucolipotoxicity by Restoring Mitochondrial Function and Physiological Redox Balance
Johanna Schultheis, Dirk Beckmann, Dennis Mulac, Lena Müller, Melanie Esselen, Martina Düfer
Oxidative Medicine and Cellular Longevity.2019; 2019: 1. CrossRef - Early overnutrition reduces Pdx1 expression and induces β cell failure in Swiss Webster mice
Maria M. Glavas, Queenie Hui, Eva Tudurí, Suheda Erener, Naomi L. Kasteel, James D. Johnson, Timothy J. Kieffer
Scientific Reports.2019;[Epub] CrossRef - Anti-diabetic effect of mulberry leaf polysaccharide by inhibiting pancreatic islet cell apoptosis and ameliorating insulin secretory capacity in diabetic rats
Yao Zhang, Chunjiu Ren, Guobing Lu, Zhimei Mu, Weizheng Cui, Huiju Gao, Yanwen Wang
International Immunopharmacology.2014; 22(1): 248. CrossRef - The Furan Fatty Acid Metabolite CMPF Is Elevated in Diabetes and Induces β Cell Dysfunction
Kacey J. Prentice, Lemieux Luu, Emma M. Allister, Ying Liu, Lucy S. Jun, Kyle W. Sloop, Alexandre B. Hardy, Li Wei, Weiping Jia, I. George Fantus, Douglas H. Sweet, Gary Sweeney, Ravi Retnakaran, Feihan F. Dai, Michael B. Wheeler
Cell Metabolism.2014; 19(4): 653. CrossRef
- Nrf2 Activation Protects Mouse Beta Cells from Glucolipotoxicity by Restoring Mitochondrial Function and Physiological Redox Balance
- The Association between Serum GGT Concentration and Diabetic Peripheral Polyneuropathy in Type 2 Diabetic Patients
- Ho Chan Cho
- Korean Diabetes J. 2010;34(2):111-118. Published online April 30, 2010
- DOI: https://doi.org/10.4093/kdj.2010.34.2.111
- 4,250 View
- 39 Download
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Diabetic peripheral polyneuropathy (DPP) is one of the common complications of diabetes mellitus (DM) and can lead to foot ulcers or amputation. The pathophysiology of DPP includes several factors such as metabolic, vascular, autoimmune, oxidative stress and neurohormonal growth-factor deficiency and recent studies have suggested the use of serum gamma-glutamyl transferase (GGT) as an early marker of oxidative stress. Therefore, we investigated whether serum GGT may be useful in predicting DPP.
Methods We assessed 90 patients with type 2 DM who were evaluated for the presence of DPP using clnical neurologic examinations including nerve conduction velocity studies. We evaluated the association between serum GGT and the presence of DPP.
Results The prevalence of DPP was 40% (36 cases) according to clinical neurological examinations. The serum GGT concentration was significantly elevated in type 2 diabetic patients with DPP compared to patients without DPP (
P < 0.01). There were other factors significantly associated with DPP including smoking (P = 0.019), retinopathy (P = 0.014), blood pressure (P < 0.05), aspartate aminotransferase (P = 0.022), C-reactive protein (P = 0.036) and urine microalbumin/creatinine ratio (P = 0.004). Serum GGT was independently related with DPP according to multiple logistic analysis (P < 0.01).Conclusion This study shows that increased levels of serum GGT may have important clinical implications in the presence of DPP in patients with type 2 diabetes.
-
Citations
Citations to this article as recorded by- Validation of the Framingham Diabetes Risk Model Using Community-Based KoGES Data
Hye Ah Lee, Hyesook Park, Young Sun Hong
Journal of Korean Medical Science.2024;[Epub] CrossRef - Liver enzymes and risk of ocular motor cranial nerve palsy: a nationwide population-based study
Joonhyoung Kim, Kyungdo Han, Juhwan Yoo, Kyung-Ah Park, Sei Yeul Oh
Neurological Sciences.2022; 43(5): 3395. CrossRef - Validity of the diagnosis of diabetic microvascular complications in Korean national health insurance claim data
Hyung Jun Kim, Moo-Seok Park, Jee-Eun Kim, Tae-Jin Song
Annals of Clinical Neurophysiology.2022; 24(1): 7. CrossRef - The association of liver enzymes with diabetes mellitus risk in different obesity subgroups: A population-based study
Dinghao Zheng, Xiaoyun Zhang, Lili You, Feng Li, Diaozhu Lin, Kan Sun, Meng Ren, Li Yan, Wei Wang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Early Biomarkers of Neurodegenerative and Neurovascular Disorders in Diabetes
Aleksandra Gasecka, Dominika Siwik, Magdalena Gajewska, Miłosz J. Jaguszewski, Tomasz Mazurek, Krzysztof J. Filipiak, Marek Postuła, Ceren Eyileten
Journal of Clinical Medicine.2020; 9(9): 2807. CrossRef - Dissociable Contributions of Precuneus and Cerebellum to Subjective and Objective Neuropathy in HIV
Natalie M. Zahr, Kilian M. Pohl, Adolf Pfefferbaum, Edith V. Sullivan
Journal of Neuroimmune Pharmacology.2019; 14(3): 436. CrossRef - Evaluation of Serum Gamma Glutamyl Transferase Levels in Diabetic Patients With and Without Retinopathy
Neda Valizadeh, Rasoul Mohammadi, Alireza Mehdizadeh, Qader Motarjemizadeh, Hamid Reza Khalkhali
Shiraz E-Medical Journal.2018;[Epub] CrossRef - The Effect of Cigarette Smoking on Diabetic Peripheral Neuropathy: A Systematic Review and Meta-Analysis
Carole Clair, Marya J. Cohen, Florian Eichler, Kevin J. Selby, Nancy A. Rigotti
Journal of General Internal Medicine.2015; 30(8): 1193. CrossRef - Evaluation of oxidative stress markers and vascular risk factors in patients with diabetic peripheral neuropathy
Noha Ahmed El Boghdady, Gamal Ali Badr
Cell Biochemistry and Function.2012; 30(4): 328. CrossRef - Angiotensin-converting enzyme gene single polymorphism as a genetic biomarker of diabetic peripheral neuropathy: longitudinal prospective study
J. Jurado, J. Ybarra, J.H. Romeo, M. Garcia, E. Zabaleta-del-Olmo
Journal of Diabetes and its Complications.2012; 26(2): 77. CrossRef - Routine enzymes in the monitoring of type 2 diabetes mellitus
Osman Evliyaoğlu, Erkan Kibrisli, Yaşar Yildirim, Osman Gökalp, Leyla Çolpan
Cell Biochemistry and Function.2011; 29(6): 506. CrossRef - Antioxidant Effects of Fermented Red Ginseng Extracts in Streptozotocin-Induced Diabetic Rats
Hyun-Jeong Kim, Sung-Gyu Lee, In-Gyeong Chae, Mi-Jin Kim, Nam-Kyung Im, Mi-Hee Yu, Eun-Ju Lee, In-Seon Lee
Journal of Ginseng Research.2011; 35(2): 129. CrossRef - Serum γ‐glutamyltransferase and associated damage among a She Chinese population
Y. Lin, Y. Xu, G. Chen, B. Huang, J. Yao, Z. Chen, L. Yao, F. Lin, Y. Qiao, Z. Chen, S. Zhu, H. Huang, J. Wen
Diabetic Medicine.2011; 28(8): 924. CrossRef
- Validation of the Framingham Diabetes Risk Model Using Community-Based KoGES Data
- High Glucose and/or Free Fatty Acid Damage Vascular Endothelial Cells via Stimulating of NAD(P)H Oxidase-induced Superoxide Production from Neutrophils.
- Sang Soo Kim, Sun Young Kim, Soo Hyung Lee, Yang Ho Kang, In Ju Kim, Yong Ki Kim, Seok Man Son
- Korean Diabetes J. 2009;33(2):94-104. Published online April 1, 2009
- DOI: https://doi.org/10.4093/kdj.2009.33.2.94
- 2,222 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Oxidative stress and inflammation are important factors in the pathogenesis of diabetes and contribute to the development of diabetic complications. To understand the mechanisms that cause vascular complications in diabetes, we examined the effects of high glucose and/or free fatty acids on the production of superoxide from neutrophils and their role in endothelial cell damage. METHODS: Human neutrophils were incubated in the media containing 5.5 mM D-glucose, 30 mM D-glucose, 3 nM oleic acid, or 30 microM oleic acid for 1 hour to evaluate superoxide production through NAD(P)H oxidase activation. Human aortic endothelial cells were co-cultured with neutrophils exposed to high glucose and oleic acid. We then measured neutrophil adhesion to endothelial cells, neutrophil activation and superoxide production, neutrophil-mediated endothelial cell cytotoxicity and subunits of neutrophil NAD(P)H oxidase. RESULTS: After 1 hour of incubation with various concentrations of glucose and oleic acid, neutrophil adherence to high glucose and oleic acid-treated endothelial cells was significantly increased compared with adhesion to low glucose and oleic acid-treated endothelial cells. Incubation of neutrophils with glucose and free fatty acids increased superoxide production in a dose-dependent manner. High glucose and oleic acid treatment significantly increased expression of the membrane components of NAD(P)H oxidase of neutrophil (gp91(phox)). Endothelial cells co-cultured with neutrophils exposed to high glucose and oleic acid showed increased cytolysis, which could be prevented by an antioxidant, N-acetylcysteine. CONCLUSION: These results suggest that high glucose and/orfree fatty acidsincrease injury of endothelial cells via stimulating NAD(P)H oxidase-induced superoxide production from neutrophils.
- Oxidative Stress and Cell Dysfunction in Diabetes: Role of ROS Produced by Mitochondria and NAD(P)H Oxidase.
- Sang Soo Kim, Seok Man Son
- Korean Diabetes J. 2008;32(5):389-398. Published online October 1, 2008
- DOI: https://doi.org/10.4093/kdj.2008.32.5.389
- 2,153 View
- 60 Download
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF - Oxidative stress has been considered to be a major contributor to the pathogenesis of the diabetic macrovascular and microvascular complications. In the absence of an appropriate antioxidant defense mechanism, increased oxidative stress leads to the activation of stress-sensitive intracellular signaling pathways and the formation of gene products that cause damage and contribute to the late complications ofdiabetes. The source of reactive oxygen species (ROS) in the pancreatic beta cells and insulin sensitive cells has postulated to be the mitochondrial electron transport chain. NAD(P)H oxidase-dependent ROS production is also important as the source both in pancreatic beta cells and other cells. NAD(P)H oxidase mediated ROS can alter parameters of signal transduction, insulin secretion, insulin action, cell proliferation and cell death. Additionally, oxidative stress as the pathogenic mechanism linking insulin resistance with dysfunction of both pancreatic beta cells and endothelial cells, eventually leads to diabetes and its complications. Further investigation of the mechanisms and its therapeutic interventions based on focusing NAD(P)H oxidase associated ROS production in the islet cells and other islet cells are needed
-
Citations
Citations to this article as recorded by- Cytoprotective Effect of Hot-Water Extracts of Protaetia brevitarsis seulensis Larvae in Cisplatin-Treated Macrophages
Bo-Gyeong Yoo, Jun-Pyo Hong, Ha-Yeon Song, Eui-Hong Byun
Journal of the Korean Society of Food Science and Nutrition.2022; 51(12): 1252. CrossRef - The Effects of LR and SP Acupuncture on Renal Damage in Streptozotocin-induced Diabetic Mice
Cho In Lee, Hyun Jong Lee, Yun Kyu Lee, Seong Chul Lim, Jae Soo Kim
The Acupuncture.2015; 32(3): 41. CrossRef - Effect of Chungkukjang supplementation on oxidative stress and antioxidant nutrients of diabetic rats induced by streptozotocin
Heyun-Sook Park, Hyun-Joo Kong, Eon-Hee Lee, Eun-Mi Choi, Joung-Hyeon Jang, Myoung-Hee Lee, Ju-Yeon Hong, Su-Jung Hwang, Hyeon-A Jung, Kyung-Mi Yang
Korean Journal of Food Preservation.2015; 22(2): 281. CrossRef - The Effects of Several Halophytes on Insulin Resistance in Otsuka Long-evans Tokushima Fatty Rats
Jeong-Yong Cho, Zhangjun Huang, Sun-Young Park, Kyung-Hee Park, Tong-Kun Pai, So-Young Kim, Haeng-Ran Kim, Kyung-Sik Ham
Korean Journal of Food Science and Technology.2014; 46(1): 100. CrossRef - Protective Effects of Radiation-induced Blackberry Mutant Extract on Carbon Tetrachloride (CCl4)-induced Liver Injury in Sprague-Dawley Rats
Byoung Ok Cho, Chang-Wook Lee, Yangkang So, Chang-Hyun Jin, Hong-Sun Yook, Myung-Woo Byun, Yong-Wook Jeong, Jong Chun Park, Il-Yun Jeong
Journal of the Korean Society of Food Science and Nutrition.2014; 43(6): 807. CrossRef - Antioxidant Activities and α-Glucosidase Inhibitory Effect of Water Extracts from Medicinal Plants
Hyun Sook Kim, Tae Woo Kim, Dae Jung Kim, Jae Sung Lee, Kyoung Kon Kim, Myeon Choe
Korean Journal of Medicinal Crop Science.2013; 21(3): 197. CrossRef - Antioxidant Effect of Hot water and Ethanol extracts from Cheonnyuncho (Opuntia humifusa) on Reactive Oxygen Species (ROS) Production in 3T3-L1 Adipocytes
Bo-Ra Yoon, Young-Jun Lee, Sun-Gu Kim, Jung-Young Jang, Hyo-Ku Lee, Seong-Kap Rhee, Hee-Do Hong, Hyeon-Son Choi, Boo-Yong Lee, Ok-Hwan Lee
Korean Journal of Food Preservation.2012; 19(3): 443. CrossRef - Inhibitory Effects of Panax ginseng C. A. Mayer Treated with High Temperature and High Pressure on Oxidative Stress
Bo-Ra Yoon, Young-Jun Lee, Hee-Do Hong, Young-Chul Lee, Young-Chan Kim, Young Kyoung Rhee, Kyung-Tack Kim, Ok-Hwan Lee
The Korean Journal of Food And Nutrition.2012; 25(4): 800. CrossRef - Effect of Dietary Supplementation of β-Carotene on Hepatic Antioxidant Enzyme Activities and Glutathione Concentration in Diabetic Rats
Jung-Hyun Jang, Kyeung-Soon Lee, Jung-Sook Seo
Journal of the Korean Society of Food Science and Nutrition.2011; 40(8): 1092. CrossRef - An Association between 609 C →T Polymorphism in NAD(P)H: Quinone Oxidoreductase 1 (NQO1) Gene and Blood Glucose Levels in Korean Population
Dohee Kim
Korean Diabetes Journal.2009; 33(1): 24. CrossRef
- Cytoprotective Effect of Hot-Water Extracts of Protaetia brevitarsis seulensis Larvae in Cisplatin-Treated Macrophages
- Migration of Vascular Smooth Muscle Cells by High Glucose is Reactive Oxygen Dependent.
- Yong Seong An, Ji Hae Kwon, Yang Ho Kang, In Ju Kim, Yong Ki Kim, Seok Man Son
- Korean Diabetes J. 2008;32(3):185-195. Published online June 1, 2008
- DOI: https://doi.org/10.4093/kdj.2008.32.3.185
- 1,937 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Oxidative stress contributes to vascular diseases in patients with diabetes. As the mechanism of development and progression of diabetic vascular complications is poorly understood, this study was aimed to assess the potential role of hyperglycemia-induced oxidative stress and to determine whether the oxidative stress is a major factor in hyperglycemia-induced migration of vascular smooth muscle cells (VSMCs). METHODS: We treated primary cultured rat aortic smooth muscle cells for 72 hours with medium containing 5.5 mM D-glucose (normal glucose), 30 mM D-glucose (high glucose) or 5.5 mM D-glucose plus 24.5 mM mannitol (osmotic control). We measured the migration of VSMCs and superoxide production. Immunoblotting of PKC isozymes using phoshospecific antibodies was performed, and PKC activity was also measured. RESULTS: Migration of VSMCs incubated under high glucose condition were markedly increased compared to normal glucose condition. Treatment with diphenyleneiodonium (DPI, 10 micromol/L) and superoxide dismutase (SOD, 500 U/mL) significantly suppressed high glucose-induced migration of VSMCs. Superoxide production was significantly increased in high glucose condition and was markedly decreased after treatment with DPI and SOD. High glucose also markedly increased activity of PKC-delta isozyme. When VSMCs were treated with rottlerin or transfected with PKC-delta siRNA, nitro blue tetrazolium (NBT) staining and NAD(P)H oxidase activity were significantly attenuated in the high glucose-treated VSMCs. Furthermore, inhibition of PKC-delta markedly decreased VSMC migration by high glucose. CONCLUSION: These results suggest that high glucose-induced VSMC migration is dependent upon activation of PKC-delta, which may responsible for elevated intracellular ROS production in VSMCs, and this is mediated by NAD(P)H oxidase.
- The Protective Effect of EGCG on INS-1 Cell in the Oxidative Stress and Mechanism.
- Mi Kyung Kim, Hye Sook Jung, Chang Shin Yoon, Min Jeong Kwon, Kyung Soo Koh, Byung Doo Rhee, Jeong Hyun Park
- Korean Diabetes J. 2008;32(2):121-130. Published online April 1, 2008
- DOI: https://doi.org/10.4093/kdj.2008.32.2.121
- 2,057 View
- 24 Download
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Oxidative stress is important in both diabetic complications and the development and the progression of type 2 diabetes via the effects on the pancreatic beta-cells. EGCG (epigallocatechin galleate), a major constituent of green tea, has been known to have beneficial effects on various diseases through the mechanisms of antioxidant and cell signaling modulation. But, very small numbers of studies were published about the direct effects of EGCG on the pancreatic beta cell lines. We performed this study to see the protective effect of EGCG on pancreatic beta cell line under H2O2 and the mechanisms of this phenomenon. METHODS: We used INS-1 cells and hydrogen peroxide as an oxidative stressor. Their viabilities were verified by MTT assay and FACS. The activity of glutathione peroxidase was assessed by total glutathione quantification kit. Western blot and semi-quantitative RT-PCR for the catalase, SOD (superoxide dismutase), PI3K and Akt were performed. Functional status of INS-1 cells was tested by GSIS (glucose stimulated insulin secretion). RESULTS: The biological effects of EGCG were different according to its concentrations. 10 micrometer EGCG effectively protected hydrogen peroxide induced damage in INS-1 cells. The expression and the activity of SOD, catalase and the glutathione peroxidase were significantly increased by EGCG. EGCG significantly increased PI3K and Akt activity and its effect was inhibited partially by wortmannin. GSIS was well preserved by EGCG. CONCLUSION: EGCG in low concentration effectively protected INS-1 cells from the oxidative stress through the activation of both antioxidant systems and anti-apoptosis signaling. Further studies will be necessary for the more detailed mechanisms and the clinical implications. -
Citations
Citations to this article as recorded by- Suppressive Effects of Epigallocatechin Gallate Pretreatment on the Expression of Inflammatory Cytokines in RAW264.7 Cells Activated by Lipopolysaccharide
Eun Ji Seo, Jun Go, Ji Eun Kim, Eun Kyoung Koh, Sung Hwa Song, Ji Eun Sung, Chan Kyu Park, Hyun Ah Lee, Dong Seob Kim, Hong Joo Son, Cung Yeoul Lee, Hee Seob Lee, Dae Youn Hwang
Journal of Life Science.2015; 25(9): 961. CrossRef - The Protective Effects of Chrysanthemum cornarium L. var. spatiosum Extract on HIT-T15 Pancreatic β-Cells against Alloxan-induced Oxidative Stress
In-Hye Kim, Kang-Jin Cho, Jeong-Sook Ko, Jae-Hyun Kim, Ae-Son Om
The Korean Journal of Food And Nutrition.2012; 25(1): 123. CrossRef - Protective Effects of Sasa Borealis Leaves Extract on High Glucose-Induced Oxidative Stress in Human Umbilical Vein Endothelial Cells
Ji-Young Hwang, Ji-Sook Han
Journal of the Korean Society of Food Science and Nutrition.2010; 39(12): 1753. CrossRef
- Suppressive Effects of Epigallocatechin Gallate Pretreatment on the Expression of Inflammatory Cytokines in RAW264.7 Cells Activated by Lipopolysaccharide

 KDA
KDA
 First
First Prev
Prev





