- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 42(5); 2018 > Article
-
Original ArticleEpidemiology Ten-Year Mortality Trends for Adults with and without Diabetes Mellitus in South Korea, 2003 to 2013
-
Kyeong Jin Kim1, Tae Yeon Kwon2, Sungwook Yu3, Ji A Seo1, Nan Hee Kim1, Kyung Mook Choi1, Sei Hyun Baik1, Dong Seop Choi1, Sin Gon Kim1, Yousung Park4
 , Nam Hoon Kim1
, Nam Hoon Kim1
-
Diabetes & Metabolism Journal 2018;42(5):394-401.
DOI: https://doi.org/10.4093/dmj.2017.0088
Published online: April 26, 2018
1Division of Endocrinology and Metabolism, Department of Internal Medicine, Korea University College of Medicine, Seoul, Korea.
2Department of International Finance, Hankuk University of Foreign Studies, Yongin, Korea.
3Department of Neurology, Korea University College of Medicine, Seoul, Korea.
4Department of Statistics, Korea University, Seoul, Korea.
- Corresponding author: Nam Hoon Kim. Division of Endocrinology and Metabolism, Department of Internal Medicine, Korea University Anam Hospital, Korea University College of Medicine, 73 Inchon-ro, Seongbuk-gu, Seoul 02841, Korea. pourlife@korea.ac.kr
- Corresponding author: Yousung Park. Department of Statistics, Korea University, 145 Anam-ro, Seongbuk-gu, Seoul 02841, Korea. yspark@korea.ac.kr
- *Kyeong Jin Kim and Tae Yeon Kwon contributed equally to this study as first authors.
Copyright © 2018 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Background
- To estimate and compare the trends of all-cause and cause-specific mortality rates for subjects with and without diabetes in South Korea, from 2003 to 2013.
-
Methods
- Using a population-based cohort (2003 to 2013), we evaluated annual mortality rates in adults (≥30 years) with and without diabetes. The number of subjects in this analysis ranged from 585,795 in 2003 to 670,020 in 2013.
-
Results
- Age- and sex-adjusted all-cause mortality rates decreased consistently in both groups from 2003 to 2013 (from 14.4 to 9.3/1,000 persons in subjects with diabetes and from 7.9 to 4.4/1,000 persons in those without diabetes). The difference in mortality rates between groups also decreased (6.61 per 1,000 persons in 2003 to 4.98 per 1,000 persons in 2013). The slope associated with the mortality rate exhibited a steeper decrease in subjects with diabetes than those without diabetes (regression coefficients of time: −0.50 and −0.33, respectively; P=0.004). In subjects with diabetes, the mortality rate from cardiovascular disease decreased by 53.5% (from 2.73 to 1.27 per 1,000 persons, P for trend <0.001). Notably, the decrease in mortality from ischemic stroke (79.2%, from 1.20 to 0.25 per 1,000 persowns) was more profound than that from ischemic heart disease (28.3%, from 0.60 to 0.43 per 1,000 persons).
-
Conclusion
- All-cause and cardiovascular mortality rates decreased substantially from 2003 to 2013, and the decline in ischemic stroke mortality mainly contributed to the decreased cardiovascular mortality in Korean people with diabetes.
- Diabetes is a major public health problem in modern society because of its increasing prevalence and associated morbidity and mortality [1]. The mortality rate of patients with diabetes was reported to be 2- to 3-fold higher than that of the general population [23]. Along with progress in diabetes care, especially in the management of cardiovascular disease (CVD) risks [4], substantial decreases in overall, and CVD mortality rates have been observed in participants with diabetes [567]. Several studies have even reported a decreased gap in mortality rates between individuals with and without diabetes [2]. However, other studies have shown an increase in diabetes-related mortality [89]. This discrepancy is likely to be due to differences in study populations or regions, as well as the period in which the studies were conducted.
- In developing countries in Asia, diabetes has become a serious health problem [101112]. According to the World Health Organization, approximately 80% of diabetes-related deaths occurred in low- and middle-income countries, including many Asian countries [11]. However, information on diabetes-related mortality in this region is insufficient and outdated. A previous report from South Korea showed that mortality rates for people with diabetes increased continuously from 1983 to 2001 [9]. However, some evidence indicates that diabetes care has improved and treatment rates for diabetes-related conditions have increased in South Korea [1314]. Thus, more recent and accurate evidence is required because such data would profoundly influence general public health policies.
- We aimed to assess and compare all-cause and CVD mortality rates and recent trends for subjects with and without diabetes using a nationwide population-based cohort (2003 to 2013).
INTRODUCTION
- Study population
- The Korean National Health Insurance Service (NHIS) is responsible for health insurance and health promotion programs for all citizens of South Korea. Recently, the Korean NHIS released a National Sample Cohort (2002 to 2013) database comprising the data of 1,025,340 Koreans (approximately 2.2% of the total South Korean population in 2002) who were followed up until 2013, with samples for newborn infants updated annually. The database included information on medical care of the individuals, disease history, health check-up data, and basic demographic information. In addition, the database was merged with death records kept by the Korean National Statistical Office. More detailed descriptions of the NHIS study protocol and methods have been published elsewhere [15].
- We divided all subjects from the database into two groups based on their diabetes status: those with diabetes mellitus (DM) group and those without (non-DM) group. Diabetes was defined as the clinical and pharmacy codes (E10–E14) for diabetes from the International Classification of Disease, 10th revision (ICD-10, Korean version).
- Determination of cause of death
- The date of death was identified in the cohort database. The cause of death was categorized in accordance with the ICD-10 codes: total CVD (I00–I99), ischemic heart disease (I20–I25), and ischemic stroke (I63–I66).
- Ethics approval and consent to participate
- This study was approved by the Institutional Review Board of Korea University Hospital (IRB number: ED14188). Informed consent was not obtained specifically because this study was based on the NHIS data which were fully anonymized and deidentified for the analysis.
- Statistical analysis
- To control for the effects of the different population structures of the two groups, we used standardized death rates and adjusted them for age and sex, using the 2003 population structure in the NHIS cohort data as the reference group [16]. The rates were then normalized to a common baseline to allow comparisons. The direct standardization method was calculated based on the following equation:
- Here, the entire study population was divided into K age-sex groups. Pk is the proportion of the kth group in the 2003 reference population and dk the death rate of the kth group of the study population. We also calculated 95% confidence intervals for the standardized death rates, as described previously [17]. To analyze the time trends of the age- and sex-adjusted standardized death rates in the DM and non-DM groups, we fitted a simple regression model to each standardized death rate over time. Each time trend was then tested under a two-sided assumption, and its significance was addressed when the P value was <0.05.
- All statistical analyses were performed using SAS version 9.4 software (SAS Institute Inc., Cary, NC, USA).
METHODS
- The total number of subjects in this analysis ranged from 585,795 in 2003 to 670,020 in 2013. During this period, a total of 54,568 deaths occurred: 17,101 in the DM group and 37,467 in the non-DM group. The crude numbers and rates of death are displayed in the Table 1. In both groups, the death rates from CVD continuously declined over time.
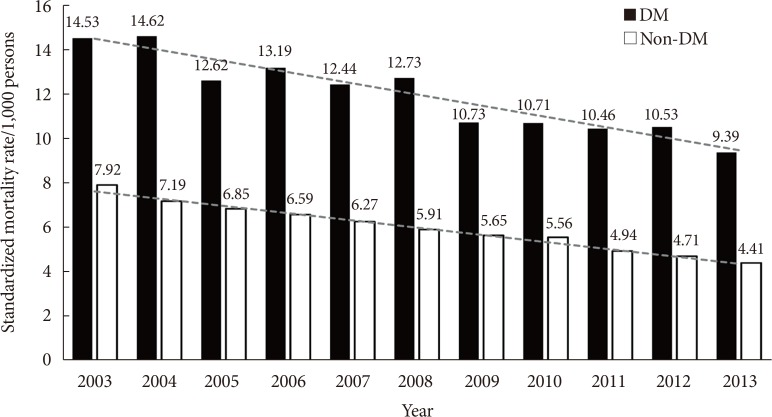
- Fig. 1 shows the annual trends of the standardized mortality rates (per 1,000 persons) in both groups from 2003 to 2013. The all-cause standardized mortality rates consistently decreased in both groups: from 14.5 per 1,000 persons in 2003 to 9.4 per 1,000 persons in 2013 in the DM group and from 7.9 per 1,000 persons to 4.4 per 1,000 persons in the non-DM group (P value for trend <0.001 in both groups). In addition, the difference in the mortality rate for subjects with diabetes relative to those without diabetes also decreased from 2003 to 2013 (from 6.61 per 1,000 persons in 2003 to 4.98 per 1,000 persons in 2013).
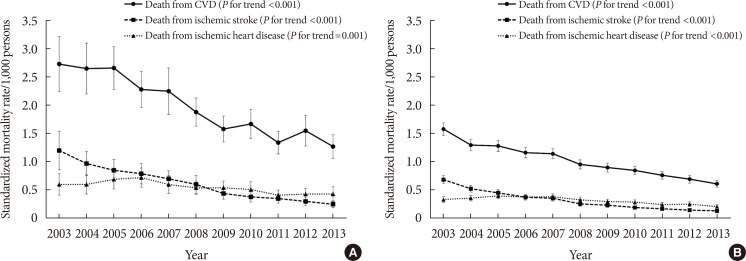
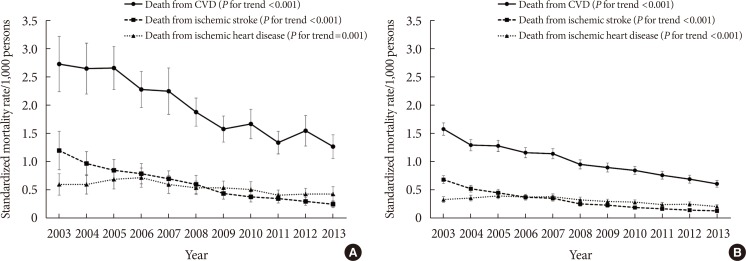
- We also assessed the cause-specific standardized mortality rates from total CVD and CVD subtypes. Fig. 2A shows those annual trends in subjects with diabetes. Similar to the trends for all-cause mortality, the rate of CVD mortality decreased significantly by 53.5% in subjects with diabetes (from 2.73 to 1.27 per 1,000 persons, P for trend <0.001). Deaths from ischemic stroke (from 1.20 to 0.25 per 1,000 persons, P for trend <0.001) accounted for a larger proportion of that reduction compared to deaths from ischemic heart disease (from 0.60 to 0.43 per 1,000 persons, P for trend=0.001). Similar trends of CVD mortality decline were found in subjects without diabetes (Fig. 2B).
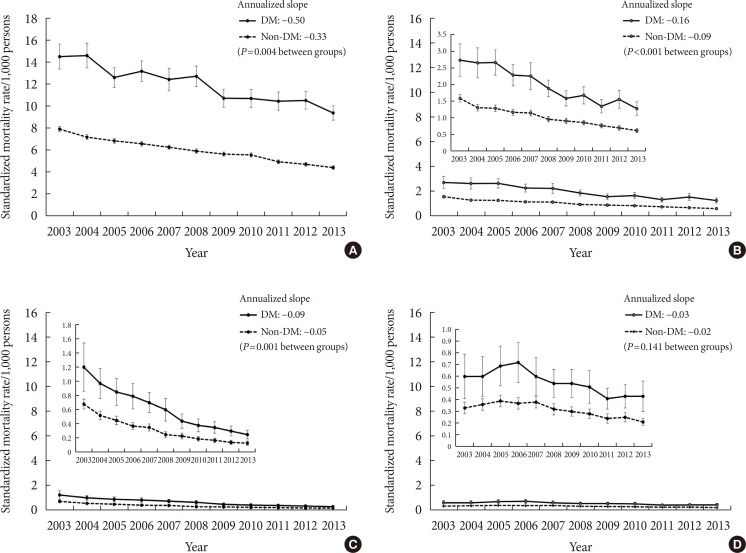
- To compare the decreasing trends in mortality rates between subjects with and without diabetes, we measured the annualized slope of decline in both groups. The rate of decline was 1.52-fold greater in the DM group than in the non-DM group (regression coefficients of time: −0.50 and −0.33, respectively; P=0.004) (Fig. 3A). Similar patterns were observed for other types of cause-specific death, including total CVD (1.82-fold greater, P<0.001) (Fig. 3B) and ischemic stroke (1.78-fold greater, P=0.001) (Fig. 3C). However, the slope associated with the decreasing ischemic heart disease death rate was comparable between the two groups (Fig. 3D).
RESULTS
- In this population-based cohort study, we reported several important findings in terms of mortality rates and trends in individuals with and without diabetes in South Korea. First, between 2003 and 2013, all-cause and CVD mortality rates decreased substantially in subjects with and without diabetes. In addition, the mortality rate decreased more rapidly in subjects with diabetes than in those without diabetes, reducing the gap in mortality rates between the two groups. Finally, the decrease in CVD mortality was primarily attributable to a decrease in mortality from ischemic stroke, rather than from ischemic heart disease, among subjects with diabetes.
- Previous studies have shown that recent all-cause and CVD mortality rates have decreased in patients with diabetes. According to the U.S. National Health Interview Survey, all-cause mortality decreased by 23% and CVD-related mortality decreased by 40% among adults with diabetes between 1997 and 2006 [2]. Similar findings were observed in studies from other developed countries during the same period [67]. These findings were largely attributable to improvements in the treatment of diabetes and its associated conditions, including hypertension and dyslipidemia [18]. The decline in the rate of diabetes-related complications over recent decades [19] also contributed to the improvements in mortality. However, this has not consistently been the case across different populations and different time periods. In a serial National Health and Nutrition Examination Survey study from 1971 to 2000, improvement in the mortality rate of patients with diabetes was limited to men [20]. Furthermore, in a Mexican population, the diabetes-related mortality rate increased from 1980 to 2000 [8]. These findings suggest that evidence of reduced diabetes-related mortality rates is limited to recent studies in developed countries.
- A previous population-based study in South Korea reported disappointing results: from 1983 to 2000, the diabetes-related mortality rate increased substantially (from 5.3 to 18.4 deaths per 100,000 people) [9]. The researchers stated that the reasons for this increase were rapid urbanization, increased intake of foods in high calories, and decreased physical activity. However, using a nationwide cohort data since the 2000s (from 2003 to 2013), we showed the opposite results. Some evidence supports our findings. A serial Korean National Health and Nutrition Examination Survey study of diabetic patients indicated that the treatment rate substantially increased from 1998 to 2005 (from 26.8% to 48.8%) [13]. Recently, the Korean Diabetes Association reported that diabetes care had improved rapidly in South Korea, with medical costs for diabetes being 5.8-fold higher in 2013 than in 2002. In addition, the proportion of patients who adhered to their medication schedule by more than 80% per year increased 2.8-fold (from 24.1% to 67.2%) during the same period [14]. We postulated that progress in the management of diabetes care led to a significant decrease in mortality among people with diabetes in South Korea. Although there were no significant improvements of glycemic control rate over the last decade [2122], we suppose that factors other than glycemic control including wide use of anti-hypertensive drugs or statins may contributed to the improvement of mortality rate in patients with diabetes. In addition, easy medical accessibility which is one of the strength in terms of medical care in Korea might be one main reason of the mortality reduction. Meanwhile, widespread screening by the national checkup programs in Korea has increased early detection and early diagnosis of diabetes. It may have affected the decreased mortality rate in patients with diabetes.
- Several reports in the United States and Canada found a substantial decrease in CVD-related mortality among patients with diabetes [23]. The results of the present study are consistent with those findings. An interesting finding of this study was the substantial decrease in ischemic stroke-related mortality in subjects with diabetes. The ischemic stroke mortality in subjects with diabetes was 2-fold higher than ischemic heart disease mortality in 2003. However, 10 years later, ischemic stroke mortality was even lower than ischemic heart disease mortality. Furthermore, the decreasing slope associated with ischemic stroke mortality was 3.5-fold steeper than that of ischemic heart disease mortality in people with diabetes.
- Improvements in the management of ischemic stroke and its risk factors may have largely contributed to the decline of ischemic stroke mortality. The treatment rate for hypertension has increased by about 2-fold during the last two decades, currently exceeding 65% [1423]. The proportion of patients receiving lipid-lowering medications also increased, being 5-fold greater in 2013 than in 2003 [24]. Moreover, the index for acute management of stroke has improved. In the Korean Stroke Registry study, the percentage of patients who arrived at the hospital within 3 hours of the initiation of stroke symptoms increased from 20% to 29% and the rate of reperfusion therapy increased from 5.3% to 7.0% between 2002 and 2010 [25]. In addition, the number of hospitals with an installed stroke unit has increased substantially [26]. Currently, South Korea has the lowest in-hospital 30-day ischemic stroke-related fatality rate among Organization for Economic Co-operation and Development nations [27]. Consequently, prevalent use of antihypertensive and lipid-lowering agents and improved acute management of stroke in South Korea seem to be major contributors to the marked decrease in ischemic stroke mortality.
- Our study has some limitations. First, we did not distinguish between type 1 diabetes mellitus and type 2 diabetes mellitus because of a lack of exact information to define the types of diabetes. Currently, approximately 5% of people with diabetes are presumed to have type 1 diabetes mellitus in Korea. Although it is a small percentage, it could limit the interpretation of our results. Second, approximately 10% of the total deaths in this cohort were classified as “unknown cause.” We speculated that the majority of those cases were sudden cardiac deaths or deaths related to cardiopulmonary disease. However, we did not include those deaths in the CVD mortality category. Therefore, it is possible that we underestimated the actual number of CVD deaths.
- In summary, overall and CVD mortality rates continuously decreased in subjects with diabetes from 2003 to 2013 in South Korea. The reduction in CVD mortality was primarily attributable to a reduction in ischemic stroke mortality. The gap between the mortality rates of subjects with and without diabetes continuously decreased over time; however, the mortality rate of individuals with diabetes was still more than 2-fold higher than that of individuals without diabetes. Further studies about contributing factors associated with improvement of mortality rate in subjects with diabetes are needed to provide valuable therapeutic information in clinical practice.
DISCUSSION
-
Acknowledgements
- This study was partly supported by a grant from the Korean Health Technology R&D Project (HI14C2750), Ministry of Health and Welfare, Republic of Korea. We thank all of the participants of the Korean Health Insurance Cohort study, as well as the Korean National Health Insurance Service (NHIS), who developed the NHIS National Sample Cohort (2002 to 2010) database (NHIS-2014-2-006). The views expressed in this article are those of the authors and do not necessarily represent the official position of the Korean NHIS.
ACKNOWLEDGMENTS
-
CONFLICTS OF INTEREST: No potential conflict of interest relevant to this article was reported.
NOTES
- 1. Danaei G, Finucane MM, Lu Y, Singh GM, Cowan MJ, Paciorek CJ, Lin JK, Farzadfar F, Khang YH, Stevens GA, Rao M, Ali MK, Riley LM, Robinson CA, Ezzati M. Global Burden of Metabolic Risk Factors of Chronic Diseases Collaborating Group (Blood Glucose). National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2·7 million participants. Lancet 2011;378:31-40. ArticlePubMed
- 2. Gregg EW, Cheng YJ, Saydah S, Cowie C, Garfield S, Geiss L, Barker L. Trends in death rates among U.S. adults with and without diabetes between 1997 and 2006: findings from the National Health Interview Survey. Diabetes Care 2012;35:1252-1257. PubMedPMC
- 3. Lind M, Garcia-Rodriguez LA, Booth GL, Cea-Soriano L, Shah BR, Ekeroth G, Lipscombe LL. Mortality trends in patients with and without diabetes in Ontario, Canada and the UK from 1996 to 2009: a population-based study. Diabetologia 2013;56:2601-2608. ArticlePubMedPDF
- 4. Gu K, Cowie CC, Harris MI. Diabetes and decline in heart disease mortality in US adults. JAMA 1999;281:1291-1297. ArticlePubMed
- 5. Preis SR, Pencina MJ, Hwang SJ, D'Agostino RB Sr, Savage PJ, Levy D, Fox CS. Trends in cardiovascular disease risk factors in individuals with and without diabetes mellitus in the Framingham Heart Study. Circulation 2009;120:212-220. ArticlePubMedPMC
- 6. Harding JL, Shaw JE, Peeters A, Guiver T, Davidson S, Magliano DJ. Mortality trends among people with type 1 and type 2 diabetes in Australia: 1997–2010. Diabetes Care 2014;37:2579-2586. ArticlePubMedPDF
- 7. Lipscombe LL, Hux JE. Trends in diabetes prevalence, incidence, and mortality in Ontario, Canada 1995–2005: a population-based study. Lancet 2007;369:750-756. ArticlePubMed
- 8. Barquera S, Tovar-Guzman V, Campos-Nonato I, Gonzalez-Villalpando C, Rivera-Dommarco J. Geography of diabetes mellitus mortality in Mexico: an epidemiologic transition analysis. Arch Med Res 2003;34:407-414. ArticlePubMed
- 9. Choi YJ, Cho YM, Park CK, Jang HC, Park KS, Kim SY, Lee HK. Rapidly increasing diabetes-related mortality with socioenvironmental changes in South Korea during the last two decades. Diabetes Res Clin Pract 2006;74:295-300. ArticlePubMed
- 10. Yang W, Lu J, Weng J, Jia W, Ji L, Xiao J, Shan Z, Liu J, Tian H, Ji Q, Zhu D, Ge J, Lin L, Chen L, Guo X, Zhao Z, Li Q, Zhou Z, Shan G, He J. China National Diabetes and Metabolic Disorders Study Group. Prevalence of diabetes among men and women in China. N Engl J Med 2010;362:1090-1101. ArticlePubMed
- 11. World Health Organization. Global health estimates: deaths by cause, age, sex and country, 2000–2012. Geneva: World Health Organization; 2014.
- 12. Song SO, Lee YH, Kim DW, Song YD, Nam JY, Park KH, Kim DJ, Park SW, Lee HC, Lee BW. Trends in diabetes incidence in the last decade based on Korean National Health Insurance claims data. Endocrinol Metab (Seoul) 2016;31:292-299. ArticlePubMedPMCPDF
- 13. Choi YJ, Kim HC, Kim HM, Park SW, Kim J, Kim DJ. Prevalence and management of diabetes in Korean adults: Korea National Health and Nutrition Examination Surveys 1998–2005. Diabetes Care 2009;32:2016-2020. PubMedPMC
- 14. Korea Diabetes Association. Diabetes fact sheet in Korea 2013 cited 2018 Mar 30. Available from: http://www.diabetes.or.kr/temp/diabetes_factsheet_2013111.pdf.
- 15. Kim NH, Lee J, Kim TJ, Kim NH, Choi KM, Baik SH, Choi DS, Pop-Busui R, Park Y, Kim SG. Body mass index and mortality in the general population and in subjects with chronic disease in Korea: a nationwide cohort study (2002–2010). PLoS One 2015;10:e0139924. ArticlePubMedPMC
- 16. Indrayan A. Medical Biostatistics. 3rd ed. Boca Raton: CRC Press; 2012.
- 17. Altman D, Machin D, Bryant T, Gardner M. Statistics with confidence: confidence intervals and statistical guidelines. Hoboken: John Wiley & Sons; 2013.
- 18. Gregg EW, Albright AL. The public health response to diabetes: two steps forward, one step back. JAMA 2009;301:1596-1598. ArticlePubMed
- 19. Gregg EW, Li Y, Wang J, Burrows NR, Ali MK, Rolka D, Williams DE, Geiss L. Changes in diabetes-related complications in the United States, 1990–2010. N Engl J Med 2014;370:1514-1523. ArticlePubMed
- 20. Gregg EW, Gu Q, Cheng YJ, Narayan KM, Cowie CC. Mortality trends in men and women with diabetes, 1971 to 2000. Ann Intern Med 2007;147:149-155. ArticlePubMed
- 21. Jeon JY, Kim DJ, Ko SH, Kwon HS, Lim S, Choi SH, Kim CS, An JH, Kim NH, Won JC, Kim JH, Cha BY, Song KH. Taskforce Team of Diabetes Fact Sheet of the Korean Diabetes Association. Current status of glycemic control of patients with diabetes in Korea: the Fifth Korea National Health and Nutrition Examination Survey. Diabetes Metab J 2014;38:197-203. ArticlePubMedPMC
- 22. Ha KH, Kim DJ. Current status of managing diabetes mellitus in Korea. Korean J Intern Med 2016;31:845-850. ArticlePubMedPMCPDF
- 23. Shin J, Park JB, Kim KI, Kim JH, Yang DH, Pyun WB, Kim YG, Kim GH, Chae SC. Guideline Committee of the Korean Society of Hypertension. 2013 Korean Society of Hypertension guidelines for the management of hypertension: part III-hypertension in special situations. Clin Hypertens 2015;21:3ArticlePubMedPMCPDF
- 24. Ha KH, Kwon HS, Kim DJ. Epidemiologic characteristics of dyslipidemia in Korea. J Lipid Atheroscler 2015;4:93-99.Article
- 25. Jung KH, Lee SH, Kim BJ, Yu KH, Hong KS, Lee BC, Roh JK. Korean Stroke Registry Study Group. Secular trends in ischemic stroke characteristics in a rapidly developed country: results from the Korean Stroke Registry Study (secular trends in Korean stroke). Circ Cardiovasc Qual Outcomes 2012;5:327-334. PubMed
- 26. Hong KS, Bang OY, Kim JS, Heo JH, Yu KH, Bae HJ, Kang DW, Lee JS, Kwon SU, Oh CW, Lee BC, Yoon BW. Stroke statistics in Korea: part II. Stroke awareness and acute stroke care, a report from the Korean Stroke Society and clinical research center for stroke. J Stroke 2013;15:67-77. ArticlePubMedPMC
- 27. Hong KS, Bang OY, Kang DW, Yu KH, Bae HJ, Lee JS, Heo JH, Kwon SU, Oh CW, Lee BC, Kim JS, Yoon BW. Stroke statistics in Korea: part I. Epidemiology and risk factors: a report from the Korean Stroke Society and clinical research center for stroke. J Stroke 2013;15:2-20. ArticlePubMedPMC
REFERENCES
Annual trends of the standardized all-cause mortality rates for subjects with diabetes (black bar) and without diabetes (white bar) from 2003 to 2013. DM, diabetes mellitus.
Annual trends in the standardized mortality rates from cardiovascular disease (CVD), ischemic stroke, and ischemic heart disease for subjects with diabetes (A) and without diabetes (B).
Trends in mortality rates and annualized slopes for mortality from (A) any cause, (B) all cardiovascular diseases, (C) ischemic stroke, and (D) ischemic heart disease for subjects with and without diabetes. DM, diabetes mellitus.

Causes and annual number of deaths in subjects with and without diabetes from 2003 to 2013
Figure & Data
References
Citations

- Green tea consumption and incidence of cardiovascular disease in type 2 diabetic patients with overweight/obesity: a community-based cohort study
Bingyue Liu, Shujun Gu, Jin Zhang, Hui Zhou, Jian Su, Sudan Wang, Qian Sun, Zhengyuan Zhou, Jinyi Zhou, Chen Dong
Archives of Public Health.2024;[Epub] CrossRef - Trends in all-cause and cause-specific mortality in older adults with and without diabetes: A territory-wide analysis in one million older adults in Hong Kong
Aimin Yang, Tingting Chen, Mai Shi, Eric Lau, Raymond SM Wong, Jones Chan, Juliana CN Chan, Elaine Chow
Diabetes Research and Clinical Practice.2024; 210: 111618. CrossRef - Lipid Management in Korean People With Type 2 Diabetes Mellitus: Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis Consensus Statement
Ye Seul Yang, Hack-Lyoung Kim, Sang-Hyun Kim, Min Kyong Moon
Journal of Lipid and Atherosclerosis.2023; 12(1): 12. CrossRef - Lipid Management in Korean People with Type 2 Diabetes Mellitus: Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis Consensus Statement
Ye Seul Yang, Hack-Lyoung Kim, Sang-Hyun Kim, Min Kyong Moon
Diabetes & Metabolism Journal.2023; 47(1): 1. CrossRef - Letter: Triglyceride-Glucose Index Predicts Cardiovascular Outcome in Metabolically Unhealthy Obese Population: A Nationwide Population-Based Cohort Study (J Obes Metab Syndr 2022;31:178-86)
Gwanpyo Koh
Journal of Obesity & Metabolic Syndrome.2023; 32(2): 179. CrossRef - Management of Dyslipidemia in Patients with Diabetes Mellitus
Kyung Ae Lee
The Journal of Korean Diabetes.2023; 24(3): 111. CrossRef - 2023 Clinical Practice Guidelines for Diabetes: Management of Cardiovascular Risk Factors
Ye Seul Yang
The Journal of Korean Diabetes.2023; 24(3): 135. CrossRef - The Characteristics and Risk of Mortality in the Elderly Korean Population
Sunghwan Suh
Endocrinology and Metabolism.2023; 38(5): 522. CrossRef - Current Status of Low-Density Lipoprotein Cholesterol Target Achievement in Patients with Type 2 Diabetes Mellitus in Korea Compared with Recent Guidelines
Soo Jin Yun, In-Kyung Jeong, Jin-Hye Cha, Juneyoung Lee, Ho Chan Cho, Sung Hee Choi, SungWan Chun, Hyun Jeong Jeon, Ho-Cheol Kang, Sang Soo Kim, Seung-Hyun Ko, Gwanpyo Koh, Su Kyoung Kwon, Jae Hyuk Lee, Min Kyong Moon, Junghyun Noh, Cheol-Young Park, Sung
Diabetes & Metabolism Journal.2022; 46(3): 464. CrossRef - Health-related Quality of Life Instrument With 8 Items for Use in Patients With Type 2 Diabetes Mellitus: A Validation Study in Korea
Juyoung Kim, Hyeon-Jeong Lee, Min-Woo Jo
Journal of Preventive Medicine and Public Health.2022; 55(3): 234. CrossRef - Improvement in Age at Mortality and Changes in Causes of Death in the Population with Diabetes: An Analysis of Data from the Korean National Health Insurance and Statistical Information Service, 2006 to 2018
Eugene Han, Sun Ok Song, Hye Soon Kim, Kang Ju Son, Sun Ha Jee, Bong-Soo Cha, Byung-Wan Lee
Endocrinology and Metabolism.2022; 37(3): 466. CrossRef - Renoprotective Mechanism of Sodium-Glucose Cotransporter 2 Inhibitors: Focusing on Renal Hemodynamics
Nam Hoon Kim, Nan Hee Kim
Diabetes & Metabolism Journal.2022; 46(4): 543. CrossRef - Diabetic Ketoacidosis and COVID-19: A Retrospective Observational Study
Govind Nagdev, Gajanan Chavan, Charuta Gadkari, Gaurav Sahu
Cureus.2022;[Epub] CrossRef - Trends in the effects of pre‐transplant diabetes on mortality and cardiovascular events after kidney transplantation
Ja Young Jeon, Soo Jung Kim, Kyoung Hwa Ha, Ji Hyun Park, Bumhee Park, Chang‐Kwon Oh, Seung Jin Han
Journal of Diabetes Investigation.2021; 12(5): 811. CrossRef - Acute Hyperglycemic Crises with Coronavirus Disease-19: Case Reports
Na-young Kim, Eunyeong Ha, Jun Sung Moon, Yong-Hoon Lee, Eun Young Choi
Diabetes & Metabolism Journal.2020; 44(2): 349. CrossRef - Polysomnographic phenotyping of obstructive sleep apnea and its implications in mortality in Korea
Jeong-Whun Kim, Tae-Bin Won, Chae-Seo Rhee, Young Mi Park, In-Young Yoon, Sung-Woo Cho
Scientific Reports.2020;[Epub] CrossRef - Peripheral arterial endothelial dysfunction predicts future cardiovascular events in diabetic patients with albuminuria: a prospective cohort study
Bo Kyung Koo, Woo-Young Chung, Min Kyong Moon
Cardiovascular Diabetology.2020;[Epub] CrossRef - Metformin treatment for patients with diabetes and chronic kidney disease: A Korean Diabetes Association and Korean Society of Nephrology consensus statement
Kyu Yeon Hur, Mee Kyoung Kim, Seung Hyun Ko, Miyeun Han, Dong Won Lee, Hyuk-Sang Kwon
Kidney Research and Clinical Practice.2020; 39(1): 32. CrossRef - Outcomes for Inappropriate Renal Dose Adjustment of Dipeptidyl Peptidase-4 Inhibitors in Patients With Type 2 Diabetes Mellitus: Population-Based Study
Sangmo Hong, Kyungdo Han, Cheol-Young Park
Mayo Clinic Proceedings.2020; 95(1): 101. CrossRef - Metformin Treatment for Patients with Diabetes and Chronic Kidney Disease: A Korean Diabetes Association and Korean Society of Nephrology Consensus Statement
Kyu Yeon Hur, Mee Kyoung Kim, Seung Hyun Ko, Miyeun Han, Dong Won Lee, Hyuk-Sang Kwon
Diabetes & Metabolism Journal.2020; 44(1): 3. CrossRef - A systematic review of trends in all-cause mortality among people with diabetes
Lei Chen, Rakibul M. Islam, Joanna Wang, Thomas R. Hird, Meda E. Pavkov, Edward W. Gregg, Agus Salim, Maryam Tabesh, Digsu N. Koye, Jessica L. Harding, Julian W. Sacre, Elizabeth L. M. Barr, Dianna J. Magliano, Jonathan E. Shaw
Diabetologia.2020; 63(9): 1718. CrossRef - Diabetic ketoacidosis precipitated by COVID-19: A report of two cases and review of literature
Pavan Kumar Reddy, Mohammad Shafi Kuchay, Yatin Mehta, Sunil Kumar Mishra
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2020; 14(5): 1459. CrossRef - Prognostic value of long-term gamma-glutamyl transferase variability in individuals with diabetes: a nationwide population-based study
Da Young Lee, Kyungdo Han, Ji Hee Yu, Sanghyun Park, Ji A Seo, Nam Hoon Kim, Hye Jin Yoo, Sin Gon Kim, Seon Mee Kim, Kyung Mook Choi, Sei Hyun Baik, Yong Gyu Park, Nan Hee Kim
Scientific Reports.2020;[Epub] CrossRef - Arterial stiffness is an independent predictor for risk of mortality in patients with type 2 diabetes mellitus: the REBOUND study
Jeong Mi Kim, Sang Soo Kim, In Joo Kim, Jong Ho Kim, Bo Hyun Kim, Mi Kyung Kim, Soon Hee Lee, Chang Won Lee, Min Chul Kim, Jun Hyeob Ahn, Jinmi Kim
Cardiovascular Diabetology.2020;[Epub] CrossRef - The triglyceride glucose index is a simple and low-cost marker associated with atherosclerotic cardiovascular disease: a population-based study
Sangmo Hong, Kyungdo Han, Cheol-Young Park
BMC Medicine.2020;[Epub] CrossRef - Increased Age of Death and Change in Causes of Death Among Persons With Diabetes Mellitus From the Korean National Health Insurance and Statistical Information Service, 2006 to 2018
Eugene Han, Sun Ok Song, Hye Soon Kim, Kang Ju Son, Sun Ha Jee, Bong-Soo Cha, Byung-Wan Lee
SSRN Electronic Journal .2020;[Epub] CrossRef - Letter: Comparison of the Efficacy of Rosuvastatin Monotherapy 20 mg with Rosuvastatin 5 mg and Ezetimibe 10 mg Combination Therapy on Lipid Parameters in Patients with Type 2 Diabetes Mellitus (Diabetes Metab J2019;43:582–9)
Tae Seo Sohn
Diabetes & Metabolism Journal.2019; 43(6): 909. CrossRef - Diabetes Mellitus, Still Major Threat to Mortality from Various Causes
Nam Hoon Kim
Diabetes & Metabolism Journal.2019; 43(3): 273. CrossRef - Diabetes and Cancer: Cancer Should Be Screened in Routine Diabetes Assessment
Sunghwan Suh, Kwang-Won Kim
Diabetes & Metabolism Journal.2019; 43(6): 733. CrossRef - Trends of Diabetes Epidemic in Korea
Ji Cheol Bae
Diabetes & Metabolism Journal.2018; 42(5): 377. CrossRef

 KDA
KDA PubReader
PubReader Cite
Cite