
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 37(2); 2013 > Article
-
Brief ReportClinical Care/Education Is the Indicator Magnifying Window for Insulin Pens Helpful for Elderly Diabetic Patients?
- Ju Hee Lee1, Eun Shil Hong2, Jung Hun Ohn2, Young Min Cho2
-
Diabetes & Metabolism Journal 2013;37(2):149-151.
DOI: https://doi.org/10.4093/dmj.2013.37.2.149
Published online: April 16, 2013
- 3,164 Views
- 30 Download
1Department of Internal Medicine, Chungnam National University School of Medicine, Daejeon, Korea.
2Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Korea.
- Corresponding author: Young Min Cho. Department of Internal Medicine, Seoul National University College of Medicine, 101 Daehak-ro, Jongno-gu, Seoul 110-744, Korea. ymchomd@snu.ac.kr
• Received: November 15, 2012 • Accepted: January 2, 2013
Copyright © 2013 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Patients with type 2 diabetes who require insulin therapy are commonly elderly and have poor visual acuity. In this study, we examined the clinical usefulness of the indicator magnifying window (IMW) for elderly patients with type 2 diabetes. We recruited 50 patients with type 2 diabetes over the age of 60 who had used insulin pens for glucose control. They were asked to set the insulin pen at randomly selected doses with or without an IMW. We assessed dosing accuracy, convenience, self-confidence, need for eyeglasses, preference, and willingness to recommend the IMW to other patients. Although the IMW did not improve the dosing accuracy or convenience, it significantly decreased the need for eyeglasses. Overall, the clinical usefulness of the IMW is quite limited in elderly patients with type 2 diabetes.
- The number of elderly patients with type 2 diabetes is continuously increasing and many of them suffer from poor vision due to senile changes or diabetic eye complications [1-4]. Since type 2 diabetes is characterized by a progressive decline in insulin secretory function, many patients eventually require insulin therapy [5-7], which is a common problem in elderly patients with type 2 diabetes. Furthermore, in elderly patients with type 2 diabetes, visual impairment may predispose inaccurate insulin dosing, which may result in erroneous glycemic control, including hyper or hypoglycemia. In this study, we examined whether the indicator magnifying window (IMW) for insulin pens assists in effective insulin therapy for elderly patients with type 2 diabetes.
INTRODUCTION
- Subjects and data collection
- Fifty patients (30 men and 20 women) with type 2 diabetes were prospectively enrolled at the Seoul National University Hospital. The inclusion criteria required that subjects have type 2 diabetes, be over 60 years old, and self-inject insulin with insulin pens. The exclusion criteria included subjects who had corrected visual acuity of ≤20/200. The Institutional Review Board at Seoul National University Hospital approved the study protocol. This study is registered at ClinicalTrials. gov (NCT01563419). Written informed consent was obtained from all subjects prior to any study-related procedures. Medical history was obtained by reviewing medical records and/or questionnaires. We measured near visions of the enrolled patients using the Korean Near Vision Chart [8].
- Assessment of efficacy of the indicator magnifying window
- We asked the subjects to dial up the insulin pen (Lantus Solo-Star Pen; Sanofi, Frankfurt, Germany) to a randomly selected dose between 30 and 40 units. We checked whether they dialed the selected dose correctly and measured the time spent to complete the task. For each subject, we repeated the test three times with insulin pens with or without the IMW (Izumi Planning Co., Tokyo, Japan) (Fig. 1) in a random order. If the subject dialed the selected dose correctly at all three trials, we concluded that the subject had set the dose correctly.
- After completing the test, we asked the subjects to assess the convenience of dosing when using the IMW by checking a convenience score from 1 point (very inconvenient) to 5 points (very convenient) on the questionnaire. We also asked about their self-confidence in setting the designated doses, need for glasses in setting up the doses, preference for the use of the IMW, and willingness to recommend the IMW to other patients.
- Statistical analysis
- A sample size of 49 patients was calculated to provide 90% power (α=0.05) to simultaneously detect a 2-second difference in the time spent to complete the task with the IMW, considering a 10% screening failure. All continuous variables are expressed as mean±standard deviation. The t-test was used to compare the time spent to complete the task and the convenience score. The chi-square test was used to analyze the dosing accuracy, self-confidence in setting the designated doses, and need for glasses in setting up the insulin doses. A P value of less than 0.05 was considered statistically significant. All the analyses were performed using IBM SPSS version 18.0 for Windows (IBM, Armonk, NY, USA).
METHODS
- We recruited 50 patients with type 2 diabetes (30 men and 20 women). The mean age was 69±6 years, duration of diabetes was 17±8 years, and duration of insulin treatment was 5±5 years. The mean hemoglobin A1c was 8.2%±1.4% and the average near visual acuity of patients was 20/60 for each eye. Thirtytwo patients (64%) were diagnosed with diabetic retinopathy.
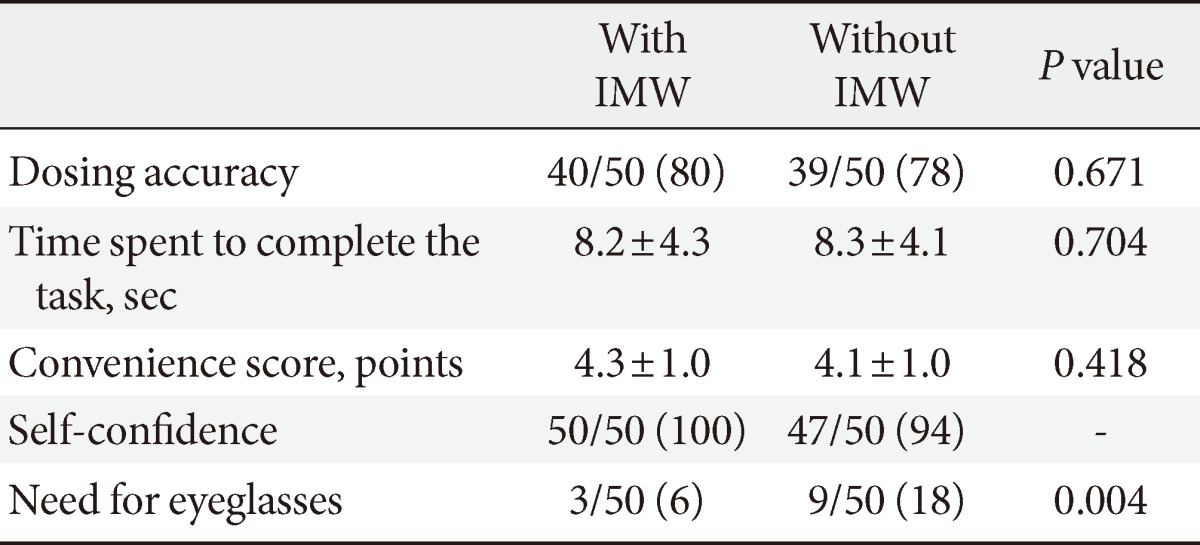
- The results of the efficacy studies for the IMW are shown in Table 1. Forty patients (80%) and 39 patients (78%) dialed the designated dose correctly with and without the IMW, respectively (P=0.671). Time spent to complete the task was 8.2±4.3 seconds with the IMW and 8.3±4.1 seconds without the IMW (P=0.704). The convenience score with or without the IMW was similar (4.3±1.0 points vs. 4.1±1.0 points; P=0.418).
- All patients expressed self-confidence in setting the correct dose with the IMW and 47 patients (94%) expressed self-confidence without the IMW. Three patients (6%) needed eyeglasses for near vision to set the designated insulin doses with the IMW, while nine patients (18%) needed eyeglasses without the IMW, which was statistically significantly different (P=0.004). Seventeen patients (34%) reported that they would like to continue to use the device and 24 patients (48%) reported that they were willing to recommend it to other patients.
RESULTS
- Various diabetes-care devices have been developed for patients with impaired vision, such as a talking blood glucose monitor, magnifiers for insulin syringes and pumps, and syringe-filling devices for the blind or partially sighted people with diabetes [9,10]. However, the efficacy of these devices for diabetic patients had not been proven, except in the case of prefilled insulin pen devices. The insulin pen has been shown to exhibit distinct advantages over the syringe and vial in terms of accuracy and ease of use [11-16].
- In this study, we examined the clinical usefulness of the IMW for insulin pens in elderly patients with type 2 diabetes. Since syringe or insulin pen magnifiers enlarge the scale of insulin syringes or pens, it was expected that they would be useful particularly for elderly diabetic patients. However, the IMW did not improve the dosing accuracy or convenience score with regard to the use of insulin pens, which could be explained by the fact that all the patients had previously used insulin pens and felt comfortable with insulin pens. Nonetheless, the IMW significantly decreased the need for eyeglasses while setting up the insulin doses. Overall, the IMW may decrease the need for eyeglasses for insulin dosing with insulin pens, although other clinical benefits of the IMW appear to be limited.
DISCUSSION
- 1. Zhang X, Gregg EW, Cheng YJ, Thompson TJ, Geiss LS, Duenas MR, Saaddine JB. Diabetes mellitus and visual impairment: national health and nutrition examination survey, 1999-2004. Arch Ophthalmol 2008;126:1421-1427. ArticlePubMed
- 2. de Fine Olivarius N, Siersma V, Almind GJ, Nielsen NV. Prevalence and progression of visual impairment in patients newly diagnosed with clinical type 2 diabetes: a 6-year follow up study. BMC Public Health 2011;11:80ArticlePubMedPMCPDF
- 3. Ministry for Health, Welfare and Family Affairs: The Third Korea National Health and Nutrition Examination Survey (KNHANES III) Available from: http://knhanes.cdc.go.kr (updated 2006 Jul 8).
- 4. Lim S, Kim DJ, Jeong IK, Son HS, Chung CH, Koh G, Lee DH, Won KC, Park JH, Park TS, Ahn J, Kim J, Park KG, Ko SH, Ahn YB, Lee I. A nationwide survey about the current status of glycemic control and complications in diabetic patients in 2006: the Committee of the Korean Diabetes Association on the epidemiology of diabetes mellitus. Korean Diabetes J 2009;33:48-57.Article
- 5. Porte D Jr, Kahn SE. Beta-cell dysfunction and failure in type 2 diabetes: potential mechanisms. Diabetes 2001;50(Suppl 1):S160-S163. ArticlePubMedPDF
- 6. Stumvoll M, Goldstein BJ, van Haeften TW. Type 2 diabetes: principles of pathogenesis and therapy. Lancet 2005;365:1333-1346. ArticlePubMed
- 7. Inzucchi SE, Bergenstal RM, Buse JB, Diamant M, Ferrannini E, Nauck M, Peters AL, Tsapas A, Wender R, Matthews DR. American Diabetes Association (ADA). European Association for the Study of Diabetes (EASD). Management of hyperglycemia in type 2 diabetes: a patient-centered approach: position statement of the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care 2012;35:1364-1379. ArticlePubMedPMCPDF
- 8. Hahn CS. The Korean near vision chart. J Korean Ophthalmol Soc 1964;5:7-10.
- 9. Bartos BJ, Cleary ME, Kleinbeck C, Petzinger RA, Sokol-McKay DA, Whittington A, Williams AS. Diabetes and disabilities: assistive tools, services, and information. Diabetes Educ 2008;34:597-605. ArticlePubMedPDF
- 10. Petzinger RA. Diabetes aids and products for people with visual or physical impairment. Diabetes Educ 1992;18:121-138. ArticlePubMedPDF
- 11. Graff MR, McClanahan MA. Assessment by patients with diabetes mellitus of two insulin pen delivery systems versus a vial and syringe. Clin Ther 1998;20:486-496. ArticlePubMed
- 12. Gnanalingham MG, Newland P, Smith CP. Accuracy and reproducibility of low dose insulin administration using pen-injectors and syringes. Arch Dis Child 1998;79:59-62. ArticlePubMedPMC
- 13. Korytkowski M, Bell D, Jacobsen C, Suwannasari R. FlexPen Study Team. A multicenter, randomized, open-label, comparative, two-period crossover trial of preference, efficacy, and safety profiles of a prefilled, disposable pen and conventional vial/syringe for insulin injection in patients with type 1 or 2 diabetes mellitus. Clin Ther 2003;25:2836-2848. ArticlePubMed
- 14. Ignaut DA, Schwartz SL, Sarwat S, Murphy HL. Comparative device assessments: Humalog KwikPen compared with vial and syringe and FlexPen. Diabetes Educ 2009;35:789-798. ArticlePubMedPDF
- 15. Rubin RR, Peyrot M. Quality of life, treatment satisfaction, and treatment preference associated with use of a pen device delivering a premixed 70/30 insulin aspart suspension (aspart protamine suspension/soluble aspart) versus alternative treatment strategies. Diabetes Care 2004;27:2495-2497. ArticlePubMedPDF
- 16. Williams AS, Schnarrenberger PA. A comparison of dosing accuracy: visually impaired and sighted people using insulin pens. J Diabetes Sci Technol 2010;4:514-521. ArticlePubMedPMCPDF
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 


 KDA
KDA
 PubReader
PubReader Cite
Cite




