
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 35(2); 2011 > Article
-
ReviewThe Prediabetic Period: Review of Clinical Aspects
- Sang Youl Rhee, Jeong-Taek Woo
-
Diabetes & Metabolism Journal 2011;35(2):107-116.
DOI: https://doi.org/10.4093/dmj.2011.35.2.107
Published online: April 30, 2011
Department of Endocrinology and Metabolism, Kyung Hee University School of Medicine; Research Institute of Endocrinology, Kyung Hee University, Seoul, Korea.
- Corresponding author: Jeong-Taek Woo. Department of Endocrinology and Metabolism, Kyung Hee University School of Medicine, 1 Hoegi-dong, Dongdaemun-gu, Seoul 130-702, Korea. jtwoomd@khmc.or.kr
Copyright © 2011 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Hyperglycemia that does not satisfy the diagnostic criteria for diabetes mellitus (DM) is generally called prediabetes (preDM). The global prevalence of preDM has been increasing progressively in the past few decades, and it has been established that preDM status is a strong risk factor for DM and cardiovascular disease. Currently, preDM status is classified into two subtypes: impaired fasting glucose and impaired glucose tolerance. Currently, preDM is not regarded as an independent clinical entity, but only as a risk factor for others. In this article, we review various clinical aspects of preDM in terms of the working definition, changes in criteria over the years, epidemiology, and pathophysiological characteristics, and its clinical significance in current medicine.
- Non-diabetic hyperglycemia that does not satisfy the diagnostic criteria for diabetes mellitus (DM) is generally known as prediabetes (preDM). It is generally agreed that all forms of diabetes pass through this prediabetic state before escalating into full-blown diabetes [1]. Similar to DM, fasting plasma glucose (FPG) and oral glucose tolerance tests are both used independently as defining criteria for preDM [1,2]. Recently, hemoglobin A1c (HbA1c) has also been used in the diagnosis of preDM [1,3].
- Because it is well-established that the risks of type 2 DM (T2DM) and cardiovascular disease are significantly increased in preDM subjects, life style modifications have been recommended for this population as a method to control preDM [2,4]. The benefits of this have been confirmed in many prospective, randomized studies where life style modification and pharmacological intervention have been shown to significantly improve clinical markers related to the risk of T2DM and cardiovascular disease [5-7]. However, current preDM medical guidelines treat this condition as a risk factor for diabetes and cardiovascular disease, rather than a separate clinical entity. Additionally, the clinical significance of preDM has not been clearly established [1,2,4]. Studies suggest that preDM has specific clinical significance separate from type 2 diabetes. Because of this, it is thought that more active discussions are needed on the topic. Here, we review various clinical aspects of preDM with respect to the working definition, changes in criteria over time, epidemiology, pathophysiological characteristics, and its clinical significance in current medicine.
INTRODUCTION
- According to the most recent clinical practice recommendations published in 2010 by the American Diabetes Association (ADA), preDM is defined as 1) impaired fasting glucose (IFG) with fasting plasma glucose levels of 100 to 125 mg/dL (5.6 to 6.9 mmol/L), 2) impaired glucose tolerance (IGT) with plasma glucose levels of 140 to 199 mg/dL (7.8 to 11.0 mmol/L) 2-hour postprandial, or 3) an HbA1c of 5.7 to 6.4% [1]. These criteria have evolved over the years and discussions on the topic continue.
- Changes in preDM diagnostic criteria
- In the 1979 American National Diabetes Data Group (NDDG) report, the first consensus-based, systematic criteria for DM were proposed. Specifically, non-diabetic hyperglycemia was defined as being in the high-risk group for the progression of DM and the presence of IGT [8]. The diagnostic criteria for IGT required satisfaction of the following three conditions: 1) FPG <140 mg/dL (7.8 mmol/L), 2) FPG ≥200 mg/dL (11.1 mmol/L) 0.5, 1, and 1.5 hours after a 75-g oral glucose tolerance test, 3) and FPG between 140 and 200 mg/dL (7.8 to 11.1 mmol/L) 2 hours after a 75-g oral glucose tolerance test [8]. However, the diagnostic criteria for IGT based on the NDDG reports are somewhat restricting, and there were difficulties including some subjects during the screening period [9].
- The diagnostic criteria for IGT that were published by the World Health Organization (WHO) in 1980 were simpler than the NDDG classification criteria. IGT was defined by a 2-hour plasma glucose level of 140 to 200 mg/dL (8.0 to 11.0 mmol/L) after a 75-g oral glucose tolerance test [10]. However, WHO criteria excluded the fasting criteria in the IGT diagnosis and only emphasized post-challenge glucose. This is because confirmation of fasting during screening is not easily obtained [10].
- Eighteen years after the NDDG report, ADA proposed new diagnosis criteria for DM in 1997 [11]. When considering the cost, time, and reproducibility of oral glucose tolerance tests, it was recommended that diabetes screening and diagnostic tests primarily use the FPG test. Based on macrovascular complication risks, the threshold for the diagnostic criterion changed from 140 to 126 mg/dL [11]. Thus, according to these criteria, a fasting glucose of 110 to 126 mg/dL in preDM (6.1 to 7.0 mmol/L) is classified as IFG, while a 2-hour post-challenge plasma glucose concentration between 140 and 200 mg/dL (7.8 to 11.1 mmol/L) is now classified as IGT. The WHO diagnostic criteria that were released in 1999 were very similar to the ADA diagnostic criteria [12,13].
- To prevent similarity between IGT and IFG, in the ADA Expert Committee report, the IFG criteria was changed from 110 mg/dL (6.1 mmol/L) to 100 mg/dL in 2003 (5.6 mmol/L) [14,15]. Recently, the International Expert Committee recommended that HbA1c be added to the diagnosis of DM; the 2010 ADA clinical practice recommendation defining HbA1c levels of over 6.5% as DM, and an HbA1c between 5.7 and 6.4% as preDM [1,3].
- Major issues in diagnostic criteria changes for preDM
- The diagnostic criteria for diabetes and preDM have been changed several times, and the use of A1c and others tests as diagnostic criteria for DM have been actively discussed. However, there does not appear to be a complete consensus regarding this matter.
- To determine the cut-off values for preDM, criteria that sharply delineate increases in the risk of adverse clinical or metabolic outcomes based on changes in blood glucose are needed. These questions are important for both IFG and IGT. However, unlike the widely accepted IGT criteria, controversy remains regarding diagnostic criteria for IFG.
- In 2003, the ADA recommended that the criterion for IFG be lowered from 110 mg/dL (6.1 mmol/L) to 100 mg/dL (5.6 mmol/L) [14]. This change was based on receiver operating characteristic (ROC) analysis results for fasting blood glucose levels. Specifically, these criteria were able to maximize sensitivity and specificity in detecting DM over a period of 5 years from Pima Indian, Mauritius, San Antonio, and Hoorn Study data [14,16-18]. The cut-off value for maximum sensitivity and specificity for detecting DM was set at 97 to 99 mg/dL (5.4 to 5.5 mmol/L) [14]. Additionally, by lowering the IFG cut-off value, IFG prevalence became similar to IGT prevalence, and the percentages of people who were screened for FPG and postprandial blood glucose were similarly matched [14].
- However, the WHO advised that the cut-off value for IFG should be maintained at 110 mg/dL, because IFG prevalence would be increased significantly by changing the cut-off criterion. Although this could have important personal or social impacts, there is not a major reduction in adverse outcomes or the prevention of DM progression as a result of this change [19].
- The actual risk of developing DM is known to be associated with an increase in FPG concentrations from "normal" conditions. In studies conducted in young men, the risk of developing diabetes gradually increased when fasting blood glucose levels rose from under 81 mg/dL (4.5 mmol/L) to over 86 mg/dL (4.8 mmol/L) [20]. This result suggests that there is no exact cut-off value for FPG levels that predicts adverse outcomes. Additionally, in the Atherosclerosis Risk in Communities (ARIC) study, when FPG levels were over 106 mg/dL (5.9 mmol/L), it was predicted with 50% sensitivity that subjects would develop diabetes, whereas when FPG was over 100 mg/dL (5.6 mmol/L), it was predicted with 70% sensitivity; thus, higher-risk groups could be screened for. However, the percentage of the population that can be screened as a high-risk group increases by more than double the normal value with this kind of increase in sensitivity [21]. Additionally, when the ADA diagnostic criterion cut-off value was lowered, new IFG patients had more favorable cardiovascular risk profiles and a lower risk of developing diabetes compared with patients who were selected by the WHO criteria [22-25]. For these reasons, many diabetes experts did not completely agree with the ADA's IFG diagnostic criteria [19,22,26].
- A1c had been widely used as a test to estimate the degree of glycemic control. Because it can be measured regardless of food intake, A1c is simpler than FPG or oral glucose tolerance tests. Additionally, because it reflects long-term glucose concentrations, versus frequently changing glucose levels, it is more closely related to the chronic complications of diabetes [27-29]. Because the current DM diagnostic criteria are based on an increased risk of developing DM-related chronic complications, using A1c for the diagnosis of DM is a rational approach. However, the cost of A1c compared with simple glucose tests is high. Additionally, because measurement standards have not been established, its use as a diagnostic criterion for diabetes has been limited. Measurement methods are continuously improving, and according to the efforts of professionals from the American National Glycohemoglobin Standardization Program, European International Federation of Clinical Chemistry, Japanese Diabetes Society/Japanese Society of Clinical Chemistry, and other organizations for measurement standardization, A1c is now actively being considered as a diagnostic criterion for diabetes [27,30,31].
- In several studies that have examined the diagnostic value of A1c, compared with FPG, A1c has been shown to have lower variability and higher specificity [32]. Based on several population-based studies, the A1c cut-off value has been set at 5.9 to 6.2% for estimated diabetes diagnoses [33-36]. Specifically, in the National Health and Nutrition Examination Survey (NHANES) III, where the mean value of the A1c cut-off was set at over 6.5%, diabetes diagnoses had a 99.6% specificity and a 43 to 44% sensitivity [37]. Based on the results of these studies, the International Expert Committee proposed that the new standard A1c value for the diagnosis of DM be changed to above 6.5%. Since this time, the ADA has adopted it as a new official diagnostic criterion [1,3].
- For preDM, the International Expert Committee also decided that A1c values between 6 and 6.5% are considered to be in the high-risk category for diabetes [3]. In an actual population-based study, participants who had A1c levels between 6 and 6.5% had a 10-fold increase in the occurrence of diabetes compared with participants with A1c levels below 6% [38,39]. However, over 5 years, participants with A1c levels of 5.5 to 6.0% had cumulative occurrence percentages between 12 and 25%, which was 3 to 8 times higher than the control group. Based on data from NHANES study subjects, the closest A1c level for current IFG and IGT criteria was 5.5 to 6.0%; however, in the linear regression analysis, a fasting glucose level of 100 mg/dL corresponded with an A1c of 5.4%, and a fasting glucose level of 110 mg/dL corresponded with an A1c of 5.6% [1]. When the A1c cut-off value for preDM was set at 5.7%, sensitivity was 39 to 45% and specificity was 81 to 91% for IFG and IGT predictions [1]. Based on large-scale prospective studies, when the preDM cut-off value was set at 5.7%, the sensitivity was 66% and specificity was 88% for predicting the risk of DM risk over the next 6 years [36]. Consistent with these results, an HbA1c of 5.7 to 6.4% was presented by the ADA as a preDM criterion [1].
- However, based on the current criteria, diagnosis of subjects screened using the A1c 5.7 to 6.4% criterion are not completely consistent with IFG and IGT methods. With respect to the fasting blood glucose cut-off values proposed by the ADA, it is expected that that it will take some time until the aforementioned diagnostic criteria are widely accepted.
DEFINITION OF PREDIABETES AND DIAGNOSTIC CRITERIA
Issues regarding IFG criteria
HbA1c criteria issues
- According to several epidemiological studies, the worldwide prevalence of preDM exceeds that of true diabetes. The prevalence of preDM is expected to increase, and factors related to race, age, and various characteristics related to gender are known to exist.
- Prevalence
- According to the IDF Diabetes Atlas, currently, the number of cases of IGT (2010) worldwide is estimated to be approximately 340 million [40,41]. North America has the highest prevalence of IGT in the world, with 10.4%. For Europe and the Middle East, the values are 8.9% and 8.2%, respectively, which is also relatively high versus other parts of the world [41]. In Southeast Asia and the Western Pacific Region, the prevalences are 6.2% and 7.7%, respectively [41]. However, according to the absolute differences in population size, the Western Pacific Region is estimated to have the largest number of IGT subjects, approximately 120 million people [41]. When compared with DM, the prevalence of IGT is generally similar; however, in North America, the prevalence of IGT is lower than that of DM. In Africa and the Western Pacific Region, IGT prevalence is slightly higher than that of diabetes [41]. By 2030, the global prevalence of IGT is estimated to reach 8.4%, which will be approximately 462 million people [41].
- There are no additional comprehensive global estimates of IGF prevalence; however, in most parts of the world, it is known that the prevalence is above 5% [2]. In 2002, an IGT/IFG consensus statement published by the International Diabetes Federation (IDF) stated that based on surveys conducted in many parts of the world, IGF prevalence was 2.0 to 17.3% [2]. Generally, the prevalence of IGT is known to be higher than that of IFG; however, these data were mostly based on the previous ADA/WHO criteria. According to the new ADA criteria, when the IFG cut-off value is adjusted to 100 mg/dL, IFG prevalence increases dramatically. In this case, the increase in IFG prevalence is greater than that of IGT [26,42]. For example, by changing the IFG diagnostic criteria, the Danish IFG prevalence increased from 11.8% to 37.6% [43]. Further, by changing the diagnostic criteria in DETECT-2 study subjects, IFG prevalence increased from 12.7% to 28.7% in Chinese subjects, from 11.0% to 38.6% in Asian Indians, from 16.3% to 45.7% in French subjects, and from 12.1% to 32.0% in the Unites States [44]. According to data from a survey on NHANES subjects, the IFG prevalence of Americans over the age of 20 was reported as 25.7% and IGT was reported as 13.8% [45].
- Overlap of IFG and IGT
- The issue with the IFG and IGT concept began with whether screening for diabetic high-risk groups should be performed using fasting blood glucose or postprandial blood glucose tests. However, subjects selected through IFG and IGT criteria were not identical.
- Generally, among subjects screened using IGT, only 20 to 25% of individuals have FPG levels ≥110 mg/dL. In subjects screened with IFG, <50% have a postprandial 2-hour glucose level ≥140 mg/dL [2]. In the DECODE studies, which examined European IFG subjects that were defined exclusively by FPG levels between 6.1 and 6.9 mmol/L, 64.8% of subjects had 'isolated' IFG, 28.6% showed combined IFG with IGT, and 6.6% were diagnosed with diabetes [2,46]. In the DECODA studies, 45.9% of Asian IFG subjects that were defined exclusively by FPG levels had 'isolated' IFG, 35.2% showed IFG values that were associated with IGT, and 18.9% had diabetes [47]. Even in the analyses of NHANES subjects, only some of the preDM subjects showed overlap between IGT and IFG. Using the ADA IFG criteria, 60% of all IGT subjects were screened; however, among subjects classified as IFG, only 18.5% of IGT subjects could be screened.
- These data suggest that screening for all high-risk diabetes groups is not possible through the simple methods of either fasting glucose or postprandial blood glucose. Additionally, these results show that across physiological conditions, there can be a significant difference between IFG and IGT.
- Characteristics of age and gender
- Differences in age and gender between IFG and IGT are known to exist depending on the populations and region investigated. Generally, the prevalence of IFG and IGT increases according to age. Additionally, while IFG prevalence is relatively high in men, it is lower in women [2]. In the DECODE studies, the prevalence of isolated IFG in men increased gradually with age. In the 50 to 59 age group, IFG decreased gradually after reaching a plateau of 10.1%. Additionally, when the over 70 group was excluded, prevalence in men was significantly higher [2,46,48]. The prevalence of isolated IGT increased continuously regardless of gender, and excluding the over 70 group, the prevalence in women of all ages was significantly higher [2,46]. In the DECODA studies in Asians, excluding Indian cohorts, isolated IFG and isolated IGT prevalence both tended to increase with age, but not gender [2,47]. Differences by gender were not significant when compared with Europeans. Further, the isolated IFG prevalence of women in the same age group was much higher than in men, and women had higher incidences of isolated IGT [2,47]. Even in NHANES subjects, the prevalence of IFG and IGT increased proportionally with age [45]. However, IFG prevalence in men was 32.1%, compared with 19.8% in women. There was no significant difference in IGT based on gender; IGT prevalence in men was 14.6% and 13.1% in women [45]. There was also no observed difference in the prevalence of preDM in NHANES subjects based on ethnic backgrounds [45].
- There are differences between target populations in the above large-scale epidemiological survey results, and an exact comparison between each is very difficult. Estimating incidence is not possible using a cross-sectional design. Furthermore, with the rapidly changing lifestyle habits observed in many Asian countries, there is a problem applying epidemiological characteristics longitudinally.
- The clinical course of preDM
- The risk for DM in preDM subjects is much higher compared with those with normal glucose tolerance (NGT). When several prospective epidemiological studies were compiled, the incidence of T2DM in isolated IFG and IGT subjects was estimated at 4 to 6% per year, and this value was significantly higher than NGT subjects (<0.5% per year) [5-7,13,16,49]. In the subjects who were diagnosed with IFG and IGT in combination, the annual percentage for the risk of developing T2DM increased by 10%. This suggests that IFG and IGT have additive roles in predicting the risk of developing T2DM. However, some preDM subjects also experienced complete recovery to normal glucose tolerance levels. In an 11-year follow-up study on Mauritius adults with IGT, 46% progressed into overt DM, 28% retained their condition, 4% changed to IFG, and 24% showed normalized glucose tolerance [16]. For patients with IFG, 38% developed overt DM, 7% experienced no change, 17% progressed to IGT, and 38% developed normalized glucose tolerance [16].
- The occurrence of cardiovascular disease and associated mortality in preDM subjects compared with normal glucose tolerance are known to be significantly elevated [25,50,51]. In several studies, the risk of cardiovascular disease in preDM patients compared with NGT increased by over 50%, and this risk was greater in young adults [25]. However, in each study, there were differences in the risks of developing cardiovascular disease between IFG and IGT, and when confounding variables were compensated for, the risk of developing cardiovascular disease was lowered [25]. As previously mentioned, in patients screened as having IFG based on the new ADA diagnostic criteria, and using the WHO criteria as a comparison, the cardiovascular risk profile is a little more favorable, and the risk of developing diabetes is known to be lower. There is much room for debate regarding IFG diagnostic criteria and the risk of developing cardiovascular disease [22-25].
EPIDEMIOLOGY OF PREDM
- Epidemiological studies examining a large number of subjects who were independently screened for both IFG and IGT suggest that the pathophysiological characteristics of IFG and IGT are significantly different [2]. The most important factors that may explain the pathophysiology of T2DM are increased insulin resistance and decreased insulin secretion. Studies analyzing insulin resistance and insulin secretion in isolated IFG and IGT subjects suggest that there are distinguishable characteristics between the subtypes [52-57]. However, differences in pathophysiology between each preDM subtypes still do not clarify whether these commonly shared phenomena occur in various regions or ethnicities around the world. Additionally, their significance in clinical practice is unknown.
- Perspectives on insulin resistance
- During glucose stimulation, pancreatic insulin secretion physiologically suppresses hepatic glucose production in the liver; however, glucose utilization is promoted in the peripheral tissues, including muscle and adipose tissue. Insulin resistance refers to a dysfunctional physiological response to insulin secretion in vivo. Despite normal or higher insulin levels, hepatic glucose production is not adequately suppressed, or a reduction in glucose utilization in peripheral tissue causes increased plasma glucose concentrations. Compared with NGT subjects, there is a significantly higher tendency for insulin resistance to increase in preDM subjects. Additionally, important differences in the mechanisms underlying insulin resistance are known to exist between preDM subtypes [42,52-55,57].
- Hepatic insulin resistance in IFG subjects is significantly higher than in NGT subjects. In contrast, peripheral insulin resistance is known to be significantly higher in IGT subjects [42,52,53,57]. Fasting blood glucose levels are significantly higher in basal hepatic glucose production in response to insulin in IFG subjects, despite hyperinsulinemia, compared with NGT subjects. These results suggest that proper suppression does not occur; however, hepatic insulin resistance eventually increases in IFG subjects [42,52,57]. In IGT subjects, hepatic insulin resistance is significantly lower than in IFG subjects; however, there is no significant difference compared with NGT [42,52,57]. In studies that use the euglycemic hyperinsulinemic clamp, the gold-standard for assessing insulin resistance, total body glucose disposal in isolated IGT subjects is significantly reduced compared with NGT, while in isolated IFG, it is similar to NGT [58,59]. In isolated IGT subjects, this significantly increases insulin resistance in peripheral tissues. In contrast, peripheral insulin resistance is not significantly different between isolated IFG and NGT. While IFG is associated with IGT, both hepatic and peripheral insulin resistance are significantly higher than NGT [42,52,55,57].
- Perspectives on insulin secretion
- The progressive failure of beta cells is the major factor underlying the development and progression of T2DM. Physiological pancreatic insulin secretion occurs biphasically. Generally, sharply increasing early phase secretion and late phase secretion can be divided by post-continuous glucose stimulation during initial glucose loading. Even if the same amount of glucose is loaded, differences in in vivo insulin secretion exist during the course of administration. When glucose is administered orally, insulin secretion promotion occurs via the additional effects of incretin; however, when glucose is delivered intravenously, this effect is not observed [55]. It is well-known that a reduction in insulin secretion due to beta cell failure is an early step in NGT and preDM stages. In addition to simple reduction in insulin secretion, however, differences in beta cell dysfunction patterns are known to exist between preDM subtypes [56,57,60].
- According to studies based on oral glucose tolerance tests, early phase insulin secretion in IFG subjects is significantly reduced compared with NGT, while late-phase insulin secretion is normal. Further, supranormal conditions can be observed [52,57]. On the other hand, early phase insulin secretion was relatively intact in IGT subjects, while late-phase insulin secretion was severely decreased [52,57]. In other studies, first- and second-phase insulin secretion in IGT subjects decreased in response to glucose infusion, while in IFG subjects, first-phase secretion decreased and second-phase insulin secretion remained relatively intact [54,55]. For both oral and intravenous glucose loads, symptoms of insulin secretion disorders in preDM subjects do not appear to be the result of incretin, but, instead, are caused by direct beta cell dysfunction. When IFG is accompanied by IGT, both early and late-phase insulin secretion were extremely reduced [52,57].
- Racial differences in the pathophysiological characteristics of preDM
- Based on the results discussed above, it seems clear that there is a difference between insulin resistance and insulin secretion between IFG and IGT subjects; however, most studies have targeted Caucasians, and there are not many studies that include physiological characteristics of other races, including Asians.
- Using a 75-g oral glucose tolerance test, differences between insulin secretion and insulin resistance have recently been compared according to preDM subtypes in 307 Korean subjects diagnosed with drug-naïve preDM [56]. 75-g oral glucose tolerance test results were classified according to ADA diagnostic criteria: 87 subjects had isolated IFG, 75 had isolated IGT, and 145 had both. Within the subjects, homeostasis model assessment of insulin resistance (HOMA-IR) represents hepatic insulin resistance, whole body insulin sensitivity index (WBISI; Matsuda index) represents peripheral insulin resistance, the insulinogenic index (IGI) represents early phase insulin secretion, AUC I/G0-120 represents late-phase insulin secretion, and insulin resistance effects are compensated for. To assess beta cell function, the disposition index (DI, IGI×WBISI), was measured [56]. After adjusting for confounding variables, it was found that HOMA-IR, IGI, AUC I/G0-120, and DI were high in isolated IFG subjects, while only WBISI was high in isolated IGT subjects (Fig. 1) [56]. Although the gold-standard was being used in this study, preDM pathophysiology increased insulin resistance in IFG and reduced insulin secretion in IGT. Additionally, there was an apparent difference among study results, which suggests that something else is playing a relatively important role [56]. In future, additional studies are required between each preDM subtype to determine the physiological characteristics in various regions around the world to confirm the most common racial characteristics.
- Do pathophysiological characteristics between preDM subtypes have clinical significance?
- It remains unclear as to how clinically important heterogeneous pathophysiological features are between the observed subtypes. In many of the previous prospective, randomized trials that used interventions such as lifestyle modification and pharmacological agents, the risk of developing T2DM decreased in preDM subjects and it is known that several cardiovascular risk factors can be significantly improved upon [5-7]. In previous studies, however, interventions according to preDM subtypes have considered distinct pathophysiological characteristics, which could not be tested in subjects. Although it is only a hypothesis, it is suspected that when medical interventions are made during preDM and the early phase of T2DM according to hepatic/peripheral insulin resistance-dominant phenotype recognition or beta cell dysfunction-dominant phenotype recognition, more positive clinical outcomes may be obtained. For example, metformin and TZDs are used as insulin sensitizers for hepatic/peripheral insulin resistance phenotypes. In contrast, for beta cell dysfunction phenotypes, GLP-1 antagonists are thought to be effective. Additional studies will be necessary to determine whether this hypothesis is accurate.
PATHOPHYSIOLOGY OF PREDM
- PreDM is an obvious risk factor for both T2DM and cardiovascular disease. However, there are almost no symptoms of preDM and the clinical course is variable. Because there is not a worldwide consensus on diagnostic criteria, there are inadequacies in defining it as a single disease. However, we feel that the prevalence of preDM is higher than that of T2DM, and there are many epidemiological characteristics involved in different regions and races. Compared with observable symptoms, physiologically dynamic changes are occurring. Through proper management, recovery of normal glucose tolerance is possible. Additionally, because complications can be prevented, the clinical approach is more aggressive and more time is required to develop a more systematic approach. This suggests that individual management is required given the observed significant pathophysiological heterogeneity between preDM subtypes for the management of preDM subjects. Through future research, the pathophysiology of preDM and early stage T2DM is expected to become much more widely understood.
CONCLUSIONS
-
Acknowledgements
- This article was supported by a grant from the Korea Health 21 R&D Project, Ministry of Health and Welfare, Republic of Korea (Grant No. A050463).
ACKNOWLEDGMENT
- 1. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2010;33(Suppl 1):S62-S69. ArticlePubMedPMCPDF
- 2. Unwin N, Shaw J, Zimmet P, Alberti KG. Impaired glucose tolerance and impaired fasting glycaemia: the current status on definition and intervention. Diabet Med 2002;19:708-723. ArticlePubMed
- 3. International Expert Committee. International Expert Committee report on the role of the A1C assay in the diagnosis of diabetes. Diabetes Care 2009;32:1327-1334. ArticlePubMedPMCPDF
- 4. American Diabetes Association. Standards of medical care in diabetes--2010. Diabetes Care 2010;33(Suppl 1):S11-S61. ArticlePubMedPMCPDF
- 5. Tuomilehto J, Lindstrom J, Eriksson JG, Valle TT, Hamalainen H, Ilanne-Parikka P, Keinanen-Kiukaanniemi S, Laakso M, Louheranta A, Rastas M, Salminen V, Uusitupa M. Finnish Diabetes Prevention Study Group. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med 2001;344:1343-1350. ArticlePubMed
- 6. Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, Nathan DM. Diabetes Prevention Program Research Group. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 2002;346:393-403. ArticlePubMedPMC
- 7. Pan XR, Li GW, Hu YH, Wang JX, Yang WY, An ZX, Hu ZX, Lin J, Xiao JZ, Cao HB, Liu PA, Jiang XG, Jiang YY, Wang JP, Zheng H, Zhang H, Bennett PH, Howard BV. Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance. The Da Qing IGT and Diabetes Study. Diabetes Care 1997;20:537-544. ArticlePubMedPDF
- 8. National Diabetes Data Group. Classification and diagnosis of diabetes mellitus and other categories of glucose intolerance. Diabetes 1979;28:1039-1057. ArticlePubMedPDF
- 9. Massari V, Eschwege E, Valleron AJ. Imprecision of new criteria for the oral glucose tolerance test. Diabetologia 1983;24:100-106. ArticlePubMedPDF
- 10. Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 1998;15:539-553. ArticlePubMed
- 11. Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 1997;20:1183-1197. ArticlePubMedPDF
- 12. Puavilai G, Chanprasertyotin S, Sriphrapradaeng A. Diagnostic criteria for diabetes mellitus and other categories of glucose intolerance: 1997 criteria by the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus (ADA), 1998 WHO consultation criteria, and 1985 WHO criteria. World Health Organization. Diabetes Res Clin Pract 1999;44:21-26. PubMed
- 13. Gabir MM, Hanson RL, Dabelea D, Imperatore G, Roumain J, Bennett PH, Knowler WC. The 1997 American Diabetes Association and 1999 World Health Organization criteria for hyperglycemia in the diagnosis and prediction of diabetes. Diabetes Care 2000;23:1108-1112. ArticlePubMedPDF
- 14. Genuth S, Alberti KG, Bennett P, Buse J, Defronzo R, Kahn R, Kitzmiller J, Knowler WC, Lebovitz H, Lernmark A, Nathan D, Palmer J, Rizza R, Saudek C, Shaw J, Steffes M, Stern M, Tuomilehto J, Zimmet P. Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Follow-up report on the diagnosis of diabetes mellitus. Diabetes Care 2003;26:3160-3167. ArticlePubMedPDF
- 15. Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 2003;26(Suppl 1):S5-S20. ArticlePubMedPDF
- 16. Shaw JE, Zimmet PZ, de Courten M, Dowse GK, Chitson P, Gareeboo H, Hemraj F, Fareed D, Tuomilehto J, Alberti KG. Impaired fasting glucose or impaired glucose tolerance. What best predicts future diabetes in Mauritius? Diabetes Care 1999;22:399-402. ArticlePubMedPDF
- 17. Hanley AJ, Williams K, Gonzalez C, D'Agostino RB Jr, Wagenknecht LE, Stern MP, Haffner SM. San Antonio Heart Study. Mexico City Diabetes Study. Insulin Resistance Atherosclerosis Study. Prediction of type 2 diabetes using simple measures of insulin resistance: combined results from the San Antonio Heart Study, the Mexico City Diabetes Study, and the Insulin Resistance Atherosclerosis Study. Diabetes 2003;52:463-469. PubMed
- 18. de Vegt F, Dekker JM, Jager A, Hienkens E, Kostense PJ, Stehouwer CD, Nijpels G, Bouter LM, Heine RJ. Relation of impaired fasting and postload glucose with incident type 2 diabetes in a Dutch population: The Hoorn Study. JAMA 2001;285:2109-2113. ArticlePubMed
- 19. World Health Organization. Definition and diagnosis of diabetes mellitus and intermediate hyperglycemia: report of a WHO/IDF consultation. 2006. Geneva: World Health Organization.
- 20. Tirosh A, Shai I, Tekes-Manova D, Israeli E, Pereg D, Shochat T, Kochba I, Rudich A. Israeli Diabetes Research Group. Normal fasting plasma glucose levels and type 2 diabetes in young men. N Engl J Med 2005;353:1454-1462. ArticlePubMed
- 21. Schmidt MI, Duncan BB, Bang H, Pankow JS, Ballantyne CM, Golden SH, Folsom AR, Chambless LE. Atherosclerosis Risk in Communities Investigators. Identifying individuals at high risk for diabetes: The Atherosclerosis Risk in Communities study. Diabetes Care 2005;28:2013-2018. PubMed
- 22. Forouhi NG, Balkau B, Borch-Johnsen K, Dekker J, Glumer C, Qiao Q, Spijkerman A, Stolk R, Tabac A, Wareham NJ. EDEG. The threshold for diagnosing impaired fasting glucose: a position statement by the European Diabetes Epidemiology Group. Diabetologia 2006;49:822-827. ArticlePubMedPDF
- 23. Levitan EB, Song Y, Ford ES, Liu S. Is nondiabetic hyperglycemia a risk factor for cardiovascular disease? A meta-analysis of prospective studies. Arch Intern Med 2004;164:2147-2155. ArticlePubMed
- 24. DECODE Study Group, European Diabetes Epidemiology Group. Is the current definition for diabetes relevant to mortality risk from all causes and cardiovascular and noncardiovascular diseases? Diabetes Care 2003;26:688-696. ArticlePubMedPDF
- 25. Ford ES, Zhao G, Li C. Pre-diabetes and the risk for cardiovascular disease: a systematic review of the evidence. J Am Coll Cardiol 2010;55:1310-1317. PubMed
- 26. Davidson MB, Landsman PB, Alexander CM. Lowering the criterion for impaired fasting glucose will not provide clinical benefit. Diabetes Care 2003;26:3329-3330. ArticlePubMedPDF
- 27. Saudek CD, Herman WH, Sacks DB, Bergenstal RM, Edelman D, Davidson MB. A new look at screening and diagnosing diabetes mellitus. J Clin Endocrinol Metab 2008;93:2447-2453. ArticlePubMedPDF
- 28. Wong TY, Liew G, Tapp RJ, Schmidt MI, Wang JJ, Mitchell P, Klein R, Klein BE, Zimmet P, Shaw J. Relation between fasting glucose and retinopathy for diagnosis of diabetes: three population-based cross-sectional studies. Lancet 2008;371:736-743. ArticlePubMedPMC
- 29. Sabanayagam C, Liew G, Tai ES, Shankar A, Lim SC, Subramaniam T, Wong TY. Relationship between glycated haemoglobin and microvascular complications: is there a natural cut-off point for the diagnosis of diabetes? Diabetologia 2009;52:1279-1289. ArticlePubMedPDF
- 30. Weykamp C, John WG, Mosca A, Hoshino T, Little R, Jeppsson JO, Goodall I, Miedema K, Myers G, Reinauer H, Sacks DB, Slingerland R, Siebelder C. The IFCC Reference Measurement System for HbA1c: a 6-year progress report. Clin Chem 2008;54:240-248. ArticlePubMedPDF
- 31. Tominaga M, Makino H, Yoshino G, Kuwa K, Takei I, Aono Y, Hoshino T, Umemoto M, Shimatsu A, Sanke T, Kuwashima M, Taminato T, Ono J. Japanese standard reference material for JDS Lot 2 haemoglobin A1c. I: comparison of Japan Diabetes Society-assigned values to those obtained by the Japanese and USA domestic standardization programmes and by the International Federation of Clinical Chemistry reference laboratories. Ann Clin Biochem 2005;42(Pt 1):41-46. ArticlePubMedPDF
- 32. Bennett CM, Guo M, Dharmage SC. HbA(1c) as a screening tool for detection of type 2 diabetes: a systematic review. Diabet Med 2007;24:333-343. ArticlePubMed
- 33. Nakagami T, Tominaga M, Nishimura R, Yoshiike N, Daimon M, Oizumi T, Tajima N. Is the measurement of glycated hemoglobin A1c alone an efficient screening test for undiagnosed diabetes? Japan National Diabetes Survey. Diabetes Res Clin Pract 2007;76:251-256. PubMed
- 34. Herman WH, Engelgau MM, Zhang Y, Brown MB. Use of GHb (HbA(1c)) to screen for undiagnosed diabetes in the US population. Diabetes Care 2000;23:1207-1208. ArticlePubMedPDF
- 35. Rohlfing CL, Wiedmeyer HM, Little RR, England JD, Tennill A, Goldstein DE. Defining the relationship between plasma glucose and HbA(1c): analysis of glucose profiles and HbA(1c) in the Diabetes Control and Complications Trial. Diabetes Care 2002;25:275-278. PubMed
- 36. Droumaguet C, Balkau B, Simon D, Caces E, Tichet J, Charles MA, Eschwege E. DESIR Study Group. Use of HbA1c in predicting progression to diabetes in French men and women: data from an Epidemiological Study on the Insulin Resistance Syndrome (DESIR). Diabetes Care 2006;29:1619-1625. PubMed
- 37. Buell C, Kermah D, Davidson MB. Utility of A1C for diabetes screening in the 1999 2004 NHANES population. Diabetes Care 2007;30:2233-2235. ArticlePubMedPDF
- 38. Pradhan AD, Rifai N, Buring JE, Ridker PM. Hemoglobin A1c predicts diabetes but not cardiovascular disease in nondiabetic women. Am J Med 2007;120:720-727. ArticlePubMedPMC
- 39. Sato KK, Hayashi T, Harita N, Yoneda T, Nakamura Y, Endo G, Kambe H. Combined measurement of fasting plasma glucose and A1C is effective for the prediction of type 2 diabetes: the Kansai Healthcare Study. Diabetes Care 2009;32:644-646. PubMedPMC
- 40. Unwin N, Gan D, Whiting D. The IDF Diabetes Atlas: providing evidence, raising awareness and promoting action. Diabetes Res Clin Pract 2010;87:2-3. ArticlePubMed
- 41. International Diabetes Federation (IDF). IDF diabetes atlas. 2010. 4th ed. Brussels: IDF Executive Office.
- 42. Abdul-Ghani MA, DeFronzo RA. Pathophysiology of prediabetes. Curr Diab Rep 2009;9:193-199. ArticlePubMedPDF
- 43. Glumer C, Jorgensen T, Borch-Johnsen K. Inter99 study. Prevalences of diabetes and impaired glucose regulation in a Danish population: the Inter99 study. Diabetes Care 2003;26:2335-2340. PubMed
- 44. Borch-Johnsen K, Colagiuri S, Balkau B, Glumer C, Carstensen B, Ramachandran A, Dong Y, Gao W. Creating a pandemic of prediabetes: the proposed new diagnostic criteria for impaired fasting glycaemia. Diabetologia 2004;47:1396-1402. ArticlePubMedPDF
- 45. Cowie CC, Rust KF, Ford ES, Eberhardt MS, Byrd-Holt DD, Li C, Williams DE, Gregg EW, Bainbridge KE, Saydah SH, Geiss LS. Full accounting of diabetes and pre-diabetes in the U.S. population in 1988-1994 and 2005-2006. Diabetes Care 2009;32:287-294. ArticlePubMedPMCPDF
- 46. DECODE Study Group on behalf of the European Diabetes Epidemiology Study Group. Will new diagnostic criteria for diabetes mellitus change phenotype of patients with diabetes? Reanalysis of European epidemiological data. BMJ 1998;317:371-375. ArticlePubMedPMC
- 47. Qiao Q, Hu G, Tuomilehto J, Nakagami T, Balkau B, Borch-Johnsen K, Ramachandran A, Mohan V, Iyer SR, Tominaga M, Kiyohara Y, Kato I, Okubo K, Nagai M, Shibazaki S, Yang Z, Tong Z, Fan Q, Wang B, Chew SK, Tan BY, Heng D, Emmanuel S, Tajima N, Iwamoto Y, Snehalatha C, Vijay V, Kapur A, Dong Y, Nan H, Gao W, Shi H, Fu F. DECODA Study Group. Age- and sex-specific prevalence of diabetes and impaired glucose regulation in 11 Asian cohorts. Diabetes Care 2003;26:1770-1780. ArticlePubMedPDF
- 48. The DECODE study group, European Diabetes Epidemiology Group, Diabetes Epidemiology: Collaborative analysis Of Diagnostic criteria in Europe. Glucose tolerance and mortality: comparison of WHO and American Diabetes Association diagnostic criteria. Lancet 1999;354:617-621. PubMed
- 49. de Vegt F, Dekker JM, Stehouwer CD, Nijpels G, Bouter LM, Heine RJ. The 1997 American Diabetes Association criteria versus the 1985 World Health Organization criteria for the diagnosis of abnormal glucose tolerance: poor agreement in the Hoorn Study. Diabetes Care 1998;21:1686-1690. ArticlePubMedPDF
- 50. Coutinho M, Gerstein HC, Wang Y, Yusuf S. The relationship between glucose and incident cardiovascular events. A metaregression analysis of published data from 20 studies of 95,783 individuals followed for 12.4 years. Diabetes Care 1999;22:233-240. ArticlePubMedPDF
- 51. Saydah SH, Miret M, Sung J, Varas C, Gause D, Brancati FL. Postchallenge hyperglycemia and mortality in a national sample of U.S. adults. Diabetes Care 2001;24:1397-1402. ArticlePubMedPDF
- 52. Abdul-Ghani MA, Jenkinson CP, Richardson DK, Tripathy D, DeFronzo RA. Insulin secretion and action in subjects with impaired fasting glucose and impaired glucose tolerance: results from the Veterans Administration Genetic Epidemiology Study. Diabetes 2006;55:1430-1435. PubMed
- 53. Meyer C, Pimenta W, Woerle HJ, Van Haeften T, Szoke E, Mitrakou A, Gerich J. Different mechanisms for impaired fasting glucose and impaired postprandial glucose tolerance in humans. Diabetes Care 2006;29:1909-1914. ArticlePubMedPDF
- 54. Perreault L, Bergman BC, Playdon MC, Dalla Man C, Cobelli C, Eckel RH. Impaired fasting glucose with or without impaired glucose tolerance: progressive or parallel states of prediabetes? Am J Physiol Endocrinol Metab 2008;295:E428-E435. ArticlePubMedPMC
- 55. Faerch K, Vaag A, Holst JJ, Glumer C, Pedersen O, Borch-Johnsen K. Impaired fasting glycaemia vs impaired glucose tolerance: similar impairment of pancreatic alpha and beta cell function but differential roles of incretin hormones and insulin action. Diabetologia 2008;51:853-861. ArticlePubMedPDF
- 56. Rhee SY, Woo JT, Chon S, Hwang YC, Oh S, Ahn KJ, Chung HY, Kim SW, Kim JW, Kim YS. Characteristics of insulin resistance and insulin secretory capacity in Korean subjects with IFG and IGT. Diabetes Res Clin Pract 2010;89:250-255. ArticlePubMed
- 57. Faerch K, Vaag A, Holst JJ, Hansen T, Jorgensen T, Borch-Johnsen K. Natural history of insulin sensitivity and insulin secretion in the progression from normal glucose tolerance to impaired fasting glycemia and impaired glucose tolerance: the Inter99 study. Diabetes Care 2009;32:439-444. ArticlePubMedPMCPDF
- 58. Weyer C, Bogardus C, Pratley RE. Metabolic characteristics of individuals with impaired fasting glucose and/or impaired glucose tolerance. Diabetes 1999;48:2197-2203. ArticlePubMedPDF
- 59. Wasada T, Kuroki H, Katsumori K, Arii H, Sato A, Aoki K. Who are more insulin resistant, people with IFG or people with IGT? Diabetologia 2004;47:758-759. ArticlePubMedPDF
- 60. Rhee SY, Kim JY, Chon S, Hwang YC, Jeong IK, Oh S, Ahn KJ, Chung HY, Woo J, Kim SW, Kim JW, Kim YS. The changes in early phase insulin secretion in newly diagnosed, drug naïve Korean prediabetes subjects. Korean Diabetes J 2010;34:157-165. ArticlePubMedPMC
REFERENCES
Fig. 1Comparison of insulin resistance and secretory indices between Korean prediabetic subjects after adjusting for age, gender, body mass index, and abdominal circumference [56]. Data are presented as mean±standard error. HOMA-IR, homeostasis model assessment of insulin resistance; IFG, impaired fasting glucose; IGT, impaired glucose tolerance; WBISI, whole body insulin sensitivity index; IGI, insulinogenic index. aP<0.05, bP<0.01.
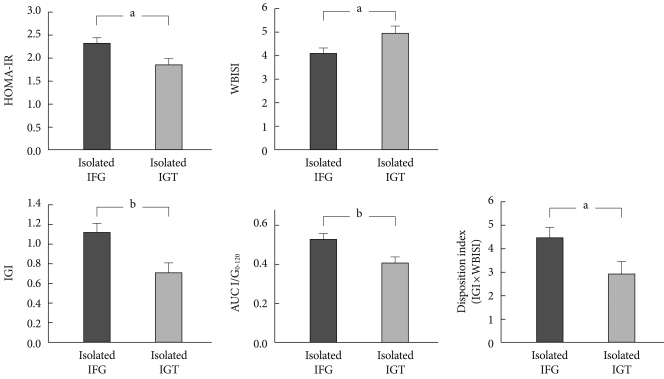

Figure & Data
References
Citations
Citations to this article as recorded by 

- Comparison of triglyceride/glucose index and related parameters with Indian Diabetes Risk Score assessment in non-diabetic individuals visiting primary healthcare centre—A community-based cross-sectional study
Sivapragasam Ramalingam, Amlan Kumar Kar, Rajini Senthil
Journal of Family Medicine and Primary Care.2024; 13(1): 235. CrossRef - Are HOMA-IR and HOMA-B good predictors for diabetes and pre-diabetes subtypes?
Davood Khalili, Marjan Khayamzadeh, Karim Kohansal, Noushin Sadat Ahanchi, Mitra Hasheminia, Farzad Hadaegh, Maryam Tohidi, Fereidoun Azizi, Ali Siamak Habibi-Moeini
BMC Endocrine Disorders.2023;[Epub] CrossRef - Finnish diabetes risk score outperformed triglyceride-glucose index in diabetes risk prediction
Anthony Chibuzor Nnamudi, Noghayin Jerry Orhue, Ifeoma Irene Ijeh, Amarachi Nene Nwabueze
Journal of Diabetes & Metabolic Disorders.2023; 22(2): 1337. CrossRef - Predictive value of triglycerides to high-density lipoprotein cholesterol and triglyceride glycemic index for diabetes incidence in pre-diabetes patients: a prospective cohort study
Mehdi Sharafi, Zahra Amiri, Babak Pezeshki, Mohammad Ali Mohsenpour, Mohammad Hassan Eftekhari, Sima Afrashteh, Elham Haghjoo, Akram Farhadi, Mohsen Khaleghi, Zahra Mastaneh
Journal of Health, Population and Nutrition.2023;[Epub] CrossRef - Triglyceride glucose index for the detection of the severity of coronary artery disease in different glucose metabolic states in patients with coronary heart disease: a RCSCD-TCM study in China
Jinyu Su, Zhu Li, Mengnan Huang, Yang Wang, Tong Yang, Mei Ma, Tongyao Ni, Guangwei Pan, Ziqin Lai, Chunjie Li, Lin Li, Chunquan Yu
Cardiovascular Diabetology.2022;[Epub] CrossRef - The triglyceride-glucose index, a predictor of type 2 diabetes development: A retrospective cohort study
Panya Chamroonkiadtikun, Thareerat Ananchaisarp, Worawit Wanichanon
Primary Care Diabetes.2020; 14(2): 161. CrossRef - Undiagnosed prediabetes status is associated with a reduced effectiveness of phosphodiesterase type 5 inhibitors in men with erectile dysfunction
Luca Boeri, Paolo Capogrosso, Eugenio Ventimiglia, Edoardo Pozzi, Francesco Chierigo, Federico Belladelli, Rani Zuabi, Nicolò Schifano, Costantino Abbate, Federico Dehò, Emanuele Montanari, Francesco Montorsi, Andrea Salonia
International Journal of Impotence Research.2020; 32(4): 393. CrossRef - Modifiable risk factors associated with non-communicable diseases among adult outpatients in Manzini, Swaziland: a cross-sectional study
Mojeed Akorede Gbadamosi, Boikhutso Tlou
BMC Public Health.2020;[Epub] CrossRef - Effect of a family and interdisciplinary intervention to prevent T2D: randomized clinical trial
Katya Vargas-Ortiz, Georgina Lira-Mendiola, Claudia M. Gómez-Navarro, Katya Padilla-Estrada, Fabiola Angulo-Romero, José M. Hernández-Márquez, Ana K. Villa-Martínez, Jessica N. González-Mena, Maciste H. Macías-Cervantes, Maria de Lourdes Reyes-Escogido, R
BMC Public Health.2020;[Epub] CrossRef - Sexual Dysfunction in Men with Prediabetes
Luca Boeri, Paolo Capogrosso, Eugenio Ventimiglia, Nicolò Schifano, Emanuele Montanari, Francesco Montorsi, Andrea Salonia
Sexual Medicine Reviews.2020; 8(4): 622. CrossRef - The ratio of estimated average glucose to fasting plasma glucose level as an indicator of insulin resistance in young adult diabetes
Jun Guo, Sisi Lei, Yu Zhou, Congqing Pan
Medicine.2020; 99(40): e22337. CrossRef - Health risks and interventions in prediabetes: A review
Roshan Kumar Mahat, Neelima Singh, Manisha Arora, Vedika Rathore
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2019; 13(4): 2803. CrossRef - Hospital-Based Korean Diabetes Prevention Study: A Prospective, Multi-Center, Randomized, Open-Label Controlled Study
Sang Youl Rhee, Suk Chon, Kyu Jeung Ahn, Jeong-Taek Woo
Diabetes & Metabolism Journal.2019; 43(1): 49. CrossRef - Nutraceuticals: Reviewing their Role in Chronic Disease Prevention and Management
Amanda Bergamin, Evangeline Mantzioris, Giordana Cross, Permal Deo, Sanjay Garg, Alison M. Hill
Pharmaceutical Medicine.2019; 33(4): 291. CrossRef - Prediabetes awareness among Southeastern European physicians
Visnja Kokic, Slaven Kokic, Mladen Krnic, Marin Petric, Ana Marija Liberati, Petra Simac, Tatjana Milenkovic, Vesna Capkun, Dario Rahelic, Kristina Blaslov
Journal of Diabetes Investigation.2018; 9(3): 544. CrossRef - Unrecognized Prediabetes Is Highly Prevalent in Men With Erectile Dysfunction–Results From a Cross-Sectional Study
Luca Boeri, Paolo Capogrosso, Filippo Pederzoli, Eugenio Ventimiglia, Nicola Frego, Francesco Chierigo, Emanuele Montanari, Francesco Montorsi, Andrea Salonia
The Journal of Sexual Medicine.2018; 15(8): 1117. CrossRef - Metformin exerts anti-obesity effect via gut microbiome modulation in prediabetics: A hypothesis
Kunal Maniar, Amal Moideen, Rajasri Bhattacharyya, Dibyajyoti Banerjee
Medical Hypotheses.2017; 104: 117. CrossRef - An association between bone mineral density and anabolic hormones in middle-aged and elderly men with prediabetes
Michał Rabijewski, Lucyna Papierska, Paweł Piątkiewicz
The Aging Male.2017; : 1. CrossRef - The Relationships between Anabolic Hormones and Body Composition in Middle-Aged and Elderly Men with Prediabetes: A Cross-Sectional Study
Michał Rabijewski, Lucyna Papierska, Paweł Piątkiewicz
Journal of Diabetes Research.2016; 2016: 1. CrossRef - Triglyceride glucose-waist circumference, a novel and effective predictor of diabetes in first-degree relatives of type 2 diabetes patients: cross-sectional and prospective cohort study
Shuang Zheng, Sheng Shi, Xingxing Ren, Tingting Han, Yangxue Li, Yawen Chen, Wei Liu, Peter C. Hou, Yaomin Hu
Journal of Translational Medicine.2016;[Epub] CrossRef - Glucose-Dependent Insulinotropic Peptide Level Is Associated with the Development of Type 2 Diabetes Mellitus
Sunghwan Suh, Mi Yeon Kim, Soo Kyoung Kim, Kyu Yeon Hur, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
Endocrinology and Metabolism.2016; 31(1): 134. CrossRef - Predictive Value of Glucose Parameters Obtained From Oral Glucose Tolerance Tests in Identifying Individuals at High Risk for the Development of Diabetes in Korean Population
Hae Kyung Yang, Hee-Sung Ha, Marie Rhee, Jin-Hee Lee, Yong-Moon Park, Hyuk-Sang Kwon, Hyeon-Woo Yim, Moo-Il Kang, Won-Chul Lee, Ho-Young Son, Seung-Hwan Lee, Kun-Ho Yoon
Medicine.2016; 95(10): e3053. CrossRef - Alteraciones glucémicas en los pacientes con enfermedad renal crónica
G. De’Marziani, G. Soler Pujol, L.M. Obregón, E.M. Morales, C.D. Gonzalez, L. Gonzalez Paganti, L. Cacciagiú, G. Lopez, L. Schreier, A. Elbert
Nefrología.2016; 36(2): 133. CrossRef - Glycaemic changes in patients with chronic kidney disease
Guillermo De’Marziani, Gervasio Soler Pujol, Liliana Miriam Obregón, Elisa Mabel Morales, Claudio Daniel Gonzalez, Luciana Gonzalez Paganti, Leonardo Cacciagiú, Graciela Lopez, Laura Schreier, Alicia Elbert
Nefrología (English Edition).2016; 36(2): 133. CrossRef - Reduction of postprandial blood glucose in healthy subjects by buns and flatbreads incorporated with fenugreek seed powder
Sathyasurya Daniel Robert, Aziz Al-safi Ismail, Wan Ishak Wan Rosli
European Journal of Nutrition.2016; 55(7): 2275. CrossRef - 1,5-Anhydroglucitol Is Associated with Early-Phase Insulin Secretion in Chinese Patients with Newly Diagnosed Type 2 Diabetes Mellitus
Xiaojing Ma, Yaping Hao, Xiang Hu, Yuqi Luo, Zixuan Deng, Jian Zhou, Yuqian Bao, Weiping Jia
Diabetes Technology & Therapeutics.2015; 17(5): 320. CrossRef - The product of triglycerides and glucose in comparison with fasting plasma glucose did not improve diabetes prediction
Mohsen Janghorbani, Siedeh Zinab Almasi, Masoud Amini
Acta Diabetologica.2015; 52(4): 781. CrossRef - Serum prostate-specific antigen levels in men with prediabetes: A cross-sectional study
Ao Sun, Rui Liu, Guangshan Sun
Scandinavian Journal of Clinical and Laboratory Investigation.2015; 75(3): 273. CrossRef - The Glycated Albumin to Glycated Hemoglobin Ratio Might Not Be Associated with Carotid Atherosclerosis in Patients with Type 1 Diabetes
Wonjin Kim, Kwang Joon Kim, Byung-Wan Lee, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee
Diabetes & Metabolism Journal.2014; 38(6): 456. CrossRef - Predicting the Development of Diabetes Using the Product of Triglycerides and Glucose: The Chungju Metabolic Disease Cohort (CMC) Study
Seung-Hwan Lee, Hyuk-Sang Kwon, Yong-Moon Park, Hee-Sung Ha, Seung Hee Jeong, Hae Kyung Yang, Jin-Hee Lee, Hyeon-Woo Yim, Moo-Il Kang, Won-Chul Lee, Ho-Young Son, Kun-Ho Yoon, Maria Eugenia Saez
PLoS ONE.2014; 9(2): e90430. CrossRef - The effect of insulin resistance on postprandial triglycerides in Korean type 2 diabetic patients
Kyeong Hye Park, Kwang Joon Kim, Byung-Wan Lee, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee
Acta Diabetologica.2014; 51(1): 15. CrossRef - Using a Participatory Research Approach in a School-Based Physical Activity Intervention to Prevent Diabetes in the Hualapai Indian Community, Arizona, 2002–2006
Nicolette I. Teufel-Shone, Michelle Gamber, Helen Watahomigie, T. J. Siyuja, Laurie Crozier, Sandra L. Irwin
Preventing Chronic Disease.2014;[Epub] CrossRef - Proinflammatory and Prothrombotic State in Subjects with Different Glucose Tolerance Status before Cardiovascular Disease
Irma Isordia-Salas, María Eugenia Galván-Plata, Alfredo Leaños-Miranda, Eberth Aguilar-Sosa, Francisco Anaya-Gómez, Abraham Majluf-Cruz, David Santiago-Germán
Journal of Diabetes Research.2014; 2014: 1. CrossRef - mRNA Expression of IGF-1 and IGF-1R in Patients with Colorectal Adenocarcinoma and Type 2 Diabetes
Rui Liu, Li-Ling Hu, Ao Sun, Ya-Jing Cao, Tao Tang, Xi-Peng Zhang, Qing-Huai Zhang
Archives of Medical Research.2014; 45(4): 318. CrossRef - Postprandial C‐peptide to glucose ratio as a predictor of β‐cell function and its usefulness for staged management of type 2 diabetes
Eun Young Lee, Sena Hwang, Seo Hee Lee, Yong‐ho Lee, A Ra Choi, Youngki Lee, Byung‐Wan Lee, Eun Seok Kang, Chul Woo Ahn, Bong Soo Cha, Hyun Chul Lee
Journal of Diabetes Investigation.2014; 5(5): 517. CrossRef -
The glycemic efficacies of insulin analogue regimens according to baseline glycemic status in Korean patients with type 2 diabetes: sub‐analysis from the A
1
chieve
®
study
Y.‐C. Hwang, J. G. Kang, K. J. Ahn, B. S. Cha, S.‐H. Ihm, S. Lee, M. Kim, B.‐W. Lee
International Journal of Clinical Practice.2014; 68(11): 1338. CrossRef - Tolerability, effectiveness and predictive parameters for the therapeutic usefulness of exenatide in obese, Korean patients with type 2 diabetes
Sun Ok Song, Kwang Joon Kim, Byung‐Wan Lee, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee
Journal of Diabetes Investigation.2014; 5(5): 554. CrossRef - Coronary Risk Estimation according to the Framingham-Wilson Score and Impaired Fasting Glucose in Adult Subjects from Maracaibo city, Venezuela
Bermúdez Valmore, Rojas Joselyn, Salazar Juan, González Robys, Martínez María Sofía, Chávez Carmen, Palacio Marcos, Rojas Edward, Cabrera Mayela, Miranda José López
Global Journal of Obesity, Diabetes and Metabolic Syndrome.2014; 1(1): 020. CrossRef - Serum glycated albumin as a new glycemic marker in pediatric diabetes
Ji Woo Lee, Hyung Jin Kim, Young Se Kwon, Yong Hoon Jun, Soon Ki Kim, Jong Weon Choi, Ji Eun Lee
Annals of Pediatric Endocrinology & Metabolism.2013; 18(4): 208. CrossRef - Prediabetes Is Associated with a High-Risk Colorectal Adenoma
Jae Myung Cha, Joung Il Lee, Kwang Ro Joo, Hyun Phil Shin, Jung Won Jeun, Jun Uk Lim
Digestive Diseases and Sciences.2013; 58(7): 2061. CrossRef - The lipid accumulation product as a useful index for identifying abnormal glucose regulation in young Korean women
J.‐Y. Oh, Y.‐A. Sung, H. J. Lee
Diabetic Medicine.2013; 30(4): 436. CrossRef - Glycemic Effectiveness of Metformin-Based Dual-Combination Therapies with Sulphonylurea, Pioglitazone, or DPP4-Inhibitor in Drug-Naïve Korean Type 2 Diabetic Patients
Young Ki Lee, Sun Ok Song, Kwang Joon Kim, Yongin Cho, Younjeong Choi, Yujung Yun, Byung-Wan Lee, Eun-Seok Kang, Bong Soo Cha, Hyun Chul Lee
Diabetes & Metabolism Journal.2013; 37(6): 465. CrossRef - Clinical characteristics and insulin independence of Koreans with new‐onset type 2 diabetes presenting with diabetic ketoacidosis
H. Seok, C. H. Jung, S. W. Kim, M. J. Lee, W. J. Lee, J. H. Kim, B‐W. Lee
Diabetes/Metabolism Research and Reviews.2013; 29(6): 507. CrossRef - Prevalence of chronic kidney disease and prediabetes and associated risk factors: a community-based screening in Zhuhai, Southern China
Dong-feng GU, Yan-lin SHI, You-ming CHEN, Hong-mei LIU, Ya-nan DING, Xin-yu LIU, Yong-qiang LI, Xiao-fei SHAO, Yan LIANG, Ying-shan CHEN, Zhi-yong YUAN, He-qun ZOU
Chinese Medical Journal.2013; 126(7): 1213. CrossRef - Post-Renal Transplant Diabetes Mellitus in Korean Subjects: Superimposition of Transplant-Related Immunosuppressant Factors on Genetic and Type 2 Diabetic Risk Factors
Hyun Chul Lee
Diabetes & Metabolism Journal.2012; 36(3): 199. CrossRef - Hormonal Association and Sexual Dysfunction in Patients with Impaired Fasting Glucose: A Cross-Sectional and Longitudinal Study
Giovanni Corona, Giulia Rastrelli, Giancarlo Balercia, Francesco Lotti, Alessandra Sforza, Matteo Monami, Gianni Forti, Edoardo Mannucci, Mario Maggi
The Journal of Sexual Medicine.2012; 9(6): 1669. CrossRef - Physical Activity among Veterans and Nonveterans with Diabetes
Erin D. Bouldin, Gayle E. Reiber
Journal of Aging Research.2012; 2012: 1. CrossRef - The ratio of glycated albumin to glycated haemoglobin correlates with insulin secretory function
Daham Kim, Kwang J. Kim, Ji H. Huh, Byung‐Wan Lee, Eun S. Kang, Bong S. Cha, Hyun C. Lee
Clinical Endocrinology.2012; 77(5): 679. CrossRef - Higher Morning to Evening Ratio in Total Dose of Twice-Daily Biphasic Insulin Analog Might Be Effective in Achieving Glucose Control in Patients with Poorly Controlled Type 2 Diabetes
Yong-Ho Lee, Byung-Wan Lee, Hea Jin Kwon, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee
Diabetes Technology & Therapeutics.2012; 14(6): 508. CrossRef - Human Monoclonal Antibodies against Glucagon Receptor Improve Glucose Homeostasis by Suppression of Hepatic Glucose Output in Diet-Induced Obese Mice
Wook-Dong Kim, Yong-ho Lee, Min-Hee Kim, Sun-Young Jung, Woo-Chan Son, Seon-Joo Yoon, Byung-Wan Lee, Nigel Irwin
PLoS ONE.2012; 7(12): e50954. CrossRef - The Risk of Bladder Cancer in Korean Diabetic Subjects Treated with Pioglitazone
Sun Ok Song, Kwang Joon Kim, Byung-Wan Lee, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee
Diabetes & Metabolism Journal.2012; 36(5): 371. CrossRef - Korean Red Ginseng (Panax ginseng) Improves Insulin Sensitivity in High Fat Fed Sprague‐Dawley Rats
Seo Hee Lee, Hyun Joo Lee, Yong‐ho Lee, Byung‐Wan Lee, Bong Soo Cha, Eun Seok Kang, Chul Woo Ahn, Jong Sook Park, Hyo Jeong Kim, Eun Young Lee, Hyun Chul Lee
Phytotherapy Research.2012; 26(1): 142. CrossRef - Latent Autoimmune Diabetes in Adults: Autoimmune Diabetes in Adults with Slowly Progressive β-cell Failure
Hannah Seok, Byung Wan Lee
Diabetes & Metabolism Journal.2012; 36(2): 116. CrossRef

 KDA
KDA PubReader
PubReader Cite
Cite




